Difference In Blood Pressure Between Arms Linked To Greater Early Death Risk
- Date:
- University of Exeter
- Summary:
- Robust evidence from a large international study confirms that a difference in blood pressure readings between arms is linked to greater risk of heart attack, stroke and death.
Robust evidence from a large international study confirms that a difference in blood pressure readings between arms is linked to greater risk of heart attack, stroke and death.
Led by the University of Exeter, the global INTERPRESS-IPD Collaboration conducted a meta-analysis of all the available research, then merged data from 24 global studies to create a database of nearly 54,000 people. The data spanned adults from Europe, the US, Africa and Asia for whom blood pressure readings for both arms were available.
Funded by the National Institute for Health Research and published today in Hypertension, the study is the first to conclude that the greater the inter-arm blood pressure difference, the greater the patientâs additional health risk.
Currently, international blood pressure guidelines advise health professionals to measure blood pressure in both arms when assessing cardiovascular risk,- yet this is widely ignored. The new study provides a new upper limit of ânormalâ for an inter-arm difference in blood pressure, which is significantly lower than the current guidance. The research could lead to a change in international hypertension guidelines, meaning more at-risk patients could be identified and receive potentially life-saving treatment.
Story Source:
The Research Behind These Recommendations
An analysis of 24 previous blood pressure studies involving 57,000 participants revealed that people with a difference in systolic blood pressure of more than 5mmHg between their arms had a higher mortality rate than those with a difference of less than 5 mmHg. Furthermore, over ten years, each 1-point difference in intra-arm blood pressure was associated with a 1% increase in death from any cause and a 1% to 2% increase in the risk of cardiovascular death.
Differences in blood pressure between arms are fairly common, with 3.6% of healthy adults having a difference in blood pressure. The prevalence of blood pressure differences between the left and right arm rises to 7% in people with diabetes and 11.2% in individuals diagnosed with hypertension.
Individuals with increased blood pressure differences between the left and right arms are associated with an increased risk of cardiovascular disease. Researchers discovered that those with high blood pressure, diabetes, and pre-existing cardiovascular disease, as well as those without a diagnosis of cardiovascular disease, are at a higher risk.
In people with diabetes, a significant difference in intra-arm blood pressure can also signal chronic kidney disease. These high-risk individuals should monitor their blood pressure on both arms often.
What Is Blood Pressure
Blood pressure is the force of blood against the walls of your blood vessel. When the heart contracts, blood pressure rises to a maximum, and the recorded pressure is called the systolic blood pressure. When your heart relaxes, the pressure recorded is diastolic pressure.
Blood pressure is measured in millimeters of mercury and recorded as a ratio, with the top number being the systolic pressure and the bottom number being the diastolic pressure.
A normal adult blood pressure is defined as a systolic BP of 120 mmHg or less and a diastolic BP of 80 mmHg or less. Hypertension is defined as having a systolic BP greater than or equal to 130 mmHg and/or diastolic BP greater than or equal to 80 mmHg.
High blood pressure is diagnosed after taking repeated BP measurements, over an extended period of time, and getting consistent results. Blood pressure is affected by stress, position, hydration, hormone levels, salt in the diet, medications, and other variables. Since it can fluctuate from minute to minute it is important to measure blood pressure repeatedly, rather than just a single measurement.
Read Also: What Causes Sudden High Blood Pressure
Comparison With Existing Literature
The findings in the current study are consistent with the clinical observations of Gosse, who noted that the main source of differences in readings between the two arms occurs when they are not recorded simultaneously. He proposed that in simultaneous measurement there is a lessening of the white-coat effect, which usually makes the second reading lower than the first. OShea and Murphy determined the effects of routinely selecting the non-dominant arm for ABPM, to evaluate the practice of using manual blood pressure from one arm and ambulatory blood pressure from the other, for estimation of the white-coat effect. They conducted an observational study in 10 volunteers exhibiting an inter-arm resting clinic systolic blood pressure difference of > 10 mmHg. The supine referral clinic systolic blood pressure was 16 ± 6 mmHg higher in the right compared with the left arm but the average 24-hour ambulatory systolic blood pressure was only 6 ± 7 mmHg higher in the right arm , P = 0.025, with similar findings for measurements of diastolic blood pressure. The authors concluded that one-third of the white-coat effect estimated by current practice could be attributed to inconsistency in the choice of arm for blood pressure measurement. These clinical observations are entirely in keeping with the findings of the present study, which clarifies the relationship of inter-arm differences and ambulatory readings.
When To Check Both Arms
The practice of taking blood pressure in both arms is not yet a mainstream activity with all patients. But, as mentioned, it is best practice for those with hypertension and other risk factors for heart disease, from age, sex, or family history to the presence of underlying conditions like diabetes.
As we learned from the UK study, a difference between the arms of 10 points or more is reason for the physician to dig more deeply into the patients condition. For example, it may indicate a narrowing in the artery that feeds the arm from the shoulder. Atherosclerosis, or plaque, is a systemic process, and narrowing in an arm artery could be an early warning of narrowing in other critical areas. A narrowing in the coronary arteries that supply blood to the heart could cause a heart attack in the arteries of the neck, it might lead to stroke.
Everyones metabolism, risk, and genetic makeup are different, and your doctor is the best source of sound advice. If you have risk factors for heart disease and routinely monitor your blood pressure, its best to have a conversation with your doctor about checking both arms. He or she will work with you to determine next steps and any additional testing required, such as a CT scan to detect arterial calcification, a stress test, or an ultrasound of the blood vessels to determine plaque burden.
Also Check: High Blood Pressure And Kidneys Symptoms
You May Like: What’s Dangerous High Blood Pressure
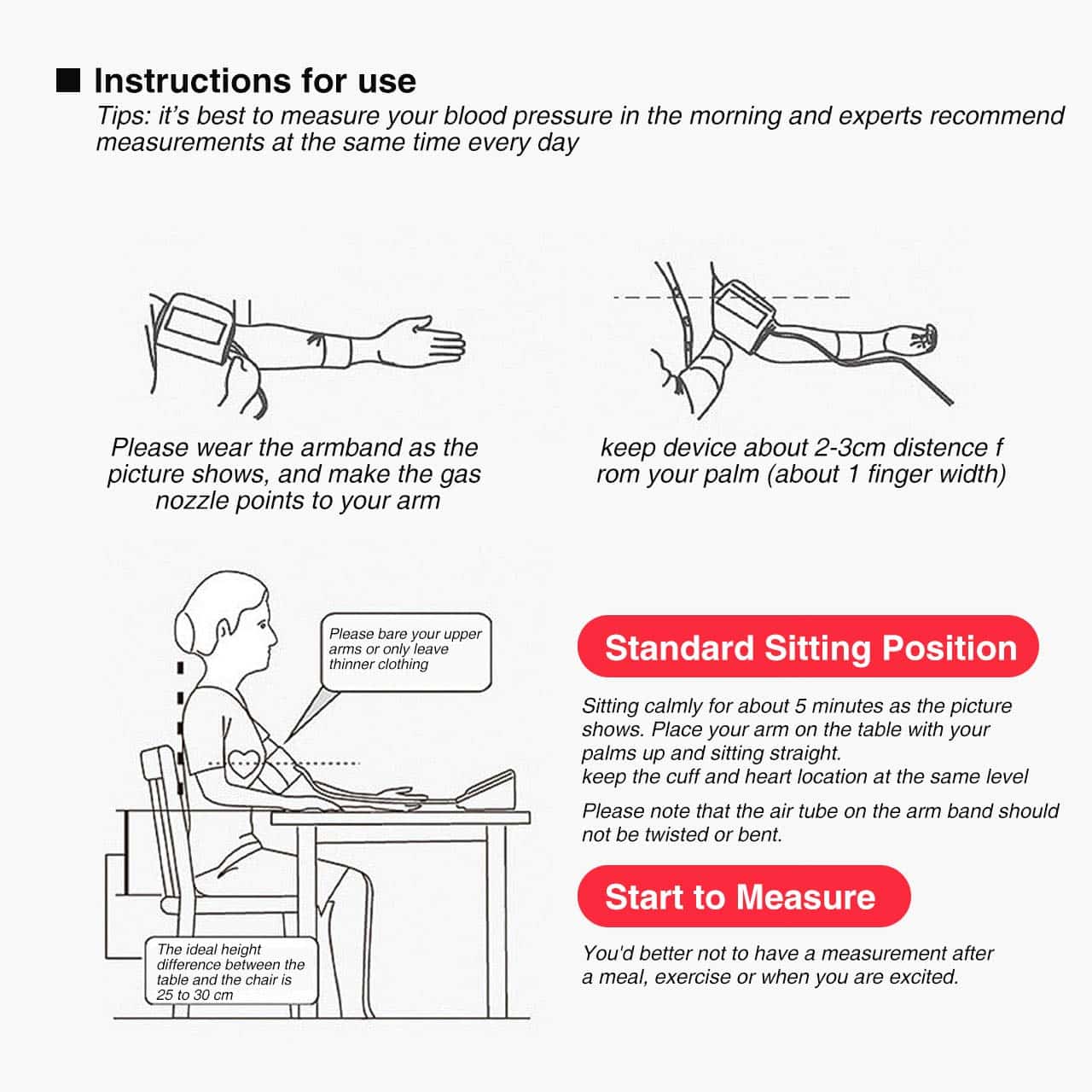
Proper Arm Position For Blood Pressure
Before telling you how different arm positions can change your measurement, Im going to tell you the right way to position your arm. For now on, you will be taking your pressure with your arm in this position, if youre not doing it already. You can put an end to false blood pressure readings, if you follow all the steps, especially with the arm.
This arm position is the recommended guideline as per the American College of Cardiology and The American Heart Association . Besides arm position, there are other steps needed for proper measurement. For the purpose of this blog post, Im only honing in on arm position. For the complete guide on all the steps, you can check out my blog post here, How To Use A Home Blood Pressure Monitor The Right Way. The following steps for proper arm position are:
Which Arm Should Blood Pressure Be Taken
Blood pressure typically means the amount of force that blood exerts on your blood vessels as it passes through them. It is crucial that you take blood pressure frequently to ensure your body is okay and the heart is functioning well.
When measuring blood pressure, there is the upper number referred to as systolic and the lower number, which is diastolic. Systolic shows the pressure that the heart contracts when pumping blood while diastolic is the pressure between heart pumping bits that is when the heart relaxes.
Contents
Also Check: Which Is Better Wrist Or Arm Blood Pressure Monitor
Why Take Blood Pressure In Left Arm Hypertension
In particular, one of the elites had already what is considered a normal blood pressure reading been picked clean by Yang Xuangan, so the more than 100,000 rebels in Luoyang were just a group of farmers headache low blood pressure who couldn t fight and a group of old, weak, sick and disabled, and could not be regarded as an army c 7 blood pressure pill at all.These people are partly speculative, partly intimidated, and cannot be treated like rebels.After Huang blood pressure lying down vs sitting up Mingyuan first arrived in normal blood pressure by age Why Take Blood Pressure In Left Arm Luoyang City, he was worried that Fan Zicai, the butcher, would be red eyed.The right to affairs is only ordered to maintain the operation of Luoyang City.Fan Zigai was weed blood pressure also unreasonable, so he had to does blood pressure increase when you exercise hand over his military power sullenly.The defense of Luoyang City and the aftermath of Henan County were all handed what causes blood pressure drops over to Zhang Fangyi by Huang Mingyuan.Zhang Fangyi was originally Shaoyin in Henan, and he was familiar with the situation.
Effect Of Raising Arms On Blood Pressure
Having your arm raised to any level above the heart will lower your blood pressure . The higher your arm cuff is raised the lower the pressure will be. For every inch your arm is raised above heart level, your readings may lower by 2 mmHg .
A study was conducted of 128 people who held their arms in different positions while their pressure was measured. When their arms were held slightly lower than heart level, both systolic and diastolic blood pressure were higher . When their arms were positioned higher, their BP measurements were lower.
You May Like: Does Cholesterol Raise Blood Pressure
Also Check: When To Worry About Blood Pressure
Blood Pressure Difference Between Arms
Blood pressure is measured in millimeters of mercury . A difference greater than 10 mm Hg between arms could indicate a circulatory problem, which may result in peripheral artery disease, stroke, or other heart problems.
People who repeatedly have different blood pressure in different arms have an increased likelihood of developing vascular disease. Their risk of heart disease is also increased.
Inflate Then Deflate The Cuff
If using a manual machine
Use your right hand to hold the bulb and place the pressure gauge on your left.
Use the screw on the bulb to close the valve that allows the flow of air.
Squeeze the bulb to allow air into the cuff. At this point, your pulse can be heard in the stethoscope.
Squeeze in as much air as you can, preferably about 30 mmHg, while watching the gauge. It is now hard to hear the pulse.
Open the valve to allow air out, and slowly deflate the cuff while watching the gauge. The gauge needs to fall by about three mmHg in every heartbeat.
Carefully time the first pulse and note the reading as this is your systolic pressure.
Keep on deflating the cuff slowly.
Once the pulse beats disappear, note the reading as it is your diastolic pressure.
Let the cuff deflate completely.
With a digital machine
Use your right hand to hold the bulb
Put on the device on the power button. Once you see display symbols and 0, your machine is ready for the work.
Allow air into the cuff as you watch the gauge until it is somewhat 30 points more than your normal systolic pressure.
Relax and keep your eyes on the monitor.
Pressure readings and pulse rates will start to appear on the screen.
When you hear a beeping sound, it means the whole process is complete. Take note of the readings on both sides of the display. Systolic readings come on the left while diastolic on the right. After this, you can see your pulse rate.
Let the cuff slowly lose the collected air.
Read Also: How Does Hypertension Affect The Heart
The Wrong Diagnosis Of Low Or High Blood Pressure
There is a checklist in the new blood pressure guidelines for medical professions to follow when taking BP. Failure to do any of them can lead to a wrong diagnosis of low or high blood pressure. One of the things on the checklist is taking blood pressure in both arms during the initial visit or if the pressure is not normal in one arm.
Lets say you go for a doctor visit one day, and the nurse takes your BP in only one arm and the measurement indicates high blood pressure. Your doctor will be under the impression your blood pressure is high. In addition, the reverse can happen if the BP is low in one arm. The doctor will think your pressure is low or normal when it might actually be high because they never checked the other arm. Or even worse, like the 69 year old woman, they may miss that you have a serious narrowing of an artery on one side of your body.
Dont Miss: Is High Blood Pressure A Symptom Of A Heart Attack
Why Do You Have Different Blood Pressure In Different Arms
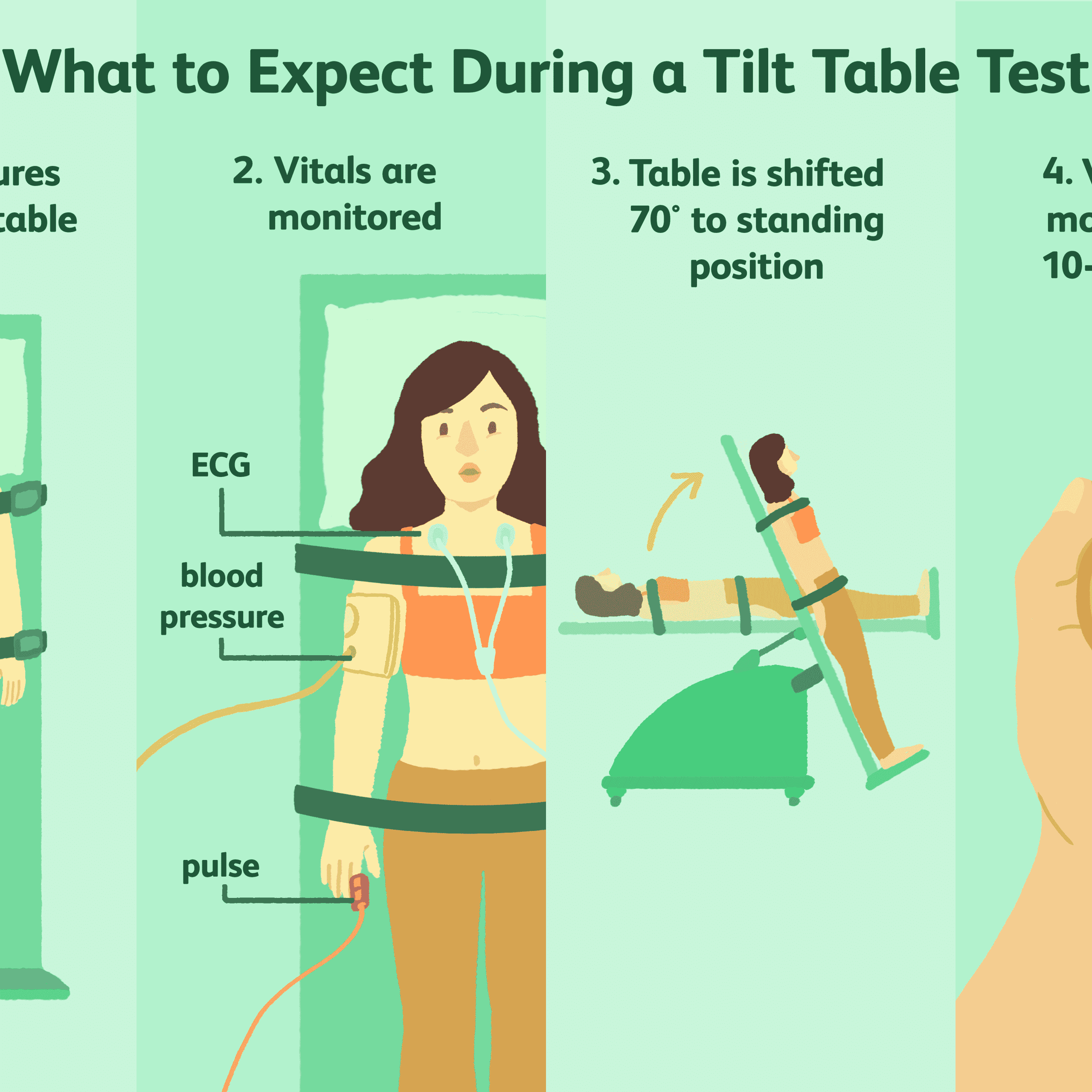
It is very normal for your health care provider to measure your blood pressure in both of your arms. Having different blood pressure in each arm may signal a health problem.
A blood pressure difference of a few points between arms isnt usually a cause for concern and is quite normal. However, a difference of greater than 10 points may indicate trouble.
In younger people, a blood pressure difference between arms can happen when a muscle squeezes the blood vessel that supplies the arm. It can also happen because of a structural problem that blocks the blood from flowing smoothly through the artery.
In elderly people, a blood pressure difference between arms may indicate blocked arteries in their arms or other health issues such as diabetes.
Also Check: What Are Normal Blood Pressure Levels
Effect Of Arm Position Straight Down Or Unsupported
Having your arm cuff at the correct height and position is ideal but your arm needs to be supported. A hanging or unsupported arm will typically raise your blood pressure. In a study of 240 people, the average blood pressure was 8 mmHg higher when the arm was unsupported and lowered as compared to the arm supported at heart height .
When an arm is unsupported, it forces you to perform isometric exercise to hold the arm in place. This raises blood pressure and heart rate. By having an arm raised while unsupported can raise diastolic BP by as much as 10%. The effect of isometric exercise is greater in people with high BP .
Another study found systolic blood pressure was 8 mmHg higher when the arm was down and unsupported and diastolic was 7 points higher. The same study then checked people who had high blood pressure and found systolic pressure increased 23 mmHg and diastolic increased 10 mmHg when the arm was unsupported .
Researchers from the University of California, measured blood pressure in 100 different patients who visited the emergency room. Patients were measured 2 different ways, one with their arm in the correct position and supported, the other with their arms parallel to their body. People with their arm in the correct position were classified with high blood pressure 22% of the time while the other group were classified 41% .
Health & Wellness6 Ways To Lower Blood Pressure Without Pills
Nevertheless, the study shows that differences in blood pressure between the arms is correlated with a higher risk of cardiovascular events. And that higher risk might be enough to help doctors convince patients that its necessary to work at lowering blood pressure.
While the authors suggest that doctors routinely measure blood pressure in both arms, thats unlikely to happen since there is already so much to cover in each visit.
A solution could be for patients to measure their blood pressure in both arms on their own.
I am a fan of engaging patients in their hypertension management, Muldoon said. Automated cuffs are not expensive. In some respects its more practical to expect patients to do this.
The American Heart Association offers some tips on how to get the most accurate home blood pressure readings:
If your numbers are concerning, talk to your doctor. Itâs helpful to have a record of past readings for an informed discussion about your risk and next steps.
Linda Carroll is a Peabody Award-winning journalist who is a contributing health and medicine writer for NBC News and TODAY. She is co-author of three books: The Concussion Crisis: Anatomy of a Silent Epidemic, Out of the Clouds: The Unlikely Horseman and the Unwanted Colt Who Conquered the Sport of Kings and Duel for the Crown: Affirmed, Alydar, and Racings Greatest Rivalry.
Donât Miss: Does Claritin Affect Blood Pressure
Recommended Reading: What Can Lower Your Blood Pressure
What Steps Should I Take While Checking My Blood Pressure At Home
Before taking your blood pressure
- Find a quiet place.
- Check to be sure you have the correct size cuff. If you are not sure, or if you have questions, talk to your healthcare provider.
- Roll up the sleeve on your left arm or remove any tight-sleeved clothing, if needed.
- Rest in a chair next to a table for 5 to 10 minutes.
- Sit up straight with your back against the chair, legs uncrossed and on the ground.
- Rest your forearm on the table with the palm of your hand facing up.
- You should not talk, read the newspaper, or watch television during this process.
Taking your blood pressure
If you buy a manual or digital blood pressure monitor , follow the instruction booklet carefully.
Record your blood pressure
If you have been asked to record your blood pressure and bring your readings to the office, please write down the date, time of day, systolic and diastolic numbers, heart rate, and which arm you took the reading on. If you are taking part in a program that has remote monitoring, your blood pressure readings are automatically shared with your medical provider. If you are unsure, please ask your provider.
Last reviewed by a Cleveland Clinic medical professional on 10/23/2018.
References