Symptoms Of Heart Failure And Decreased Cardiac Output
Symptoms of heart failure and decreased heart output include tiredness, tiring easily and shortness of breath that might impact your sleep and other aspects of your lifestyle. Tachycardia, or a quick heart rate even when at rest is an arrhythmia that typically occurs as a result of heart failure.
You might feel lightheaded, weak and lightheaded. You might likewise discover swelling of your extremities, especially of your ankles and feet. Swelling of the abdominal area is also a symptom of the reduced cardiac output associated with heart failure.
Structural Changes In Hypertension
Both heart and arteries adapt their structure in response to altered load. This occurs physiologically and pathologically in hypertension. Increased pressure exerts an increased load on a thin walled chamber or tube by increasing wall tension according to Laplaces law .
Wall stress and tension in a thin walled tube or chamber .
More complex expressions for wall tension in the heart or blood vessels exist, but this is a reasonable approximation. A rise in tension results in increased wall tensile stress. Normalisation of wall tensile stress can be achieved either by an increase in wall thickness or by a reduction in chamber/lumen diameter, or both.
Haemodynamics Of Early Hypertension Or Pre
While the basic haemodynamics of established hypertension are undisputed, there is less agreement about the haemodynamic pattern in young individuals with elevated blood pressures. Since an individuals position within the overall blood pressure distribution tends to remain fairly constant these subjects are at high risk of developing hypertension in later life.
In young individuals less than 19 years, most evidence suggests that subjects with the highest blood pressure have increased PVR, though small increases in cardiac index have been seen in some studies.w12 w13 There is evidence that young individuals with hypertension have an increased sympathetic activity, though studies in established hypertension are inconclusive. The question is complicated by methodological difficulties in the assessment of sympathetic nerve activity in vivo and the importance of increased sympathetic activity in the development of hypertension is uncertain. Interestingly, an increased left ventricular mass is a fairly consistent finding in young individuals with raised blood pressure and is also seen in offspring of hypertensives,w14 although the functional determinants of this abnormality are not well understood.
Don’t Miss: Does Claritin D Cause High Blood Pressure
Height Weight Bmi And Bsa As Independent Variables And Scaling Of Factors
These results further emphasize the importance of evaluating many physiological phenomena within the context of body size. West and Brown, for example, report such scaling over many orders of magnitude across living forms for metabolic power, proxies for which are cardiac output or blood volume flow rate through the cardiovascular system . Others emphasize the critical importance of body size measurements in cardiovascular medicine. Our studies emphasize that the findings regarding the role of obesity in the etiology of hypertension must be carefully considered within the context of specific assessments of body orientation, size and mass.
The effect of aging on the relationship between body size and cardiovascular variables is not known. However, the fact that these relationships are firmly established in pediatric literature, and the present and related studies extend pediatric results to young adults, but these relationships are not commonly recognized in older adults, hints that the effect may diminish with age.
Definition Of Hypotension And Its Causes
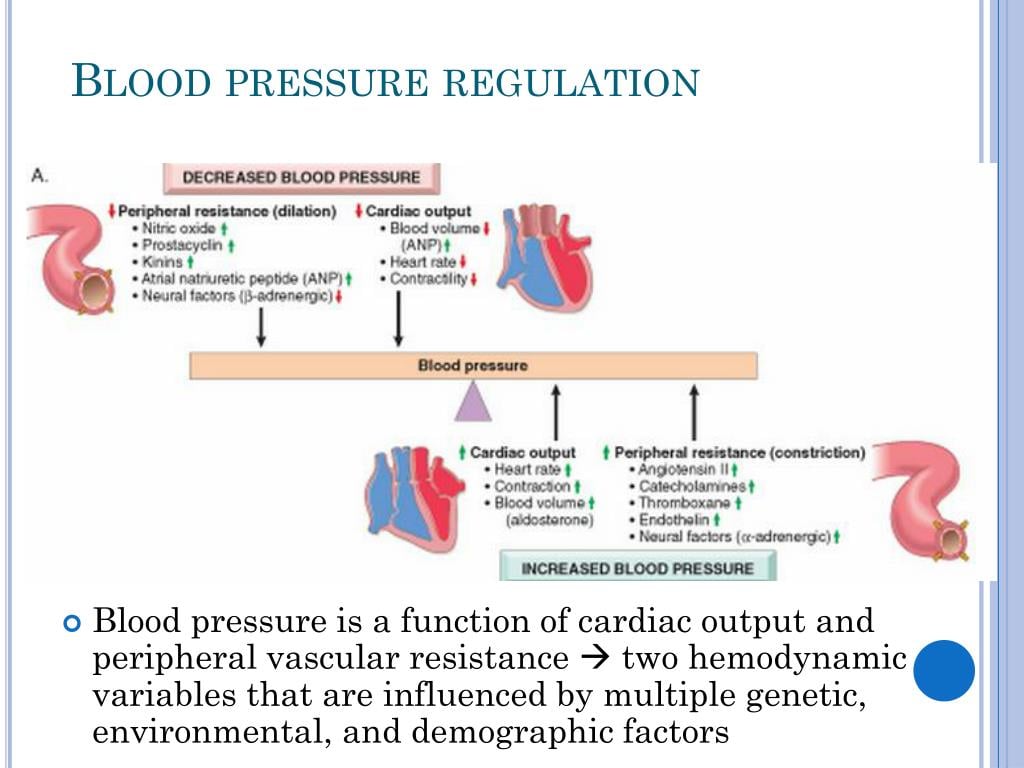
Hypotension is a physiologic state in which the arterial blood pressure is abnormally low. For an adult, hypotension exists when the is less than 90 mmHg and the is less than 60 mmHg. Hypotension reduces blood flow and therefore oxygen delivery to organs and tissues, which may cause cellular damage and dysfunction. When oxygen delivery is insufficient to support tissue metabolic requirements, a person is said to be in circulatory shock. Because arterial pressure is determined by cardiac output, venous pressure and systemic vascular resistance , a reduction in any of these variables can lead to hypotension. Hypotension may result from:
The following diagram shows diseases or conditions that may result in reduced cardiac output, or those related to abnormal vascular function.
Recommended Reading: Can I Take Claritin With High Blood Pressure
Does Systemic Vascular Resistance Affect Heart Rate
When blood vessels dilate, the blood flow is increased due to a decrease in vascular resistance. Therefore, dilation of arteries and arterioles leads to an immediate decrease in arterial blood pressure and heart rate. Cardiac output is the amount of blood ejected by the left ventricle in one minute.
Flotrac Sensor And Vigileo Monitor: Basic System Configuration
The system consists of a specialized blood pressure sensor and monitor to collect and analyze arterial pressure data in real time. The output variables from this analysis, as displayed on the monitor in this most basic configuration, include CO, cardiac index, SV, and SV index .
To perform accurate analysis, a high-quality arterial pressure waveform is mandatory. Thus, the catheter conducting system must be free of air bubbles, which would otherwise dampen the signal, and also be of an appropriate length and stiffness of connecting tubing to minimize harmonic artifacts. When starting the monitor, the healthcare professional enters the patient’s age, gender, height, and weight, which are important to establish a baseline estimate of the patient’s large-vessel compliance and to calculate indices of displayed parameters. Once the procedure for zeroing the arterial pressure in the monitor is complete, the algorithm continuously collects and analyzes the pressure signal received from the sensor to calculate SV.
This and other monitoring technologies are commonly validated against a clinical gold standard, pulmonary artery cathers in this case, using Bland-Altman analysis. Variance of measurements against the gold standard is commonly compared as part of assessing clinical applicability and utility of the device. The first validation studies of this kind were conducted showing clinically acceptable performance.,,
Also Check: How To Calibrate Omron Blood Pressure Machine
How Does Cardiac Output Affect Mean Arterial Pressure
Mean arterial pressure iscardiac outputCardiac output isis
. In this way, what will increase mean arterial pressure?
This number in parentheses is the mean arterial pressure . For example, it’s harder for blood to flow through a narrow artery. As resistance in your arteries increases, blood pressure also increases while the flow of blood decreases.
Likewise, what happens when mean arterial pressure drops? When the MAP gets below 60, vital organs in the body do not get the nourishment they need for survival. When it gets low, it can lead to shock and eventually death of cells and organ systems. Low mean arterial pressure can be caused by sepsis, stroke, hemorrhaging, or trauma.
In this manner, how does cardiac output maintain blood pressure?
Cardiac output is calculated by multiplying heart rate by stroke volume. For a given TPR, the blood pressure is maintained unless there is a relative bradycardia or a further fall in stroke volume. During systole, the volume of blood ejected from the left ventricle must enter the aorta and major arterial branches.
Does increasing blood pressure increase cardiac output?
Blood pressure increases with increased cardiac output, peripheral vascular resistance, volume of blood, viscosity of blood and rigidity of vessel walls. Blood pressure decreases with , peripheral vascular resistance, volume of blood, viscosity of blood and elasticity of vessel walls.
Normative Levels Of Arterial Pressure In Humans
ABP is a quantitative trait because values vary with age, sex, body weight, and physical activity of the individual. A pressure considered normal in one individual may be judged abnormal in another. ABP increases with age for both genders and generally is lower in premenopausal women than in men of the same age. ABP increases with increased body mass such that some hypertensive subjects can normalize their ABP by losing only 510% of body mass. Once hypertension is evident, gender differences tend to be obscured .
Figure 11. Variation of systolic blood pressure and diastolic blood pressure with age as function of gender and race for subjects in the U.S. population, over the age of 18 years. For both genders, SBP exhibits a steady increase with age. As discussed, this SBP age-dependence partly reflects increased rigidity of conduit and smaller arteries with aging. In contrast, DBP tends to exhibit little increase beyond the age of 5059 years for both genders. Note the significant increase in pulse pressure after the age of 50 years for both genders and races examined.
Figure 12. Illustration of the extreme spread of systolic blood pressure . In part, the distribution spread reflects age variation, as shown in Figure 11. As reported in the JNC7, SBPs greater than 115 mmHg are associated with 60% increase of cerebrovascular disease in subjects and nearly 50% ischemic heart disease.
Daniel De Backer, in, 2020
You May Like: What Is A Dangerously High Blood Pressure
Changing The Diameter Of Arterioles And Veins
Muscle tissue within the walls of arterioles allow these blood vessels to widen or narrow . The more constricted arterioles are, the greater their resistance to blood flow and the higher the blood pressure. Constriction of arterioles increases blood pressure because more pressure is needed to force blood through the narrower space. Conversely, dilation of arterioles reduces resistance to blood flow, thus reducing blood pressure. The degree to which arterioles are constricted or dilated is affected by
-
Nerves that contract smooth muscle in the arterioles, thus reducing their diameter
-
Hormones that are primarily made by the kidneys
-
Certain drugs
Veins also play a role in the control of blood pressure, although their effect on blood pressure is much less than that of arterioles. Veins dilate and constrict to change how much blood they can hold . When veins constrict, their capacity to hold blood is reduced, allowing more blood to return to the heart from which it is pumped into the arteries. As a result, blood pressure increases. Conversely, when veins dilate, their capacity to hold blood is increased, allowing less blood to return to the heart. As a result, blood pressure decreases.
What’s The Desired Outcome For People With Decreased Cardiac Output
Depending on the patient and the underlying causes of decreased cardiac output, there are different desired outcomes for controlling and managing the condition. For some people, their cardiac output can be returned to a normal, healthy level, while for others the issue is chronic and they will need to make lifestyle changes in order to manage their decreased cardiac output.
Evidence of improved cardiac output includes:
- Blood pressure within a normal range for the patient
- Pulse steady and within 60-100 beats per minute
- Breathing is unlabored
- Urine output at least 30 ml/hour
- Patient feels less weak and fatigued
- No dizziness or confusion
- Skin is warm and usual color
Not all patients may be able to meet these desired outcomes though. In order to reach the desired outcome, different nursing care plans for decreased cardiac output may be implemented, and these are explained in the next section.
Recommended Reading: What Is A Dangerously High Blood Pressure
Deleterious Effects Of Inotropic Therapy
As the long-distance cyclist will know, prolonged strenuous exercise can lead to high tissue oxygen demands, which can later result in impaired muscle contraction and poor performance. Positive inotropic drugs act by different mechanisms to increase the contractility of the heart, and as such have been proposed for use in patients with cardiac failure to increase myocardial contractility and hence cardiac output. Indeed, in the short-term, acute phase of heart failure, inotropic drugs can be useful to increase cardiac output. When considered in light of our analogy, however, it is easy to appreciate that excessive inotropic stimulation may increase the myocardial oxygen demand, leading ultimately to myo-cardial ischemia. Indeed, prolonged stimulation with long-term inotropic therapy has been shown to increase mortality rates in patients with chronic heart failure . In contrast, reducing the force of contraction may enable the cyclist to pedal longer this may account for some of the beneficial effects of prolonged -blockade therapy in the treatment of heart failure.
Determinants Of Arterial Pressure
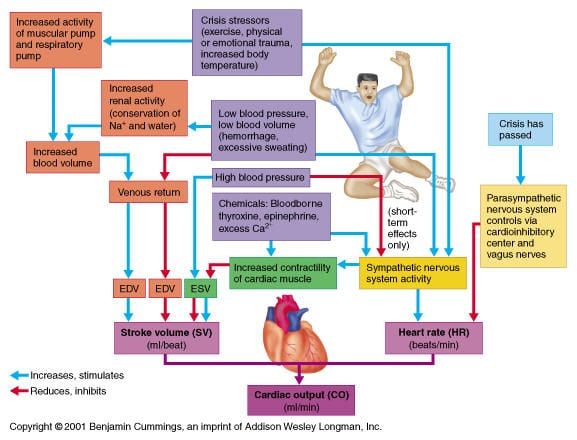
The main determinant of arterial pressure is the stretch of the walls of the arteries by the volume they contain. This volume increases in systole because inflow exceeds outflow and falls after the peak of ejection because outflow exceeds inflow. The outflow is dependent upon the resistance emptying the arterial tree and the elastance of the vessel walls. The product of the inverse of elastance and the downstream resistance gives the time constant of emptying of the arterial vessels. The time constant is the time it takes to get to 63% of a new steady state after a step change in flow or pressure. Time constants are important in pulsatile systems because they set the amount of filling and emptying of aortic volume that can occur based on the cardiac frequency, the proportions of contraction and relaxation times during systole, and the diastole time.
Read Also: Does Claritin D Raise Blood Pressure
What Are Signs Of Decreased Cardiac Output
The signs and symptoms of decreased cardiac output include the abnormal presence of S3 and S4 heart sounds, hypotension, bradycardia, tachycardia, weak and diminished peripheral pulses, hypoxia, cardiac dysrhythmias, palpitations, decreased central venous pressure, decreased pulmonary artery pressure, dyspnea, fatigue.
Elasticity Of Vessel Walls
Elasticity of vessel walls refers to the capacity to resume its normal shape after stretching and compressing. Vessels larger than 10 mm in diameter are typically elastic. Their abundant elastic fibres allow them to expand as blood pumped from the ventricles passes through them, and then to recoil after the surge has passed. If artery walls were rigid and unable to expand and recoil, their resistance to blood flow would greatly increase and blood pressure would rise to even higher levels, which would in turn require the heart to pump harder to increase the volume of blood expelled by each pump and maintain adequate pressure and flow. Artery walls would have to become even thicker in response to this increased pressure.
_________________________________________________________________________
All content on this page was adapted from OER #2:
© Apr 10, 2017 OpenStax Anatomy and Physiology. Textbook content produced by OpenStax Anatomy and Physiology is licensed under a Creative Commons Attribution License 4.0 license. Download for free at
Recommended Reading: Does Claritin D Raise Blood Pressure
Determinants Of Levels Of Arterial Pressure
The pressure difference between systolic and diastolic pressure is termed the pulse pressure. Pulse pressure, which is sensed by the blood vessel elements, has recently been deemed a potential contributor to the development of both systemic arterial hypertension and arterial wall damage contributory to atherosclerosis.
Arterial pressure is influenced by many factors. These include age, gender, body weight, level of physical conditioning, current physical activity, and behaviors of all kinds, for example, stress, eating, drinking, and exercise. Arterial pressure can also be influenced by many agents, both prescription and over-the-counter drugs, herbal products, caffeine-loaded energy drinks, psychoactive drugs, and drugs of abuse. Further, arterial pressure varies continuously with variations caused by changes in heart beat-to-beat intervals, periods of rest and sleep, as well as levels of psychological stress.
M.P. Printz, in, 2014
Monitoring And Controlling Blood Pressure
Baroreceptors are specialized cells located within arteries that act as blood pressure sensors. Those in the large arteries of the neck and chest are particularly important. When baroreceptors detect a change in blood pressure, they trigger the body to react to maintain a steady blood pressure. Nerves carry signals from these sensors and the brain to
-
The heart, which is signaled to change the rate and force of heartbeats . This change is one of the first, and it corrects low blood pressure quickly.
-
The arterioles, which are signaled to constrict or dilate .
-
The veins, which are signaled to constrict or dilate .
-
The kidneys, which are signaled to change the amount of fluid excreted and to change the amount of hormones that they produce . This change takes a long time to produce results and thus is the slowest mechanism for how the body controls blood pressure.
Nonetheless, the ways that the body can monitor and control blood pressure have limitations. For example, if a person loses a lot of blood quickly, the body cannot compensate quickly enough, blood pressure falls, and organs may begin to malfunction .
In addition, as people age, the body responds to changes in blood pressure more slowly.
You May Like: Can High Bp Cause Chest Pain
Changing The Body’s Position
Blood pressure can vary throughout the body due to the direct action of gravity. When a person is standing, blood pressure is higher in the legs than in the head, much in the way that the water pressure at the bottom of a swimming pool is higher than that at the top. When a person lies down, blood pressure tends to be more equal throughout the body.
When a person stands up, blood from the veins in the legs has a harder time getting back to the heart. As a result, the heart has less blood to pump out, and blood pressure may temporarily drop throughout the body. When a person sits down or lies down, blood can more easily return to the heart, and cardiac output and blood pressure may increase. Elevating the legs above the level of the heart can increase return of blood to the heart, which increases cardiac output and raises blood pressure.
How Blood Volume Affects Blood Pressure
Changes in blood volume affect arterial pressure by changing cardiac output. An increase in blood volume increases central venous pressure. This increases right atrial pressure, right ventricular end-diastolic pressure and volume. This increase in ventricular preload increases ventricular stroke volume by the Frank-Starling mechanism. An increase in right ventricular stroke volume increases pulmonary venous blood flow to the left ventricular, thereby increasing left ventricular preload and stroke volume. An increase in stroke volume then increases cardiac output and arterial blood pressure.
Revised 4/25/2014
DISCLAIMER: These materials are for educational purposes only, and are not a source of medical decision-making advice.
Don’t Miss: Claritin Raise Blood Pressure