Questions For Your Doctor
You may want to write down a list of questions before your appointment, so you can make sure you ask your doctor everything you want to. It can also help to have a friend or family member with you to help you get the answers you want.
Some possible questions are:
- What’s the best treatment for me?
- How often should I see a doctor for my condition?
- Do I need to see a specialist?
- When should I go to the emergency room?
- Do I need to limit the salt or fluids in my diet?
- What kind of exercise can I do?
- Are there any activities I should stay away from?
- Should I get a pneumonia vaccine and a flu shot?
Copd With Pulmonary Hypertension
Pulmonary hypertension is a lung disease characterized by high blood pressure in the pulmonary arteries. PH causes the pulmonary arteries, which are responsible for carrying blood from the heart to the lungs, to become narrowed and blocked. The disease often affects the right side of the heart since the right ventricle is responsible for pumping blood to the lungs unlike the left heart ventricle that pumps blood to the rest of the body. In PH, because the heart needs to work harder to pump blood through the right ventricle, it becomes enlarged and weakened.
Shortness of breath , fatigue, dizziness or fainting spells , pressure or pain in the chest, swelling in the ankles, legs and abdomen , a bluish color in the lips and skin and irregular heart beat are common symptoms of the disease, all of which can result in right heart failure and death. There is no cure for pulmonary hypertension and suffering from another disease, such as chronic obstructive pulmonary disease , can exacerbate it.
Symptoms Of Pulmonary Hypertension
Pulmonary hypertension may not cause any symptoms at first. Often, shortness of breath or lightheadedness during activity is the first symptom. As the disease gets worse, symptoms can include the following:
- Increased shortness of breath, with or without activity
- Fatigue
- Pain in the upper right side of the abdomen
- Swelling of the ankles, legs and abdomen
- Bluish tint or shading to your skin or lips
Symptoms of pulmonary hypertension usually limit a persons ability to exercise and do other activities.
Also Check: Does Onion Lower Blood Pressure
Lvrs And Lung Transplantation
Patients with advanced emphysema may benefit from LVRS . Generally, COPD with severe PH are not candidates for LVRS and should rather be considered for lung transplantation. LVRS could have favourable pulmonary haemodynamic effects, since it improves pulmonary function and arterial blood gases. Conversely, it could have deleterious effects, since it may cause a reduction of the pulmonary vascular tree.
There have been few studies on pulmonary haemodynamics before and after LVRS . LVRS may have adverse effects on pulmonary haemodynamics owing to the reduction of the vascular bed after the resection of lung tissue. Early studies have shown conflicting results, with increases in Ppa after LVRS in one study but not in others , . A recent study as part of the National Emphysema Treatment Trial has shown no significant differences in terms of Ppa and PVR, 6months after medical treatment or LVRS .
There Are Four Types Of Pah
According to Galié, “most types are considered idiopathic,” meaning there’s no known cause or major precipitating factor.
About 6% of cases are heritable. They’re passed down from a parent, most likely due to a mutation in a protein receptor that affects tissue growth. “If you’re carrying this gene it does not mean you’re definitely going to develop PAH, but you are at a higher risk,” Maresta says. “We think you need more than one trigger,” such as a pre-existing condition.
The idiopathic and heritable forms of PAH are at least twice as common in women compared to men. In fact, PAH is most often diagnosed in women between the ages of 30 and 60.
Share
In some cases, PAH can be drug-induced. The medication most famous for causing PAH is fen-phen , a weight loss drug that was popular in the 1960s and 1970s but is no longer on the market.
Lastly, associative cases occur when PAH goes hand in hand with another pre-existing condition, such as HIV, congenital heart disease or scleroderma.
All four typesidiopathic, heritable, drug-induced and associativeare treated similarly, but the prognosis might vary as a result of which one you have.
For example, notes Maresta, patients who have associative PAH because they also have scleroderma are already more prone to renal disease, GI complications and heart complications. “That can impact your overall life expectancy,” Maresta adds.
Also Check: Vodka Blood Pressure
What Causes Swelling Of The Feet And Ankles
Get immediate medical care if you experience the following symptoms along with swollen feet: 1. Edema Edema is a common condition where excess fluid is trapped in your bodys tissue. This causes swelling and puffiness of the tissue directly under your skin in your feet, ankles, and legs. It can also affect your hands and arms.
Therapies Targeting The No Pathway: Soluble Gc And Pdes
5.1.1 Soluble GC stimulation
5.1.2 PDE inhibition
Reinforcing the notion that sGC plays a prominent role in the pathology of COPD, another strategy for targeting the same downstream pathway supported this concept in preclinical studies. Namely, blockade of cGMP degradation by PDE5 inhibitors, such as sildenafil or tadalafil , prevented the development of PH in smoke-exposed guinea pigs and mice, respectively. In addition, guinea pigs treated with sildenafil had a lower airspace size than the placebo group. Also, lung structure and function in tadalafil-treated mice after smoke exposure did not differ from non-exposed animals. Surprisingly, treatment with the PDE4 inhibitor also had a significant protective effect on emphysema and PH development in mice, indicating that cAMP may play a role in COPD pathology as well . Regarding the transfer to the human disease, again, possible adverse effects on V/Q matching and oxygenation have to be taken into account . Interestingly, these effects appeared to be less pronounced in severe COPDPH .
Read Also: Onions And Blood Pressure
Nocturnal Oxygen Therapy In Patients With Isolated Sleep
COPD patients who are hypoxaemic while awake will also be hypoxaemic during sleep. In most COPD patients, hypoxaemia does, in fact, worsen during sleep and especially during REM sleep, as mentioned above. It follows that it is particularly important to oxygenate these patients during sleep. It is sometimes recommended to add 1L·min1 oxygen flow to the daytime resting prescription .
Some COPD patients do not have significant hypoxaemia when awake but are hypoxaemic during sleep with a mean nocturnal transcutaneous Sa,O2< 8890%. It has been hypothesised that sleep-related hypoxaemia, occurring in COPD patients without significant daytime hypoxaemia, could lead to permanent PH . If this was the case, prescription of nocturnal oxygen therapy to these patients would be justified. In fact, this hypothesis has not yet been demonstrated .
The present data, related to the evolution of pulmonary haemodynamics, are not sufficient for justifying the use of nocturnal oxygen in COPD patients who do not qualify for conventional oxygen therapy according to current criteria , .
The Relationship Between Copd And Heart Problems
Aug 13, 2021 | hide, Uncategorized
The number one cause of death in the United States is heart disease, and the second leading is cancer. However, what many people might not know is that the third leading cause of death is chronic lower respiratory diseases, such as chronic obstructive pulmonary disease . COPD and heart problems, specifically heart failure, have one serious symptom in commondifficulty breathing. Often, people with COPD and people with heart failure have difficulty exercising, walking distances and climbing stairs.
If you have COPD and heart problems, it can be difficult to pinpoint which disease is causing your shortness of breath. In some instances, it could be a combination. Heres what you need to know about the relationship between COPD and heart problems.
Also Check: Does Spicy Food Cause High Blood Pressure
Why Do The Pulmonary Arteries Narrow
Scientists believe that the process starts with injury to the layer of cells that line the small blood vessels of the lungs. This injury, which occurs for unknown reasons, may cause changes in the way these cells interact with the smooth muscle cells in the vessel wall. As a result, the smooth muscle contracts and grows more than is normal and narrows the vessel.
Peaks Of Ph During Sleep
Some COPD patients who are normoxaemic or mildly hypoxaemic during the day develop moderate to severe hypoxaemia during sleep , . These episodes of hypoxaemia are due to alveolar hypoventilation which occurs mainly in rapid eye movement sleep. They coincide with transient increase in Ppa, . It has been hypothesised that intermittent episodes of PH during sleep in COPD could lead to permanent PH . However, the investigations performed in this area are rather controversial. Indeed, one group found that desaturations during sleep is a risk factor for developing permanent PH and is associated with a worse prognosis , while another group found the opposite to be the case , .
Also Check: Does Spicy Food Cause High Blood Pressure
Pathobiology Of Pulmonary Hypertension In Copd
Remodeling of pulmonary vessels is the major cause of PH in COPD. It affects small and precapillary arteries and has been identified at different degrees of disease severity.8,9 The most prominent feature of pulmonary vascular remodeling in COPD is the enlargement of the intimal layer in muscular arteries. Intimal hyperplasia is produced by the proliferation of smooth muscle cells , which in advanced stages conform bundles of longitudinal muscle that differs from the normal circumferential disposition, and deposition of elastic and collagen fibers.8,9 In the arterioles, there is development of a medial coat of circular smooth muscle bounded by a new elastic lamina.
Intimal hyperplasia of pulmonary muscular arteries is apparent at all disease stages. In mild-to-moderate COPD the majority of SMC proliferating in hyperplasic intimas have a poorly differentiated phenotype, as shown by the lack of expression of contractile filaments that are characteristic of mature cells.8
Changes in the tunica media are less conspicuous and the majority of morphometric studies have failed to demonstrate differences in the thickness of the muscular layer when comparing COPD patients with control subjects.1012
Vascular stiffness is increased due to a higher deposition of elastic and collagen fibers. This results in an increase of PVR with the subsequent increase in PAP. Small reductions in the diameter of remodeled small pulmonary arteries can lead to significant increases in PVR.19
While Theres No Cure For Pah There Are Effective Ways To Manage The Disease
The median survival used to be 2.5 years. Now I’d say most patients are living seven to 10 years, and some are living as long as 20 years.
Alessandro Maresta. M.D., Vice President and Head of Global Medical Affairs, Actelion PharmaceuticalsShare
On a physiological level, there are several different biological mechanismsknown as pathwaysrelated to how blood vessels work that are believed to play a role in PAH.
“The guidelines strongly recommend that when a patient is diagnosed with PAH, they start a combination of drugs to target two different pathways,” Maresta says. “You might get one drug first, and then start on the second one within six months.” Maresta adds that current studies are now suggesting that targeting three pathways at once has the potential to lead to better outcomes.
While there’s currently no cure for PAH, the typical prognosis is much better today than it was 25 years ago. “The median survival used to be 2.5 years,” Maresta says. “Now I’d say most patients are living seven to 10 years, and some are living as long as 20 years.”
The main focus today, adds Maresta, is to find a new pathway and an effective drug to target itfor which research is currently underway. “We’re dedicated to making it happen,” Maresta says.
Don’t Miss: Onions Blood Pressure
Preventing High Blood Pressure When You Have Copd
One thing that’s important to know is that most causes of high blood pressure are very preventable. That’s good news, because that means that you can take control over the health of your heart and prevent high blood pressure by making healthy decisions.
However, it is not always easy to commit to the kinds of lifestyle changes that are necessary to keep your heart and blood vessels healthy. But the time, effort, and dedication it takes is worth the difference it will make to your health and your quality of life.
By and far, the best thing you can do to prevent high blood pressure when you have COPD is to quit smoking. Despite what some people believe, it’s never too late to quit smoking, and quitting will always have a positive effect on your health, even if you already have COPD.
In fact, if you still smoke, quitting smoking is one of the most important things you can do to treat your COPD. It will not only help you feel better both physically and mentally, but it could even slow down the progression of your COPD.
Eating a healthy, balanced diet and getting plenty of exercise is also extremely important for keeping your cardiovascular system healthy and strong. Eating lots of fruits and vegetables and living an active lifestyle is one of the most effective ways to prevent high blood pressure and atherosclerosis.
How to Prevent High Blood Pressure When You Have COPD:
Atherosclerosis Coronary Artery Disease And Left
No mater the cause of your high blood pressure, hypertension increases your risk for atherosclerosis. The pressure of your blood against the inside of your blood vessels causes tiny tears and inflammation, which provide perfect spots for plaque to stick to your artery walls.
Since most COPD patients already have a history of smoking, their blood vessels are already more prone to atherosclerosis. This makes high blood pressure even more likely to cause more severe cardiovascular problems for people with COPD.
Over time, atherosclerosis causes your arteries to narrow and harden, causing a more severe form of atheroscelrosis known as heart disease . As the blockages become even more severe, it causes the left side of your heart to enlarge.
Heart enlargement is one of the most dangerous effects of high blood pressure, and it causes your heart muscle to weaken over time. It happens when the pressure of the blood in your arteries gets so high that it creates a significant amount of back-pressure in your heart whenever it tries to pump.
This pressure causes blood to back up in your pumping chamber, which causes it to both pump faster and expand. While this allows the chamber to better handle the increased amount of blood, it also weakens the muscles in the walls of your heart, which eventually leads to heart failure.
Don’t Miss: Spicy Food High Blood Pressure
Group 1 Pulmonary Arterial Hypertension
Group 1 PAH can have a variety of causes including:
- connective tissue diseases
- schistosomiasis, a type of parasitic infection
- certain drugs or toxins, including some recreational drugs and diet medications
- conditions that affect the veins and small blood vessels of the lungs
PAH can also be inherited genetically. In some cases, PAH appears with no known cause.
Group : Pulmonary Hypertension Caused By Left Heart Disease
The left side of your heart is the high-pressure system that pumps blood to the rest of your body. If there are problems with how the left heart works, blood cant flow easily through your lungs into the left hand side of your heart.
As a result, the right side of your heart has to work harder to pump blood through your lungs. This increases the blood pressure in your pulmonary arteries.
This is one of the most common causes of pulmonary hypertension.
Recommended Reading: What Is The Va Disability Rating For Hypertensive Heart Disease
Development Of Copd With Pulmonary Hypertension
Pulmonary hypertension is often a result of COPD and is associated with increased risks of exacerbation and decreased survival, according to the study, Pulmonary hypertension in COPD, published in 2008. PH as a consequence of COPD can be mild-to-moderate but the combination of the two disorders can lead to a discouraging prognosis for patients. The symptoms worsen during exercise, sleep and exacerbation.
In patients with COPD, pulmonary artery pressure increases due to pulmonary vascular remodeling, which is caused by the combinations of hypoxia, inflammation, and loss of capillaries in severe emphysema. The same 2008 study revealed that a small proportion of COPD patients may present with out-of-proportion pulmonary hypertension, which is defined by a mean pulmonary artery pressure of about 35-40 mmHg, with normal levels lower than 20 mmHg, and a relatively preserved lung function. The prevalence of out-of-proportion pulmonary hypertension in COPD is similar to the prevalence of idiopathic pulmonary arterial hypertension.
How Are Peripheral Edema And Copd Linked
Peripheral edema is common in COPD patients. While COPD does not directly cause edema, it can result in a medical condition called pulmonary hypertension which causes peripheral edema. Oftentimes, when a COPD patient experiences swelling in the hands, legs, or feet, they dont associate it with their lung condition. Its often shrugged off as a sign of aging or they may take Benadryl or a similar drug thinking its an allergic reaction. Ideally, if you ever experience unusual symptoms its best to consult your doctor rather than trying home remedies because this may exacerbate the issue.
Also Check: Does Hot Sauce Cause High Blood Pressure
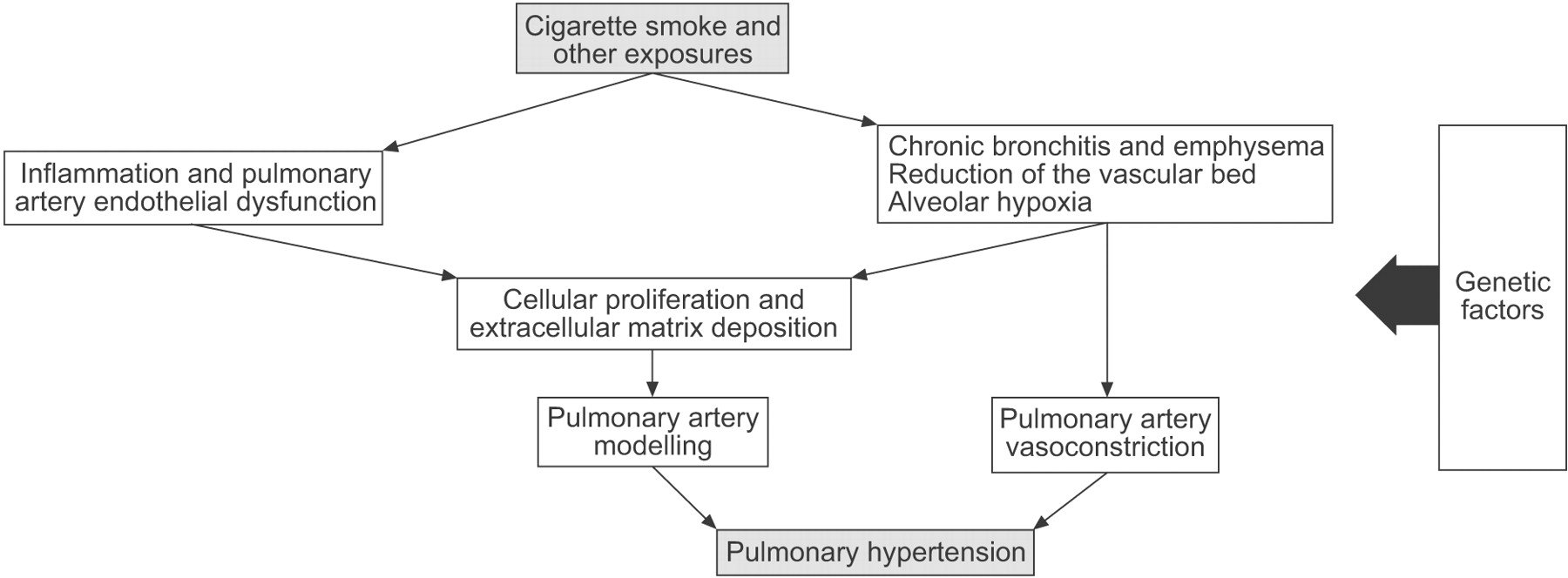
Tobacco Smoking Endothelial And Epithelial Dysfunction And Inflammation
In addition to hypoxia-driven mechanisms described above, recent studies provided evidence that tobacco smoking may cause remodelling of the pulmonary arteries, independent of changes in lung function . Animals with chronic cigarette smoke exposure developed pulmonary vascular remodelling prior to lung emphysema development . Cigarette smoke acts through either a direct effect on endothelial cells, epithelial cells, , and/or pulmonary arterial smooth muscle cells or through an inflammatory mechanism . Endothelial dysfunction causes vascular stiffness, for example, due to lack of NO and prostacyclin and overproduction of thromboxane A2 and endothelin-1 , and is frequently present in COPD . Some studies suggest that endothelial dysfunction of the small pulmonary vessels also causes lung emphysema . In addition, endothelial dysfunction also results in left HF, which again contributes to an increase in mPAP. Cigarette smoke is also associated with epithelial cell apoptosis causing lung emphysema. Inflammatory cytokines like C-reactive protein, TNF-, the chemokine CCL2, soluble intercellular adhesion molecule-1, and PDGF can contribute to pulmonary vascular disease by directly affecting the pulmonary artery smooth muscle cells and pulmonary artery endothelial cells . In addition, tobacco smoke may directly target pulmonary artery smooth muscle cells .