Metformin In Pulmonary Hypertension In Left Heart Disease
- 1Heart and Vascular Institute, University of Pittsburgh Medical Center, Pittsburgh, PA, United States
- 2Division of Cardiology, Department of Medicine, School of Medicine, University of Pittsburgh, Pittsburgh, PA, United States
- 3Department of Bioengineering, University of Pittsburgh, Pittsburgh, PA, United States
- 4Pittsburgh Heart, Lung, Blood and Vascular Medicine Institute, University of Pittsburgh, Pittsburgh, PA, United States
- 5McGowan Institute for Regenerative Medicine, University of Pittsburgh, Pittsburgh, PA, United States
- 6Clinical and Translational Science Institute, University of Pittsburgh, Pittsburgh, PA, United States
Group 1 Pulmonary Arterial Hypertension
Group 1 PAH can have a variety of causes including:
- connective tissue diseases
- schistosomiasis, a type of parasitic infection
- certain drugs or toxins, including some recreational drugs and diet medications
- conditions that affect the veins and small blood vessels of the lungs
PAH can also be inherited genetically. In some cases, PAH appears with no known cause.
Pulmonary Hypertension: Prognosis And Life Expectancy
Pulmonary hypertension is caused by high blood pressure in the arteries that are responsible for carrying blood from the right side of the heart to the lungs.
The life expectancy of an individual with PH depends on several factors, including the class of PH, the type of PH, and any underlying conditions. Prognosis with the disease has improved greatly over the years thanks to better medications and treatments.
For example, the life expectancy of someone with pulmonary arterial hypertension , one type of PH, used to be 2.5 years. Now it has been extended to more than a decade.
Recommended Reading: Vinegar For Blood Pressure
Factors That Can Affect Pulmonary Hypertension
While pulmonary hypertension has no cure, you can live an active, fulfilling life by working with your doctor to manage your symptoms. Talk to your doctor before taking over-the-counter medicine, as some can worsen symptoms of pulmonary hypertension or interfere with prescriptions and keep a list of medicines with you. Ask whether you should get a pneumonia vaccination or flu shot. Additionally, pregnancy can pose serious risks for women with pulmonary hypertension, so be sure to discuss birth control options with your physician.
Group : Ph Due To Left
Group 2 refers to PH due to left heart disease, also known as pulmonary venous hypertension. Long-term problems with the left side of the heart can lead to changes in the pulmonary arteries and cause PH. This may include:
- Left ventricular systolic dysfunction, in which the heart cannot pump blood effectively
- Left ventricular diastolic dysfunction, when the heart cannot properly relax to allow enough blood to flow into it
- Valvular disease, when the valves of the left side of the heart do not work properly, reducing blood flow or allowing blood to flow backwards
You May Like: How Does Alcohol Increase Blood Pressure Mechanism
A Special Focus: Patients With Heart Failure
Pulmonary venous hypertension occurs in an estimated 19-35% of patients with left heart disease . Treatment of PVH is aimed at the underlying disease process. Hypervolemia in both diastolic and systolic heart failure is treated with diuretics, salt and fluid restriction. Optimization of therapy is patients with systolic heart failure include administration of an ACE-I or ARB, beta blocker, aldosterone antagonist and in some patients the combination of a nitrate and hydralazine. Blood pressure control in patients with diastolic heart failure is essential. However, elevated pulmonary artery pressure may persist after augmenting diuresis and optimizing medical therapy. An additional reactive phenomenon with superimposed pulmonary arterial disease may exist in a subset of patients with left-sided heart failure. Generally, this reactive vasculopathy is diagnosed when the mean PA pressure is > than 25 mm Hg, PVR> 3 woods units, and the transpulmonary gradient is > 20 mmHg . It is postulated that this out of proportion PH is triggered by chronically elevated pulmonary venous pressures leading to pre-capillary vasoconstriction and remodeling. However, it remains unclear what degree and duration of PVH is required to trigger this phenomenon. Also consider evaluation for COPD, sleep disordered breathing and thromboembolic disease in appropriate patients.
Ph In Valvular Heart Disease
Aortic Valve:
PH is present in 28% to 56% of patients with severe aortic stenosis, depending on patient selection criteria and definition of PH used. The prognosis of patients with severe aortic stenosis and PH is dismal., Surgical aortic valve replacement is the recommended treatment of patients with severe aortic stenosis in the appropriate clinical setting. Perioperative complications associated with aortic valve replacement are greater when PH is present preoperatively. Valve replacement is an effective treatment of the PH associated with this condition, however, and a significant decrease in PAP can be seen immediately after surgery. Some patients will have persistent PH, and these patients have decreased long-term survival. Transcatheter aortic valve replacement is an emerging therapeutic option, particularly in patients with severe aortic stenosis and PH who are at high risk for surgical valve replacement.
PH can also develop in patients with aortic regurgitation. Surgical repair of aortic regurgitation is recommended when symptoms develop or when LV dilation occurs. There does not appear to be an increased risk of mortality or operative complications in patients with aortic regurgitation with severe PH compared with those with mild or no PH, and in most cases, the PAP normalizes with aortic valve replacement. Again, there is no current literature to support the use of PAH-specific therapies in patients with aortic regurgitation.
Mitral Valve:
Recommended Reading: Calibrate Omron
These Lifestyle Changes Can Improve Your Symptoms:
- Quit smoking. Your doctor can recommend programs and products to help.
- Follow a healthy diet. Eat a variety of fruits, vegetables, and whole grains, plus lean meat, poultry, fish and low-fat/fat-free milk. Your diet should be low in fat, cholesterol, sodium and sugar.
- Watch your weight. A daily record of your weight can help you be aware of rapid weight gain, which may be a sign that your pulmonary hypertension is worsening.
- Stay active. Incorporate physical activity such as walking into your lifestyle. Discuss the level of activity with your doctor. Avoid straining or lifting heavy weights. Rest when you need to.
- Avoid sitting in a hot tub or sauna, or taking long baths, which will lower your blood pressure.
- Be cautious about air travel or high-altitude locales. You may need to travel with extra oxygen.
- Get support for the anxiety and stress of living with pulmonary hypertension. Talk with your healthcare team, or ask for a referral to a counselor. A support group for people living with pulmonary hypertension can be invaluable in learning how to cope with the illness.
Written by American Heart Association editorial staff and reviewed by science and medicine advisers. See our editorial policies and staff.
Last Reviewed: Oct 31, 2016
Alterations In Platelet Bioenergetics And Mitochondria Dysregulation
Finally, intracellular lipid chaperones, fatty acid binding proteins , coordinate lipid responses in cells and are strongly linked to metabolic and inflammatory pathways . A particular type of FABP, a cardiac-specific cytoplasmic protein, has been reported as a marker for ongoing myocardial damage, with a potential prognostic value of adverse cardiac events. This protein, absent in Group-1 PAH, has been recently proposed as major indicator of PH-LHD . This observation is probably due to the specificity of this molecule for left-heart damage, but also supports distinctive metabolic dysfunctions in PH-LHD.
Read Also: Can Apple Watch Tell Your Blood Pressure
Changes In The Heart And Lungs
Regardless of the type, the changes in the heart and lungs from pulmonary hypertension are generally the same. The pulmonary arteries, which carry blood from the heart to the lungs, narrow. This makes it difficult for blood to pass through, causing a rise in pressure and straining the right side of the heart.The right ventricle receives unoxygenated blood from the body and pumps it into the lungs, and it has to work very hard to overcome this increased pressure. Eventually, the right ventricle weakens and can no longer pump enough blood to the lungs, resulting in right-sided heart failure.
Screening And Diagnostic Evaluation
There are no data to support screening of asymptomatic individuals for pulmonary hypertension, even in high-risk groups such as those with a family history of pulmonary arterial hypertension without known BMPR2 mutations.3,22 For patients with systemic sclerosis and related diseases, expert opinion suggests annual screening with laboratory testing , electrocardiography, and pulmonary function testing, followed by echocardiography.3,8 Expert consensus recommends annual echocardiography in patients with sickle cell disease and those with known BMPR2 mutations.3,14
Recognizing pulmonary hypertension in patients presenting with new signs or symptoms can be difficult because many symptoms are common and associated with an extensive differential diagnosis . Pulmonary hypertension should be considered in patients with chronic illness and symptoms that are disproportionate to the underlying disease or poorly responsive to treatment.
Findings Suggestive of Pulmonary Hypertension
History
Information from references 1 through 3, and 22.
Findings Suggestive of Pulmonary Hypertension
History
Information from references 1 through 3, and 22.
Evaluation of Suspected Pulmonary Hypertension in Primary Care
Figure 1.
Suggested algorithm for the evaluation of suspected pulmonary hypertension in primary care.
Evaluation of Suspected Pulmonary Hypertension in Primary Care
Figure 1.
Suggested algorithm for the evaluation of suspected pulmonary hypertension in primary care.
Don’t Miss: To Lower Blood Pressure
Prevalence And Significance Of Pulmonary Hypertension In Left Ventricular Heart Failure
The presence and extent of PH and RV dysfunctionwhich are both common in LV HFare associated with disease progression, decreased exercise tolerance, and an unfavourable outcome. Data on the prevalence of PH in patients with HF yield variable numbers and depend on the method of PAP measurement, the definition of PH, and the populations studied. Although both HF with reduced ejection fraction and HF with preserved ejection fraction belong to the clinical syndrome of heart failure, they constitute distinct entities with regard to pathophysiology, clinical characteristics, haemodynamics, cardiopulmonary interaction, and response to therapy, and should thus be viewed separately. In HFrEF, the prevalence of PH as assessed by RHC was reported to be between 40 and 75%.,, In patients with HFpEF, recent studies utilizing either echocardiography or RHC indicated a PH prevalence in a range between 36 and 83%.
Ph And Restrictive Cardiomyopathy

Restrictive cardiomyopathies should always be considered in the differential diagnosis of patients presenting with elevated left-sided pressures and normal LV systolic function. Although certain echocardiographic findings, including Doppler tissue velocities, may suggest the diagnosis, further testing, including invasive hemodynamics, endomyocardial biopsy, and additional imaging, may be necessary to establish the diagnosis and to differentiate this condition from constrictive pericarditis. Restrictive cardiomyopathy is frequently difficult to treat and may result in severe PH, although this phenomenon has not been well studied. Further evaluation and management of these patients is beyond the scope of this review.
Don’t Miss: What Causes Blood Pressure To Drop
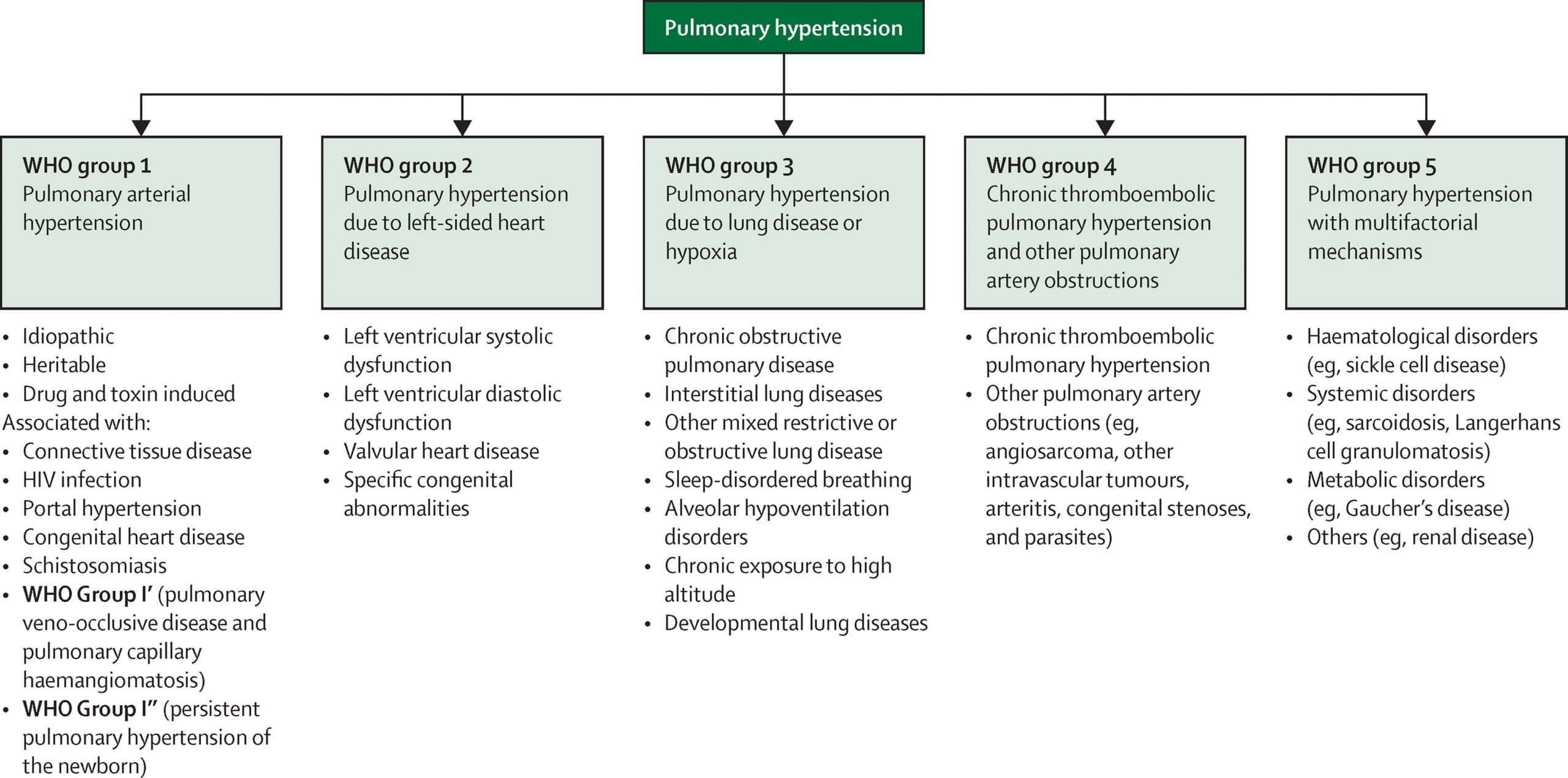
Who Classification Of Pulmonary Hypertension
Pulmonary hypertensionelevated blood pressure within the pulmonary arteryis a serious condition that has many causes. For healthcare providers, understanding the cause of a persons pulmonary hypertension is a critical first step in deciding on optimal therapy.
Category 1 Ph: Cardiac Arrest In Eisenmenger’s Syndrome
In contrast to , whose subject was WHO functional class II despite severe PAH, shows the autopsy findings of a female in her third decade. This patient also had a secundum ASD and Eisenmenger’s physiology but suffered out-of-hospital cardiac arrest. An ECG obtained shortly before her death shows severe right axis deviation and RVH . This is consistent with the dilated right ventricle with focal thinning noted at autopsy . Figure and shows the anatomy of the ostium secundum ASD.
Congenital heart disease patient with out-of-hospital sudden cardiac death. ECG showing severe RVH. Severe RV hypertrophy and dilatation. Ostium secundum atrial septal defect.
You May Like: Do Allergy Pills Raise Blood Pressure
Right Ventricular Pathological Changes
RV Metabolic Derangements
Work aimed at understanding the switch between adaptive and maladaptive RV remodeling have identified metabolic derangements as a likely mediator. In particular, mitochondrial dysfunction marked by reduced oxidative metabolism and ectopic glutaminolysis has been shown to play a role in RV dysfunction in PAH.
RV Ischemia
Another factor contributes to maladaptive RV remodeling and metabolic changes is RV ischemia due to reduced right coronary artery epicardial flow and capillary rarefaction associated with PAH.
-
In the normal RV, perfusion from the right coronary artery occurs during systole and diastole. However, in PAH, elevated RV systolic pressure minimizes the pressure differences between the right coronary artery and the aorta and thus reduces filling time and RV perfusion .
-
Impaired angiogenesis demonstrated by reduced number of capillaries and intramuscular arterioles can also contribute to RV ischemia , a phenotype often observed in Scleroderma-associated PAH. Scleroderma patients typically display maladaptive RV remodeling , providing more evidence that relative RV ischemia contributes to RV failure in PAH.
RV Calcium Mishandling
While the cellular mechanisms of LV dysfunction has been extensively studied, the understanding of the causes of RV dysfunction in PAH has lagged behind. However, recent data has emerged that suggests calcium mishandling contributes to RV dysfunction in PAH.
Sarcomere Remodeling
Cytoskeletal Remodeling
Availability Of Data And Materials
The study database was anonymized, and the study complied with the requirements of the Japanese Ministry of Health, Labour and Welfare. The datasets analyzed during the current study are not publicly available, but are available from the corresponding author on a reasonable request and with the permission of our department.
Recommended Reading: Why High Blood Pressure Happens
Overview Of Who Group 2 Pulmonary Hypertension Due To Left Heart Disease
Christopher F. Barnett, Van N. Selby Overview of WHO Group 2 Pulmonary Hypertension Due to Left Heart Disease. Advances in Pulmonary Hypertension 1 January 2015 14 : 7078. doi:
Background: Left heart disease is the most common cause of pulmonary hypertension and is associated with poor patient outcomes, especially among patients undergoing heart transplant evaluation.
Implications for clinicians: Left heart disease should be considered in all patients undergoing an evaluation for PH. Correct management of PH from LHD is to optimize treatment of LHD. Pulmonary vasodilators used to treat pulmonary arterial hypertension should not be used in patients with PH from LHD.
Additional research is needed to better understand how PH develops in patients with LHD and to investigate the role for treatment targeting PH in these patients.
Causes of pulmonary hypertension due to left heart disease .
Causes of pulmonary hypertension due to left heart disease .
Candelas Prez Del Villar
1Department of Cardiology, Hospital General Universitario Gregorio Marañón, 28007 Madrid, Spain
2Instituto de Investigación Sanitaria Gregorio Marañón, 28007 Madrid, Spain
3Centro de Investigación Biomédica en Red, CIBERCV, Instituto de Salud Carlos III, 28026 Madrid, Spain
4Facultad de Medicine, Universidad Complutense de Madrid, 28007 Madrid, Spain
Recommended Reading: How To Calibrate Home Blood Pressure Monitor
Group : Pulmonary Hypertension From Unclear Multifactorial Mechanisms
Group 5 combines all other causes that are not defined in the previous groups. For example, all causes like hematological and metabolic disorders, various blood diseases, and system disorders will fall under this group.
Treatment options: The treatment will solely depend on the underlying reason. Thus, if a patient has a metabolic disorder that has lead to pulmonary hypertension, his treatment will be mainly aimed at the metabolic disorder as well as relieving pulmonary hypertension by additional medications.
Metformin And Cardiovascular Disease

Several large observational cohort studies have outlined the merits of metformin in CVD in diabetics, including improved outcomes in coronary artery disease , myocardial infarction , and heart failure . Furthermore, data suggests that metformin may avert the progression and/or development of HF . The most current data corroborating this is from supplemental analysis of the EMPA-REG OUTCOME trial, in which patients were randomly assigned to receive empagliflozin 10 mg or 25 mg or placebo daily. Outcomes from this trial include CV death, non-fatal MI or stroke, and hospitalizations. Metformin use, even in the placebo arm of the trial, was associated with improved cardiovascular outcomes including CV death, HF hospitalizations, major adverse cardiac events, and all-cause mortality . The benefit of metformin in CVD is so profound that the American College of Cardiology has delineated its benefits in its 2018 ACC consensus, New Diabetic Drugs to Reduce CV Outcomes . Despite this growing evidence, data on metformin’s potential therapeutic role in specific CVD processes is limited.
Also Check: Does Spicy Food Increase Blood Pressure
Functional Classes Of Pulmonary Hypertension
Currently, there is no one cure for PH. This disease is caused by many factors and can worsen over time at different rates for different people. Left untreated, PH can cause permanent damage to the heart and lungs and can become life-threatening.
The World Health Organization divides cases of PH into four functional classes depending on how much the disease limits activities. The classes are as follows:
- Class 1 PH Diagnosed when there are no PH symptoms at either rest or with exercise
- Class 2 PH Diagnosed when there are no PH symptoms at rest, but there is shortness of breath during everyday activities such as shopping for groceries or climbing stairs
- Class 3 PH Diagnosed when there may not be PH symptoms at rest, but household chores and everyday activities are greatly limited due to fatigue or shortness of breath
- Class 4 PH Diagnosed when there are PH symptoms both at rest and during everyday activities swelling of the ankles and feet known as edema is common, and fainting is also possible
Metformin In Pah And Hfpef
Briefly, although beyond the scope of this review, the therapeutic role of metformin is also being investigated in both pulmonary arterial hypertension and HFpEF. There is a growing body of evidence that PAH is associated with a number of systemic metabolic derangements including metabolic syndrome, insulin resistance, and glucose intolerance. Alterations in aerobic glycolysis, tricarboxyclic acid metabolism, and fatty oxidation have all been implicated in the pathophysiology. Given these findings, there is at least one currently ongoing clinical trial looking at the role of metformin in PAH . While in HFpEF there is significant clinical heterogeneity, there is increasing evidence illustrating metformin’s therapeutic benefit across the varying phenotypes. Halabi et al. recently published a systematic review and meta regression analysis analyzing the role of metformin in HFpEF. Metformin reduced mortality and morbidity in HFpEF patients even after adjustment for other HF and glycemic control therapies including beta blockers, angiotensin converting enzyme inhibitors, and insulin .
You May Like: Reverse Pulmonary Hypertension