Prevalence And Temporal Trends Of Hypertension In Europe
Due to the difficulty of obtaining comparable results among countries, the World Health Organization Global Health Observatory represents an important source of data on the prevalence of hypertension and the mean SBP values among 51 European national populations. The first striking feature of these data is the similarity of the pattern of the association between blood pressure and age as well as between BP and sex in different countries. SBP progressively increases throughout life, with a difference of 2030 mmHg between early and late adulthood.6,7 DBP increases to a lower extent until the fifth decade, and then average DBP tends to remain constant or, more frequently, to decline slightly.6,8 For both SBP and DBP, the mean levels are higher in men than in women in early adulthood, although this difference narrows progressively and is either non-existent or reversed by the sixth or seventh decade.9,10
Figure 44.1.1 Prevalence of raised blood pressure in Europe in 2014. In males aged over 18 years in females aged over 18 years.
Adapted from11 with permission.
Why Is Hypertension Known As The Silent Killer
Blood pressure is an important part of your health. So, early detection is very important as it is a “”Silent Killer”” because it may show no symptoms. Hypertension puts one at the risk for heart disease, stroke, heart failure, and other diseases. High blood pressure is a long-lasting condition and requires immediate medication. The higher the BP, the higher the chance of serious complications.
How Hypertension Is Diagnosed
Hypertension is usually diagnosed during a routine body checkup. It is advisable to visit a general physician on the off chance that you develop high blood pressure. People who are between the age group of 18 to 39 and 40 years or older are at a higher risk of developing high blood pressure. An appropriate sized arm cuff is used to diagnose Hypertension. There are some machines available which can analyze your blood pressure levels for free.
You May Like: Claritan And High Blood Pressure
Too Much Sodium In Your Diet
Sodium is a chemical found in salt, plays a role in increasing blood pressure by promoting the retention of fluid by the body. This increases the pressure on the heart to work more. Some studies recommend an upper daily limit for sodium consumption of 1500 mg. Checking the sodium amount on food labels and menus can help you keep a track of how much sodium you are consuming. Launch meats and canned soups have particularly high levels of dietary sodium. Processed foods are high in sodium and makeup about 75% of our sodium intake.
How Do I Know If I Have High Blood Pressure
Theres only one way to know if you have high blood pressure: Have a doctor or other health professional measure it. Measuring your blood pressure is quick and painless.
Talk with your health care team about regularly measuring your blood pressure at home, also called self-measured blood pressure monitoring.
High blood pressure is called the silent killer because it usually has no warning signs or symptoms, and many people do not know they have it.
Recommended Reading: Mayo Clinic Blood Pressure
Can Hypertension Be Cured
No, Hypertension can’t be cured. It’s a chronic disease and in 90% of patients, the cause of Hypertension is unknown. It can be controlled with medication and with some modification in lifestyle and eating habits. It generally requires regular medical attention and regular follow up with your doctor.
Adopt a healthy lifestyle to control Hypertension:
- Balanced diet.
- Maintain body weight and waistline.
Pathophysiology Of Essential Hypertension
Hypertension where there is no underlying medical cause is termed primary or essential hypertension. What basically happens in essential hypertension is that the arterioles render unusual resistance to blood flow. Patients may experience few or no symptoms of hypertension at the beginning of the condition as there are still no major changes in the blood vessels or different organs.
Hypertension can start with the abnormal changes of the small and large vessels. The large vessels are involved in the following episodes:
1. Large vessels become twisty and sclerosed
2. The lumen narrows down
3. The extremities, brain and heart receives decreased blood supply
4. Large vessels eventually get obstructed or rupture resulting to hemorrhage
The small vessels on the other hand experience the following:
1. Diastolic blood pressure elevates
2. The inner most layer of the vessel are damaged
3. Fibrin gathers in the vessel
4. Local edema manifests
5. Clotting may follow
These processes results to diminished supply of blood and eventually loss of function of the retina, brain, kidneys and the heart.
1. Left ventricle will collapse and congestion follows.
2. Elevated diastolic pressure will bring forth congestion up to the lungs.
3. Pulmonary congestion will lead to right ventricular failure.
4. Systemic venous pressure may raise leading to congestion.
5. Venous congestion results to decreased kidney perfusion.
6. Kidney failure.
Recommended Reading: Mayo Blood Pressure
Inflammation And The Immune System
Inflammation makes an important contribution to the genesis of hypertension and related target organ damage. Inflammation is associated with increased vascular permeability and release of potent mediators, such as reactive oxygen species, NO, cytokines and metalloproteinases. Cytokines mediate the formation of neo-intima , thereby decreasing the lumen diameter of resistance vessels , and promoting vascular fibrosis, leading to increased vascular resistance and stiffness. Cytokines also affect renal tubular function by increasing local synthesis of angiotensinogen and angiotensin II, as well as promoting sodium and volume retention in hypertension. Matrix metalloproteinases stimulate the degradation of the extracellular matrix, allowing infiltration of immune cells through the vessel wall into the interstitium of the affected organs, promoting apoptosis and enhancing collagen synthesis and matrix deposition, leading to target organ damage.
What Is The Importance Of Pathophysiology
In many ways, pathophysiology is the basis of the nursing practice, as it helps build a strong foundation for a nurses main responsibilities, such as ordering diagnostic tests, treating acute and chronic illnesses, managing medications, and managing general health care and disease prevention for patients and their
You May Like: Will Claritin Raise Blood Pressure
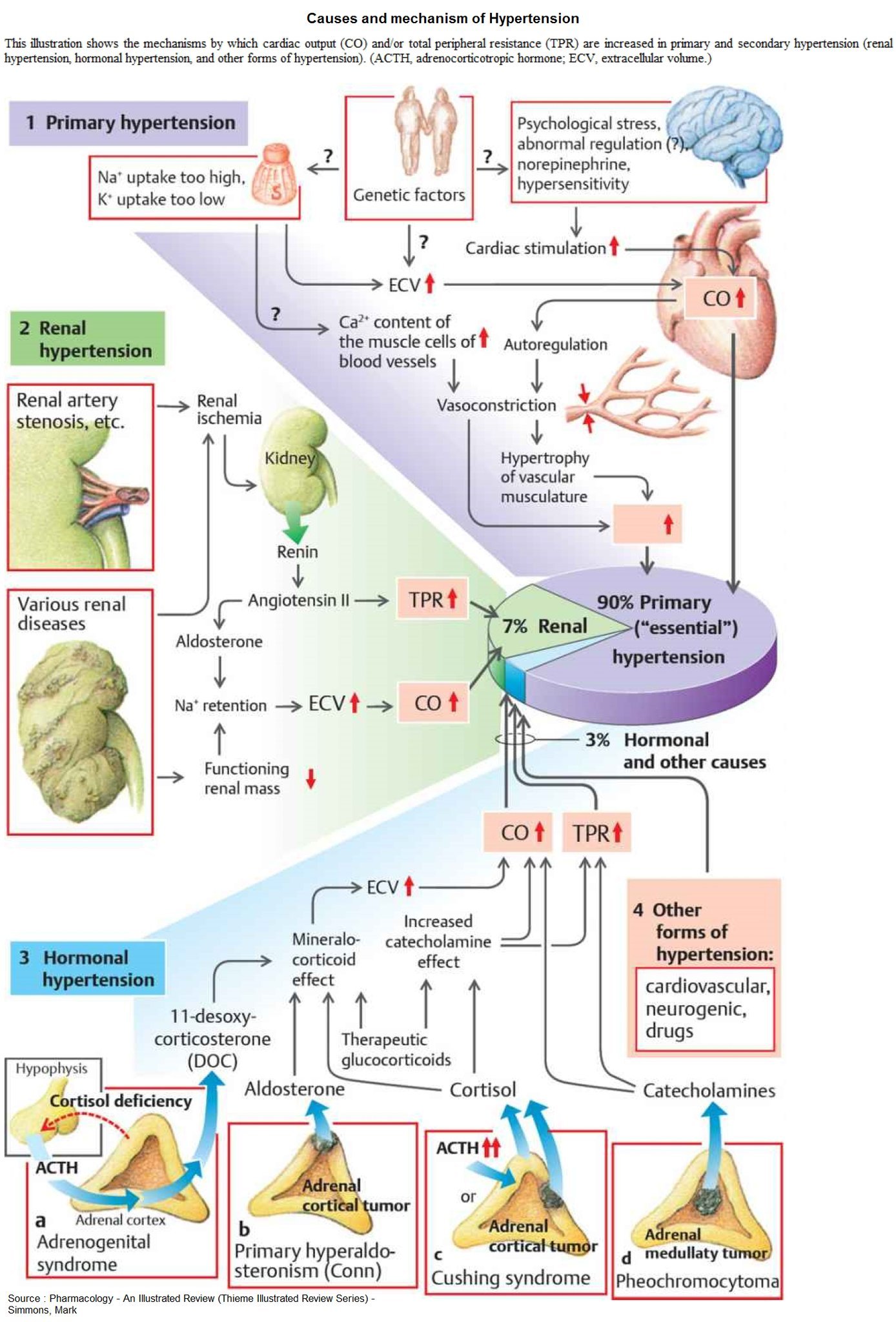
What Causes High Blood Pressure
According to Dr. Singh, hypertension is broken down into two types: primary and secondary. Primary hypertension, also called essential hypertension, has no identifiable cause and is the most common form of high blood pressure. Disposition towards primary hypertension is mostly attributed to:
- General aging
- Genetics
- Poor diet
Genetic factors, as well as lifestyle choices to diet and exercise, may contribute to the development of primary hypertension, Dr. Singh says.
Secondary hypertension, on the other hand, occurs when the elevation in pressure has a readily identifiable underlying condition,” explains Dr. Singh. Those causes can include:
- Poor diet
- An underlying condition such as:
- Kidney disease
Etiology Of Essential Hypertension
Essential hypertension may be attributed to multiple factors, including genetic predisposition, excess dietary salt intake, and adrenergic tone, that may interact to produce hypertension. Essential hypertension accounts for 90% of human hypertension and can evolve into secondary hypertension, as renal function decreases. Thus, the distinction between primary and secondary forms of hypertension is not always clear in patients who have had uncontrolled hypertension for many years.
Long-term regulation of daily blood pressure is closely linked with salt and water homeostasis. Increased BP raises renal sodium and water excretion, often called renal-pressure natriuresis or diuresis. Increased salt intake in persons who have normal kidney and neurohormonal functions has an insignificant effect on BP changes. These individuals are called âsalt resistant.â In contrast, in âsalt-sensitiveâ individuals with impaired kidney function, because of abnormal neurohormonal control or intrinsic kidney abnormalities, increased BP and subsequent pressure natriuresis or diuresis provide another means of maintaining salt and water balance. That is, sodium balance is maintained at a higher BP in patients with primary hypertension, indicating that pressure natriuresis has been reset.
There are two types of genetic causes of hypertension: rare familial monogenic hypertensive disorders and classic quantitative trait form.
Syndromes with elevated aldosterone level include the following:
Also Check: Symptoms Of Increased Blood Pressure
Heart Attack And Heart Disease
High blood pressure can damage your arteries by making them less elastic, which decreases the flow of blood and oxygen to your heart and leads to heart disease. In addition, decreased blood flow to the heart can cause:
- Chest pain, also called angina.
- Heart attack, which happens when the blood supply to your heart is blocked and heart muscle begins to die without enough oxygen. The longer the blood flow is blocked, the greater the damage to the heart.
- Heart failure, a condition that means your heart cant pump enough blood and oxygen to your other organs.
Who Is At Risk Of Developing Hypertension
On the basis of the causes and risk factors mentioned above, if one needs to determine who is more at risk of developing hypertension. Then it could be-
- A person who has a family member with high blood pressure condition
- African American person
- A person of age above 55.
- Someone who is overweight or has an inactive lifestyle
- A person who eats foods high in sodium or salt
- A smoker
Recommended Reading: Can Claritin D Cause High Blood Pressure
What Are The Symptoms Of High Blood Pressure
Unfortunately, there are no specific and overt symptoms of high blood pressure.
It is for this very reason that hypertension is often called the silent killer, Dr. Singh says.
Though hypertension in and of itself is asymptomatic, if left untreated, it can lead to organ damage. From there, different diseases can develop with harmful symptoms.
Common examples include chest pain associated with heart attacks or weakness and dizziness that occur during strokes, Dr. Singh says.
Vasoreactivity And The Role Of The Vascular Endothelium
The vasoreactivity of the vascular bed, an important phenomenon mediating changes of hypertension, is influenced by the activity of vasoactive factors, reactivity of the smooth muscle cells, and structural changes in the vessel wall and vessel caliber, expressed by a lumen-to-wall ratio.
The vascular endothelium is considered to be a vital organ, in which synthesis of various vasodilating and constricting mediators occurs. The interaction of autocrine and paracrine factors takes place in the vascular endothelium, leading to growth and remodeling of the vessel wall and to the hemodynamic regulation of BP.
Numerous hormonal, humoral vasoactive, and growth and regulating peptides are produced in the vascular endothelium. These mediators include ET, Ang II, bradykinin, NO, and several other growth factors.
ET is a potent vasoconstrictor in humans and impairs renal pressure natriuresis. ET-1 is the predominant isoform and stimulates ET type A receptor. Chronic ET-1 activation of ETA receptors in the kidneys may play a major role in the pathogenesis of hypertension. Bosentan and other ET-1 receptor antagonists have been beneficial in patients with pulmonary arterial hypertension however, their role in the management of essential hypertension is limited because of their side effects, which include fluid retention and edema.
Don’t Miss: What Heart Problems Cause Low Blood Pressure
Activation Of The Renin
Activation of the RAS via enhanced hepatic production of angiotensinogen has been described. Angiotensinogen, which is highly expressed in adipose tissues when other components of the RAS system are present, is able to generate angiotensin II and other vasoactive peptides. Low or suppressed renin levels are nevertheless quite usual in CS patients due to the negative feedback exerted by cortisol’s mineralocorticoid activity, suggesting that there is a different activation mechanism . In fact, CS patients show a greater sensitivity to angiotensin II and its pressor activity at the peripheral levels. Glucocorticoids also enhance angiotensin II’s action as a neurotransmitter leading to elevated sympathetic nerve activity, stimulating vasopressin release, and attenuating the arterial baroreceptor reflex .
Sodium/potassium Ratio Hypothesis Of Essential Hypertension
A 2007 review article states that while excessive sodium consumption has long been recognized as contributing to the risk of hypertension, “potassium, the main intracellular cation, has usually been viewed as a minor factor in the pathogenesis of hypertension. However, abundant evidence indicates that a potassium deficit has a critical role in hypertension and its cardiovascular sequelae.” The authors state that modern, western, high sodium, low potassium diets result in corresponding changes in intracellular concentration of these, the two most important cations in animal cells. This imbalance leads to contraction of vascular smooth muscle, restricting blood flow and so driving up blood pressure. The authors cite studies which showing that potassium supplementation is effective in reducing hypertension.
Epidemiological support for this hypothesis can be found in a 2014 meta-analysis which states that “the sodium-to-potassium ratio appears to be more strongly associated with blood pressure outcomes than either sodium or potassium alone in hypertensive adult populations.”.
Recommended Reading: Does Apple Watch Detect Blood Pressure
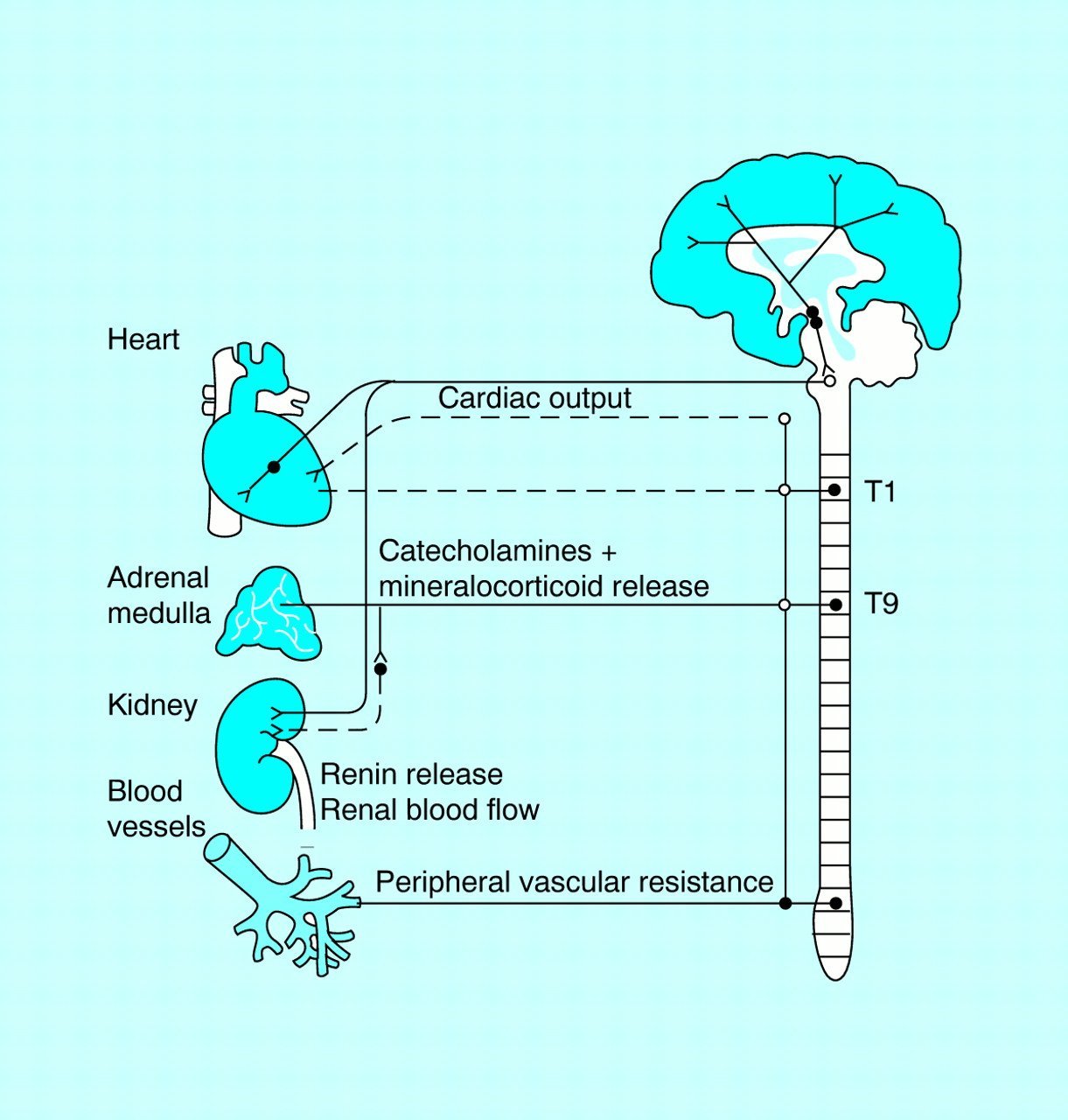
Cardiac Output And Peripheral Resistance
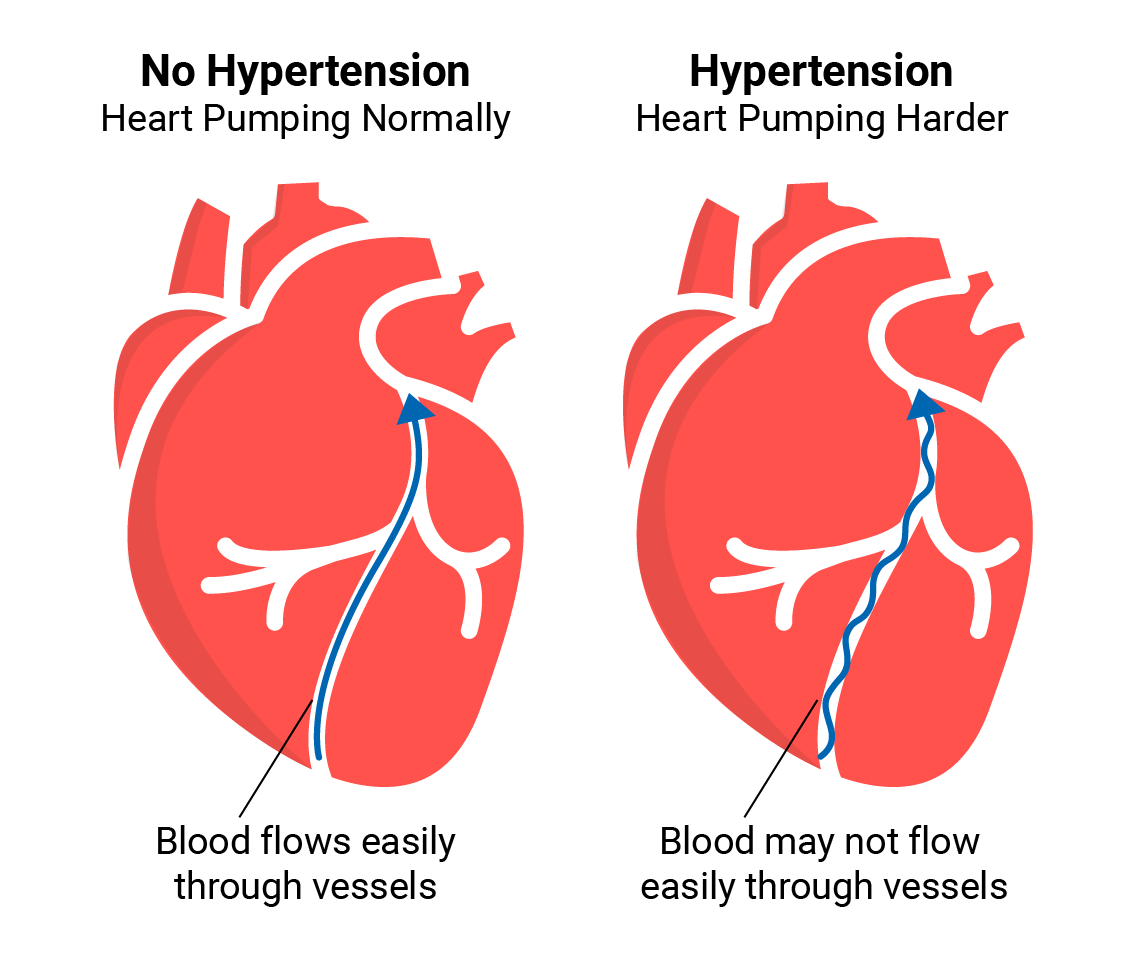
Maintenance of a normal blood pressure is dependent on the balance between the cardiac output and peripheral vascular resistance. Most patients with essential hypertension have a normal cardiac output but a raised peripheral resistance. Peripheral resistance is determined not by large arteries or the capillaries but by small arterioles, the walls of which contain smooth muscle cells. Contraction of smooth muscle cells is thought to be related to a rise in intracellular calcium concentration, which may explain the vasodilatory effect of drugs that block the calcium channels. Prolonged smooth muscle constriction is thought to induce structural changes with thickening of the arteriolar vessel walls possibly mediated by angiotensin, leading to an irreversible rise in peripheral resistance.
It has been postulated that in very early hypertension the peripheral resistance is not raised and the elevation of the blood pressure is caused by a raised cardiac output, which is related to sympathetic overactivity. The subsequent rise in peripheral arteriolar resistance might therefore develop in a compensatory manner to prevent the raised pressure being transmitted to the capillary bed where it would substantially affect cell homeostasis.
Factors Influencing Bp Regulation
Regulation of normal blood pressure is a complex process. Arterial BP is a product of cardiac output and peripheral vascular resistance. Cardiac output is the product of stroke volume and heart rate. The factors affecting cardiac output include sodium intake, renal function, and mineralocorticoids. The inotropic effects occur via extracellular fluid volume augmentation and an increase in heart rate and contractility.
Peripheral vascular resistance is dependent upon the sympathetic nervous system , humoral factors, and local autoregulation. The vasculature is highly innervated by sympathetic fibers. The SNS produces its effects via the vasoconstrictor alpha effect or the vasodilator beta effect. Along the same line, the renal artery is highly innervated, with the sympathetic activation promoting sodium retention via increased renin secretion.
Similarly, the role of the arterial baroreflex system in moment-to-moment regulation of BP is well known. Although electrical stimulation of baroreceptors can cause significant reduction in BP in humans with treatment-resistant hypertension, its importance in long-term BP control remains controversial. These studies confirm the role of the SNS as a component in the pathogenesis of hypertension.
Don’t Miss: Claritin D Blood Pressure
Pathophysiology Of Hypertensive Retinopathy
- 3 Dr. Tso is a Research to Prevent Blindness-William Friedkin Scholar.Mark O.M. TsoCorrespondenceReprint requests to Mark O.M. Tso, MD, Department of Ophthalmology, University of Illinois Hospital Eye and Ear Infirmary, 1855 West Taylor Street, Chicago, IL 60612.Footnotes* Supported in part by Public Health Service Grants EY01903, EY01904, EY2183 and core grant IP30 EY017923 Dr. Tso is a Research to Prevent Blindness-William Friedkin Scholar.Affiliations
Vascular Oxidative Stress And Hypertension
A variety of enzymatic and non-enzymatic sources of ROS exist in blood vessels. The best-characterized source of ROS is NADPH oxidase. In addition to NADPH oxidase, several other enzymes may contribute to ROS generation, including xanthine oxidase, NO synthase and mitochondrial enzymes.
NADPH oxidase: NADPH oxidase is the primary biochemical source of ROS, particularly superoxide, in the vasculature. The kidney and vasculature are rich sources of NADPH oxidase-derived ROS, which have an important role in renal dysfunction and vascular damage under pathological conditions., This system catalyses the reduction of molecular oxygen by NADPH, which functions as an electron donor, thus generating superoxide. NADPH oxidase is upregulated in hypertension by humoral and mechanical signals. AT-II is the most studied stimulus of the upregulation of NADPH oxidase, but ET-1 and urotensin II may also participate to the activation of NADPH oxidase, thereby resulting in increased ROS. It is likely that the most well-known function of NADPH oxidase-derived superoxide is the inactivation of NO in the reaction that forms peroxynitrite, which leads to impaired endothelium dependent vasodilation and the uncoupling of endothelial NO synthase to produce additional superoxide., In the vasculature, the activation of NADPH oxidase has been strongly associated with hypertension.
Recommended Reading: Claritin Side Effects Blood Pressure
Can You Live A Long Life With Hypertension
Hypertension is also called the ‘silent killer’. If you leave Hypertension untreated there is a higher chance of death within a year. High blood pressure has an average survival rate of 10 months. It can even lead to stroke, blindness, heart attack, and kidney disease. So, it is advised to keep your bp level in the normal range and always keep a check on your level of Blood pressure.
Pathogenesis Of Essential Hypertension
The pathogenesis of essential hypertension is multifactorial and highly complex. The kidney is both the contributing and the target organ of the hypertensive processes, and the disease involves the interaction of multiple organ systems and numerous mechanisms of independent or interdependent pathways. Factors that play an important role in the pathogenesis of hypertension include genetics, activation of neurohormonal systems such as the sympathetic nervous system and renin-angiotensin-aldosterone system, obesity, and increased dietary salt intake.
Arterial hypertension is the condition of persistent elevation of systemic blood pressure . BP is the product of cardiac output and total peripheral vascular resistance. Multiple factors are involved in short-term and long-term regulation of BP for adequate tissue perfusion these include the following:
-
Cardiac output and circulatory blood volume
-
Vascular caliber, elasticity, and reactivity
-
Humoral mediators
-
Neural stimulation
Over the course of its natural history, essential hypertension progresses from occasional to established hypertension. After a long, invariable, asymptomatic period, persistent hypertension develops into complicated hypertension, in which target organ damage to the aorta and small arteries, heart, kidneys, retina, and central nervous system is evident.
Go to Hypertension, Hypertensive Heart Disease, and Hypertensive Emergencies for more complete information on these topics.
Also Check: What Can You Take To Lower Blood Pressure