Prevalence Of Hypertension Among Heart Failure Patients
The prevalence of HTN as an HF etiology varies geographically and temporally . The findings from the Korean Heart Failure study, which recruited 3200 patients with HF from 2004 to 2009, showed that 36.7% of the patients had hypertensive HF . More recently, the findings from the Korean Acute Heart Failure study, which enrolled 5625 patients from 2011 to 2014, showed that only 4% of the patients had HF caused by HTN . Up to 30% of the patients in the Acute Decompensated Heart Failure National Registry had a hypertensive etiology, and this was more prevalent among the patients with normal EFs . The results from studies of other large dedicated HF registries have shown that HTN was the primary cause of HF in 1123% of the patients .
Table 1 Comparison of dedicated heart failure registries
Whether HTN is a cause or a contributor to the development of HF is not clear. Although a BP elevation alone may not be sufficient to trigger HF, it increases the risk of CV diseases progressing to HF. For example, the activation of neurohormonal pathways induced by a persistent BP elevation in addition to LV hypertrophy could lead to adverse modifications of postinfarct ventricular remodeling, rendering the heart vulnerable to the development of HF after a myocardial infarction . Factors, including an increased afterload, reduced arterial compliance, and the lack of a response to vasodilators, also affect cardiac output in the context of HF .
Articles On Heart Failure Types & Stages
Congestive heart failure doesn’t mean your heart has stopped. It means it’s not pumping blood the way it should. When that happens, blood and fluid can back up in your body and make it harder for your kidneys to flush out sodium and water. That can make you hold on to too much fluid, which causes swelling.
There’s no cure. But your doctor may give you medication to do things like lower your blood pressure, relax your blood vessels, make your heart beat stronger, or ease swelling. And diet and lifestyle changes — like not smoking — can help, too.
Blood Pressure And Heart Failure Prevention
Two issues arise regarding HF when treating HTN. The first is strictly controlling high BP to prevent structural remodeling and the development of HF. The presence of a J-curve association between BP and CV outcomes have been long debated, but evidence has been controversial . The current consensus is that strict control is mostly beneficial for hypertensive patients with low CV risk, while the risk of CV outcome increases in patients with high risk for coronary heart disease . Recently, the findings from the Systolic Blood Pressure Intervention Trial , which assessed the role of intensive HTN treatment on a composite outcome that included HF, showed that a target SBP< 120mmHg was associated with a 38% relative risk reduction in HF . BP lowering in patients with ventricular hypertrophy can delay further remodeling and reduce the incidence of HF . The LV hypertrophy induced by HTN is not unidirectional, and a regression of LV mass has been observed after the pharmacological treatment of elevated BP . Improvements in LV hypertrophy have also been associated with reduced risks of CV events, including CV death, myocardial infarction, and stroke .
Also Check: What Causes Change In Blood Pressure
Stage D And Reduced E
Patients with Stage D HF-rEF have advanced symptoms that do not get better with treatment. This is the final stage of heart failure.
Stage D treatment
The usual treatment plan for patients with Stage D heart failure includes:
- Treatments listed in Stages A, B and C.
- Evaluation for more advanced treatment options, including:
- Heart transplant.
- Research therapies.
Heart Failure From High Blood Pressure
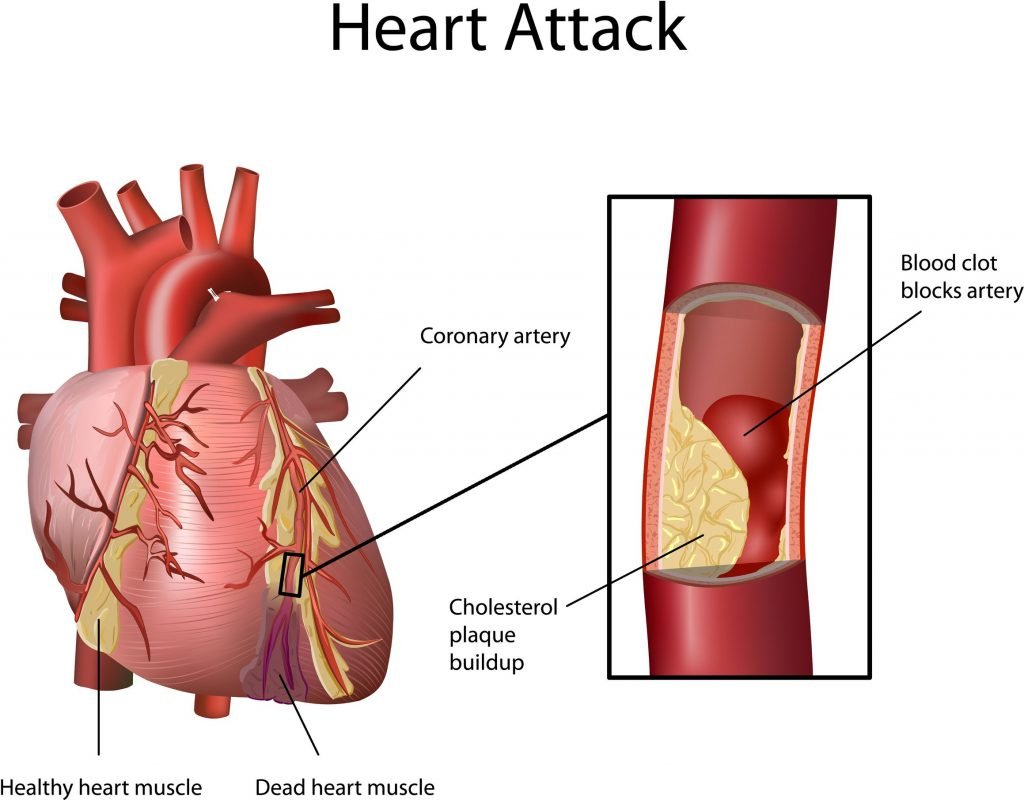
As the damage left by high blood pressure restricts blood flow, the heart is forced to work harder than ever to provide the body with adequate circulation. Eventually, all this hard work can cause thickening or stiffening of the heart, further impeding its capabilities. As the heart becomes weaker, heart failure can result.
While the type of heart failure can vary, it is most commonly seen as an enlarged left ventricle with signs of fluid build-up throughout the body. Symptoms often include shortness of breath, fatigue, and swelling of the ankles, legs, feet, abdomen, or veins in the neck.
Without fully understanding the potential dangers and health concerns, it can be difficult to appreciate why early and effective treatment of high blood pressure is so crucial. The damaging effects may not be immediately obvious, but complications can lurk, unseen for years. Preventative measures for those at risk and proactive care for diagnosed patients can help curb these risks and protect the heart and other vital organs from potentially irreparable damage.
If you are concerned about high blood pressure and the potentially deadly impact it can have on your heart, contact any location of Cardiovascular Institute of the South to schedule a consultation with one of our highly-trained and respected cardiologists.
You May Like: Shaking Low Blood Pressure
What Is High Blood Pressure
High blood pressure, also called hypertension, is blood pressure that is higher than normal. Your blood pressure changes throughout the day based on your activities. Having blood pressure measures consistently above normal may result in a diagnosis of high blood pressure .
The higher your blood pressure levels, the more risk you have for other health problems, such as heart disease, heart attack, and stroke.
Your health care team can diagnose high blood pressure and make treatment decisions by reviewing your systolic and diastolic blood pressure levels and comparing them to levels found in certain guidelines.
The guidelines used to diagnose high blood pressure may differ from health care professional to health care professional:
- Some health care professionals diagnose patients with high blood pressure if their blood pressure is consistently 140/90 mm Hg or higher.2 This limit is based on a guideline released in 2003, as seen in the table below.
- Other health care professionals diagnose patients with high blood pressure if their blood pressure is consistently 130/80 mm Hg or higher.1 This limit is based on a guideline released in 2017, as seen in the table below.
| systolic: 130 mm Hg or higherdiastolic: 80 mm Hg or higher |
If you are diagnosed with high blood pressure, talk with your health care team about your blood pressure levels and how these levels affect your treatment plan.
Can A Panick Attack Effect Oxygen Level
Can having a pannick attack effect the amount of oxygen in your body? Is this true?
Yeh if breathing changes, CO2 levels and oxygen change Kindest Regards
- Posts
- 434
During a pannick attack my level has went to 85% once, I know this seems pretty low but it came back up a minute or something later, and my general everydayoxygen levels are now 98-99% could the drop be caused by my attack?
- Posts
- 434
About 3-4 months a go I had a really bad pannick attack. I called the ambulance, and when the ambulance came they put that clip thing on my finger that measures your pulse rate and oxygen levels, when they first put it on obviously my heart rate was very high, then with me panicking even more wondering what is happening to me I was watching the screen that shown my pulse and ox levels and it went down to 85% then I started to really pannick! After about 20 seconds the 85% eventually went back up to normal and I started to calm down and my attack finished and I got took to hospital and then eveything was fine my ox level was 99% again! And every time I go to doctors they take my bp and oxygen levels, and my oxygen levels have always ever since been 98\99%! Im asking, do you think the drop of oxygen level was my pannick attack that made it go that way? Lol very confusing I know
- 22
You May Like: Claritin D And High Blood Pressure
What Is Cardiac Syncope
Cardiac or cardiovascular syncope is caused by various heart conditions, such as bradycardia, tachycardia or certain types of hypotension. It can increase the risk of sudden cardiac death.
People suspected of having cardiac syncope but who don’t have serious medical conditions may be managed as outpatients. Further inpatient evaluation is needed if serious medical conditions are present. Conditions that may warrant hospital evaluation and treatment include various cardiac arrhythmic conditions, cardiac ischemia, severe aortic stenosis and pulmonary embolism. If evaluation suggests cardiac vascular abnormalities, an ambulatory external or implantable cardiac monitor may be required.
Heart failure, atrial fibrillation and other serious cardiac conditions can cause recurrent syncope in older adults, with a sharp increase after age 70.
How Can I Prevent Left
Living a heart-healthy lifestyle can lower your risk of left-sided heart failure. If youve already experienced this condition, healthy habits can help you avoid future issues.
Steps you can take to prevent left-sided heart failure include:
- Get high blood pressure or coronary artery disease under control.
- Make time for regular physical activity and a good nights sleep.
- Maintain a healthy weight and eat fruits and vegetables.
- Manage stress with deep breathing or relaxation techniques.
- Quitting tobacco if you use it and avoiding secondhand smoke.
Also Check: Can Claritin Cause High Blood Pressure
Is There A Link Between Hbp And Heart Failure
Heart failure, a condition where your heart is unable to provide enough blood to the body, can take years to develop inside your body. The narrowing and blocking of blood vessels caused by high blood pressure increases your risk of developing heart failure.
- High blood pressure adds to your hearts workload: Narrowed arteries that are less elastic make it more difficult for the blood to travel smoothly and easily throughout your body causing your heart to work harder.
- Over time, a higher workload leads to an enlarged heart: In order to cope with increased demands, the heart thickens and becomes larger. While it is still able to pump blood, it becomes less efficient. The larger the heart becomes, the harder it works to meet your body’s demands for oxygen and nutrients.
Why Its Important To Know Your Ef
If you have a heart condition, it is important for you and your doctor to know your EF. Your EF can help your doctor determine the best course of treatment for you. Measuring your EF also helps your healthcare team check how well our treatment is working.
Ask your doctor how often you should have your EF checked. In general, you should have your EF measured when you are first diagnosed with a heart condition, and as needed when your condition changes.
Recommended Reading: Vinegar And High Blood Pressure
Damage To Your Arteries
High blood pressure can lead to your arteries becoming clogged up, reducing the blood flow around your body and back to your heart.
Your arteries are the large blood vessels that carry blood from your heart around your body, carrying oxygen and nutrients to your organs and muscles. Your arteries have a role in controlling your blood pressure, and your blood pressure can affect your arteries.
How do your arteries control your blood pressure?Your blood vessels contain muscles to help squeeze the blood around your body. These muscles respond to hormones, the flow of blood and signals from your brain, telling them to squeeze or relax.
- When the muscles squeeze, this narrows the blood vessels and your blood pressure will be higher.
- When the muscles relax, your blood vessels widen and your blood pressure will be lower.
How can high blood pressure damage your arteries?
High blood pressure can damage your blood vessel walls. Fats in the blood can collect in these damaged areas, clogging up the arteries and leading to atherosclerosis where the arteries become narrow and stiff, reducing the blood flow around your body.
The fatty, damaged areas are prone to rupture, and blood clots can form over them. Bits of the blood clot can break off, known as a thrombus, and can become lodged in a blood vessel, completely cutting off the blood supply to part of the body, including the heart, brain or legs.
Cardiovascular diseases include:
Outlook For Heart Failure
Heart failure is a serious long-term condition that’ll usually continue to get slowly worse over time.
It can severely limit the activities you’re able to do and is often eventually fatal.
But it’s very difficult to tell how the condition will progress on an individual basis.
It’s very unpredictable. Lots of people remain stable for many years, while in some cases it may get worse quickly.
Don’t Miss: What Causes Irregular Blood Pressure
Hf With Preserved Ejection Fraction
As no drug has convincingly shown to reduce morbidity or mortality in patients with HFpEF or HFmrEF thus far, the main aims of treatment are to alleviate symptoms and improve quality of life.w69 Despite the limited evidence available on treatment of hypertension in patients with HFpEF, guidelines recommend RAAS inhibition, with ACE inhibitor or ARB and especially MRA as first choice . Although diuretics are important in all patients with HF to control fluid retention, guidelines emphasise that they are essential components of the treatment regimen of all patients with hypertension and HFpEF.w70 However, close monitoring is essential because inappropriately low or high doses of diuretics can result in fluid overload or volume depletion, respectively, and the latter can increase the risk of hypotension, renal impairment and electrolyte disturbances. While nitrates are not recommended because they do not improve quality of life and may actually worsen functional status,w71 for all other common antihypertensive agents, including BBs, alpha-blockers and CCBs, the lack of evidence precludes making recommendations on their efficacy and safety. Therefore, the ultimate recommendation regarding choice of antihypertensive medication is shared decision-making, considering patients preferences and circumstances as well as clinicians judgement.
What Do The Numbers Mean
Ejection Fraction 55% to 70%
- Pumping Ability of the Heart: Normal.
- Level of Heart Failure/Effect on Pumping: Heart function may be normal or you may have heart failure with preserved EF .
Ejection Fraction 40% to 54%
- Pumping Ability of the Heart: Slightly below normal.
- Level of Heart Failure/Effect on Pumping: Less blood is available so less blood is ejected from the ventricles. There is a lower-than-normal amount of oxygen-rich blood available to the rest of the body. You may not have symptoms.
Ejection Fraction 35% to 39%
- Pumping Ability of the Heart: Moderately below normal.
- Level of Heart Failure/Effect on Pumping: Mild heart failure with reduced EF .
Ejection Fraction Less than 35%
- Pumping Ability of the Heart: Severely below normal.
- Level of Heart Failure/Effect on Pumping: Moderate-to-severe HF-rEF. Severe HF-rEF increases risk of life-threatening heartbeats and cardiac dyssynchrony/desynchronization .
Normal Heart. A normal left ventricular ejection fraction ranges from 55% to 70%. An LVEF of 65%, for example means that 65% of total amount of blood in the left ventricle is pumped out with each heartbeat. Your EF can go up and down, based on your heart condition and how well your treatment works.
HF-pEF. If you have HF-pEF, your EF is in the normal range because your left ventricle is still pumping properly. Your doctor will measure your EF and may check your heart valves and muscle stiffness to see how severe your heart failure is.
Read Also: Reversing Pulmonary Hypertension
The Heart And Nervous System
High blood pressure and high heart rate can be seen with exercise and emotional stress. This is because the sympathetic nervous system is activated for the fight-or-flight response. Due to stimulation from the nervous system, heart rate increases and blood vessels constrict to increase blood pressure.
Stages C And D With Preserved Ef
Treatment for patients with Stage C and Stage D heart failure and reserved EF includes:
- Treatments listed in Stages A and B.
- Medications for the treatment of medical conditions that can cause heart failure or make the condition worse, such as atrial fibrillation, high blood pressure, diabetes, obesity, coronary artery disease, chronic lung disease, high cholesterol and kidney disease.
- Diuretic to reduce or relieve symptoms.
YOU ARE THE MOST IMPORTANT PART OF YOUR TREATMENT PLAN!
It is up to you to take steps to improve your heart health. Take your medications as instructed, follow a low-sodium diet, stay active or become physically active, take notice of sudden changes in your weight, live a healthy lifestyle, keep your follow-up appointments, and track your symptoms. Talk to your healthcare team about questions or concerns you have about your medications, lifestyle changes or any other part of your treatment plan.
Don’t Miss: Can Pain Lower Blood Pressure
How The Normal Heart Works
The normal healthy heart is a strong, muscular pump a little larger than a fist. It pumps blood continuously through the circulatory system.
The heart has four chambers, two on the right and two on the left:
- Two upper chambers called atria
- Two lower chambers called ventricles
The right atrium takes in oxygen-depleted blood from the rest of the body and sends it through the right ventricle where the blood becomes oxygenated in the lungs.
Oxygen-rich blood travels from the lungs to the left atrium, then on to the left ventricle, which pumps it to the rest of the body.
The heart pumps blood to the lungs and to all the bodys tissues through a sequence of highly organized contractions of the four chambers. For the heart to function properly, the four chambers must beat in an organized way.
An Understanding Of The Basics
So, there are a couple of ways of determining your oxygen level. Your doctor may choose to do the more invasive ABG test. This will get an accurate PaO2 level for one point in time which can be very helpful.
However, the most common and easiest oxygen level to get is your SpO2. This can be checked at every doctor visit. A neat thing about pulse oximeters is they are easily portable. So, now we have devices that allow us to monitor your SpO2 while you are walking, and even while you are sleeping.
Now you understand the basic oxygen levels. You now know what oxygen levels are safe, or at least what oxygen level goals we are seeking.
You May Like: Does Spicy Food Cause High Blood Pressure