Learn The Warning Signs Of Serious Complications And Have A Plan
Even with treatment, pulmonary hypertension may lead to serious complications such as heart failure and arrhythmias. Know the signs and symptoms of pulmonary hypertension and how to recognize the possible complications.
If you are taking a blood thinner, this will increase your risk of bleeding. If you experience any abnormal bleeding, such as blood in your stool, black stool, or coughing up blood, contact your doctor right away. If you fall while taking a blood thinner, you are at higher risk for bleeding inside your head. Let your doctor know if you have fallen while taking a blood thinner.
Some treatments for pulmonary hypertension must be given through a long-term intravenous line. Call your doctor right away if you have any signs of infection. Signs of infection include redness, swelling, or yellow discharge where the IV is inserted a fever of 100.3°F or higher and chills.
- consuming a heart-healthy diet consisting of fruits, vegetables, and whole grains
- reaching or maintaining a moderate weight
Although physical activity is important for health, a person should avoid lifting heavy weights or doing other activities that cause strain.
PAH is a progressive condition, which means that the condition will worsen over time.
A 2012 evaluation found that in the last 20 years, the survival rate for PAH has improved.
The researchers behind the evaluation reported the following survival rates for individuals with PAH of unknown cause:
Do Lung Transplants Help With End
A lung transplant can be an option for some patients with end-stage lung disease. The Lung Transplant Program at Brigham and Women’s Hospital offers single and bilateral lung transplantation for appropriate candidates with a variety of end-stage lung diseases, including:
Learn more about lung transplantation.
While Theres No Cure For Pah There Are Effective Ways To Manage The Disease
The median survival used to be 2.5 years. Now I’d say most patients are living seven to 10 years, and some are living as long as 20 years.
Alessandro Maresta. M.D., Vice President and Head of Global Medical Affairs, Actelion PharmaceuticalsShare
On a physiological level, there are several different biological mechanismsknown as pathwaysrelated to how blood vessels work that are believed to play a role in PAH.
“The guidelines strongly recommend that when a patient is diagnosed with PAH, they start a combination of drugs to target two different pathways,” Maresta says. “You might get one drug first, and then start on the second one within six months.” Maresta adds that current studies are now suggesting that targeting three pathways at once has the potential to lead to better outcomes.
While there’s currently no cure for PAH, the typical prognosis is much better today than it was 25 years ago. “The median survival used to be 2.5 years,” Maresta says. “Now I’d say most patients are living seven to 10 years, and some are living as long as 20 years.”
The main focus today, adds Maresta, is to find a new pathway and an effective drug to target itfor which research is currently underway. “We’re dedicated to making it happen,” Maresta says.
Read Also: What Is Stroke Level Blood Pressure
Overall Characteristics Of The Study Population
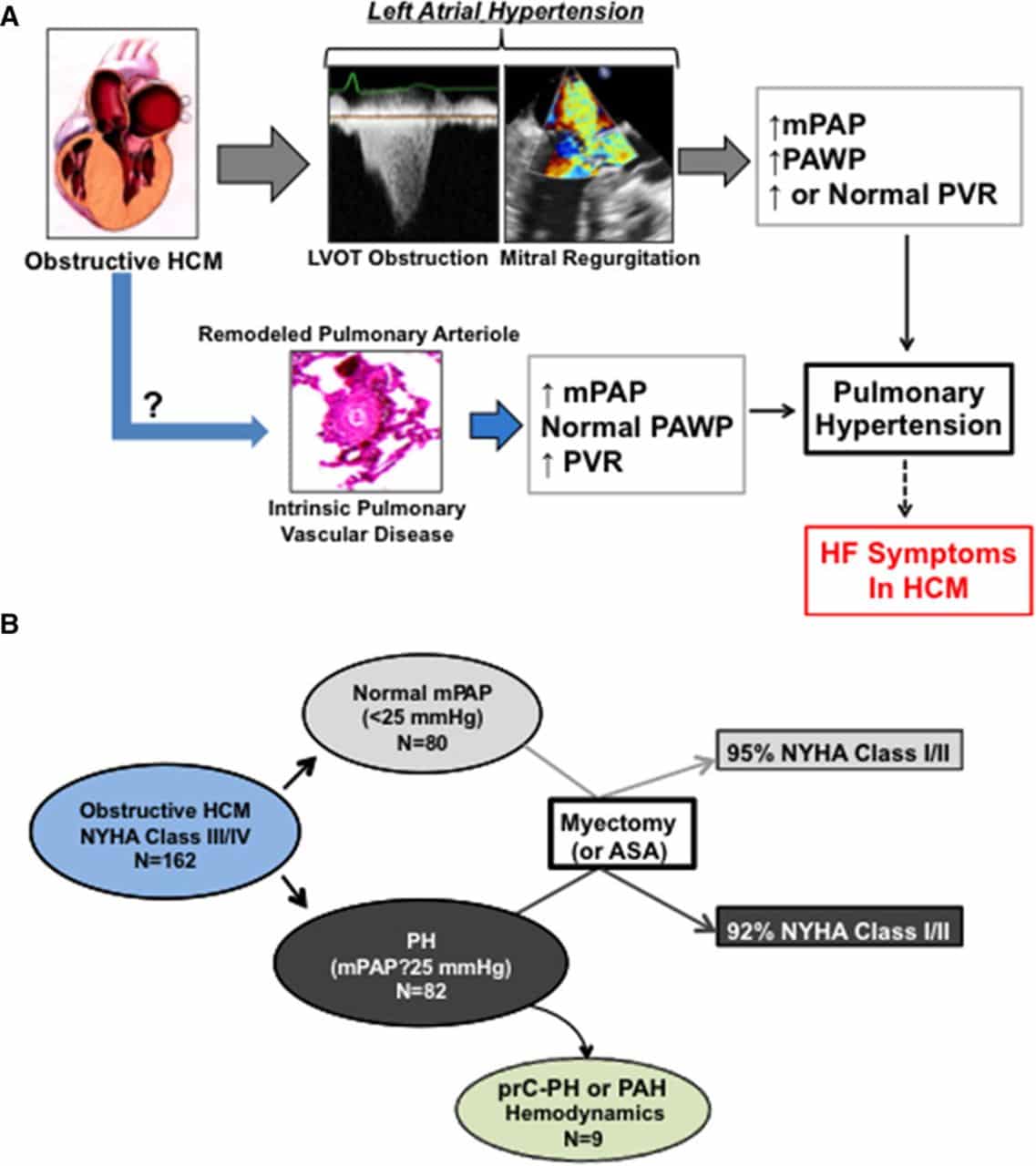
Between June 2008 and May 2012, a total of 132 patients with PH died and were reviewed by the PH team. We excluded five patients that had undergone lung transplantation and 43 subjects with nongroup I PH . The remaining 84 patients with PAH were included in this study. Mean age ± SD at the time of death was 58 ± 14 years and 61 were female. NYHA functional class at the time of last clinic visit was either III or IV in 77 patients and most of them had physical findings suggestive of right heart failure. Twenty-nine of them were on oxygen at an average ± SD flow of 4 ± 2 L/min. Right ventricular function was either moderately or severely impaired in 71 patients and 24 subjects had at least mild pericardial effusion .
Patient inclusion flow chart. PH = pulmonary hypertension.
Risk Factors For Pulmonary Hypertension
Risk factors for pulmonary hypertension include:
- family history of pulmonary hypertension especially a first-degree relative such as a parent, sibling or children
- connective tissue disorders or autoimmune diseases, including scleroderma, lupus, and rheumatoid arthritis
- living at high altitudes for extended periods of time
- chronic liver disease
- infectious diseases including human immunodeficiency virus , hepatitis B and hepatitis C
- use of certain drugs and medications including methamphetamines, chemotherapy, and some diet drugs or appetite suppressants.
Recommended Reading: What Is The Treatment For Pulmonary Hypertension
What Is Primary Pulmonary Hypertension
Primary pulmonary hypertension is high blood pressure in the lungs. Its a rare lung disorder in which the blood vessels in the lungs narrow and the pressure in the pulmonary artery rises far above normal levels. The pulmonary arteries carry blood from your body to the lungs where carbon dioxide is traded for oxygen.
Pulmonary hypertension is a serious, chronic disease that can lead to heart failure if its not treated.
Survival Rates And Prognosis
Theres currently no readily available cure for PH. Its a progressive disease, which means it can advance over time, sometimes much faster for some people than others. If left untreated, the disease can become life-threatening within a couple of years.
However, the disease can be managed. Some people can effectively make lifestyle changes and monitor their health. But for many people, PH can lead to significant heart failure, and their overall health can be in great danger. Medications and lifestyle modifications are intended to slow the progression of the disease.
If you have PH and systemic scleroderma, an autoimmune skin disease that also affects the small arteries and internal organs, your two-year survival odds are estimated to be 40 percent, according to a 2008 study. Survival rates with PH depend on the cause of the condition.
Also Check: How Do You Make Your Blood Pressure Go Down
Plausible Causes Of Arrhythmia
The mechanisms of sudden cardiac death associated with RV hypertension and arrhythmias are less well understood than are those associated with left ventricular disease. Arrhythmogenic substrate in rat hearts with monocrotaline-induced pulmonary hypertension may cause steeper RV electrical restitution and rate-dependent RV-LV action potential duration-dispersion, inducing ventricular tachycardia and fibrillation. A study of 201 pulmonary hypertension patients demonstrated that mean heart-rate corrected QT interval and QTc dispersion were significantly increased in severely ill patients, compared to patients with mild to moderate pulmonary hypertension. In addition, in women these indices were positively correlated to mean pulmonary arterial pressure, identifying a possible substrate for ventricular arrhythmias.
In contrast, supraventricular tachyarrhythmias are quite frequent. In a study of 231 PAH patients followed up for 6 years, supraventricular arrhythmias were reported with an annual incidence of 2.8%, whereas the incidence of atrial flutter and of fibrillation were almost equal, leading to rapid clinical deterioration. Atrial flutter, originating from the right atrium, seems to occur more often in patients with severely impaired hemodynamics, but does not seem to be the substrate for sudden cardiac death.
How Can I Prevent Pulmonary Hypertension
Its not always possible to prevent pulmonary hypertension. Some risk factors are out of your control. If you have risk factors, your provider may recommend preventive screenings to check your heart and lung function.
Doing whatever you can to prevent or manage other medical conditions can help lower your risk of pulmonary hypertension. Steps you can take include:
- Create an exercise plan. Ask your provider what exercises are safe for you.
- Follow a heart-healthy diet. Avoid processed foods, fast food and other foods high in salt and saturated fat.
- Quit smoking and stop using tobacco. Smoking and tobacco use are top risk factors for heart and lung problems. Quitting isnt easy, especially if youve been smoking or using tobacco for a long time. But your provider can help provide resources. Support groups may also help.
- Take medications for blood pressure and other conditions as prescribed.
Also Check: Can Apple Watch Do Blood Pressure
Investigation Into Pulmonary Hypertension
The series of tests required to confirm a diagnosis of pulmonary hypertension can be quite extensive. Your first appointment with your specialist might just be spent organising these tests, which may include:
If your doctor asks you to have any tests before the appointment, please do so because it will speed up the process of determining what the nature of your pulmonary hypertension may be, and how to treat it.
Classification Of Pulmonary Hypertension
There are many different reasons a person may develop pulmonary hypertension. The World Health Organisation classifies pulmonary hypertension by these underlying causes. These classifications include:-Group 1: Pulmonary hypertension from genetic or unknown causes, drug-induced, or related to connective tissue diseases-Group 2: Pulmonary hypertension from failure of the left side of the heart-Group 3: Pulmonary hypertension from lung diseases and chronic low levels of oxygen-Group 4: Pulmonary hypertension from chronic blood clots on the lungs-Group 5: Pulmonary hypertension from mixed or miscellaneous causes.
Pulmonary hypertension is also classified by its severity and the impact it has on a persons activities. These classifications include:
–Functional Class I: symptoms do not limit the persons physical ability-Functional Class II: symptoms result in slight limitation of physical ability, but the person is comfortable at rest. Ordinary physical activity may cause shortness of breath-Functional Class III: symptoms result in marked disability, with less than ordinary physical activity bringing on breathlessness. Comfortable at rest-Functional Class IV: symptoms at rest. Severely limited by shortness of breath.
Don’t Miss: What Do The Numbers Mean On Blood Pressure
How Common Is Pulmonary Hypertension
Some types of PH are rare, such as pulmonary arterial hypertension and PH caused by blood clots. But other types are much more common, especially PH caused by heart or lung problems.
We dont know exactly how many people around the world have pulmonary hypertension. But some estimates show PH may affect 1 in 100 people. This means 50 million to 70 million people are living with PH.
PH is even more common among older adults. Around the world, about 1 in 10 adults over age 65 have PH.
Researchers believe the number of people diagnosed with PH will rise in the next few decades.
Research Into Pulmonary Hypertension
Pulmonary hypertension is an area of intense research, particularly with respect to:
- the correct type of medication to use in the different groups of pulmonary hypertension, and in which combinations
- management of right heart failure, and possible new treatment targets or therapies
- treatments at the molecular level, such as monoclonal antibodies, which may be useful tools to slow disease progression
- further genetic markers that may identify people at high-risk of developing pulmonary hypertension.
You May Like: How To Sleep With High Blood Pressure
Talk With Others Who Understand
On myPHteam, the social network for people with pulmonary hypertension and their loved ones, more than 46,000 members come together to ask questions, give advice, and share their stories with others who understand life with pulmonary hypertension.
Are you living with end-stage pulmonary hypertension? Share your experience in the comments below, or start a conversation by posting on your Activities page.
Death And Dealing With Bereavement
When the person you care for dies, you will probably feel a range of emotions. You may feel a great sense of loss when they pass away.
As well as coping with the loss of the person you cared for, you might need to cope with the loss of your caring role.
It might be when the practical arrangements have been made and the funeral has passed that you start to grieve. However, some people experience strong feelings such as loss, grief and mourning before the person has died.
At this time, and throughout your time as a carer, it is important you take time for yourself and seek the help you need.
You may want to share your feelings with family and friends but, equally, you may not feel comfortable doing this. Some people find it easy to talk to a particular person dont be afraid to let them know how you feel. We have more information about grieving and life after the death of a loved one you might find useful to read.
Read Also: Can Constipation Cause Low Blood Pressure
When To See A Doctor/go To The Hospital
If you get short of breath once in a while or have symptoms that come and go, you should schedule an appointment with your primary care provider. Dietary and lifestyle changes can help improve your general health and prevent cardiovascular problems like pulmonary hypertension.
If you are already being treated for pulmonary hypertension, you doctor will also teach you how to watch for progression of the disease. Call the doctor who is managing your condition if you have:
- Weight gain of more than 5 pounds in a single week
- Increased swelling in your abdomen, arms, or legs
- Worsening shortness of breath, especially at rest
- Worsening cough
- Loss of consciousness
What Are The Symptoms Of Pulmonary Arterial Hypertension
You may not feel any symptoms early on. Most people with PAH begin to notice symptoms as the condition progresses. These symptoms can include:
- Blue fingers or lips.
- Shortness of breath that gets worse over time.
- Swelling in your feet and legs, later progressing to your belly and neck.
Without treatment, PAH symptoms continue to get worse over time. You may find it harder to do your usual activities without needing to catch your breath or rest.
Don’t Miss: What Can Increase Blood Pressure
How Can You Manage Symptoms Of End
You can help manage the symptoms of end-stage lung disease by:
- Quitting smoking and all tobacco products
- Avoiding any known irritants that may cause lung inflammation
- Getting an annual flu and pneumonia vaccine
- Preparing for emergencies and periods of exacerbations
- Meeting with your healthcare team frequently to monitor your health
- Receiving emotional support through therapy or support groups
- End-of-Life Care for End-Stage Lung Disease
It is important to discuss your end-of-life wishes with your healthcare team and family. Your plan may include palliative and hospice care to help manage severe symptoms.
The Palliative Care team at the Brigham includes physicians, nurse practitioners, social workers, clergy members and a personal case manager to manage pain and other symptoms, as well as promote open communication about care.
What Is The Treatment For Pulmonary Arterial Hypertension
Treatment for PAH focuses on slowing down its progression and giving you a better quality of life. Theres no one-size-fits-all approach to PAH treatment. Your provider will work with you to decide the best treatment for your specific needs.
Your individualized treatment plan for PAH may include:
- Balloon atrial . This procedure typically treats babies with congenital heart defects, but its also sometimes used for adults with PAH. A septostomy helps take pressure off the right side of your heart and also allows more oxygen to circulate in your blood. It may serve as a bridge to a lung transplant.
- Calcium channel blockers. These medications help lower the blood pressure in your pulmonary arteries and throughout your body.
- Diuretics. These water pills get rid of extra fluid in your body and reduce swelling.
- Oxygen therapy. You may need this treatment if you dont have enough oxygen in your blood. Supplemental oxygen can help people during rest, sleep or exercise.
- Pulmonary vasodilators. These medications help your pulmonary arteries relax and open up better. This relieves the strain on your heart and helps ease your symptoms.
A last resort option for some people with severe PAH is a lung transplant. This surgery may give you one or two new lungs. A heart-lung transplant gives you a new heart as well.
You May Like: How To Know If You Have High Blood Pressure
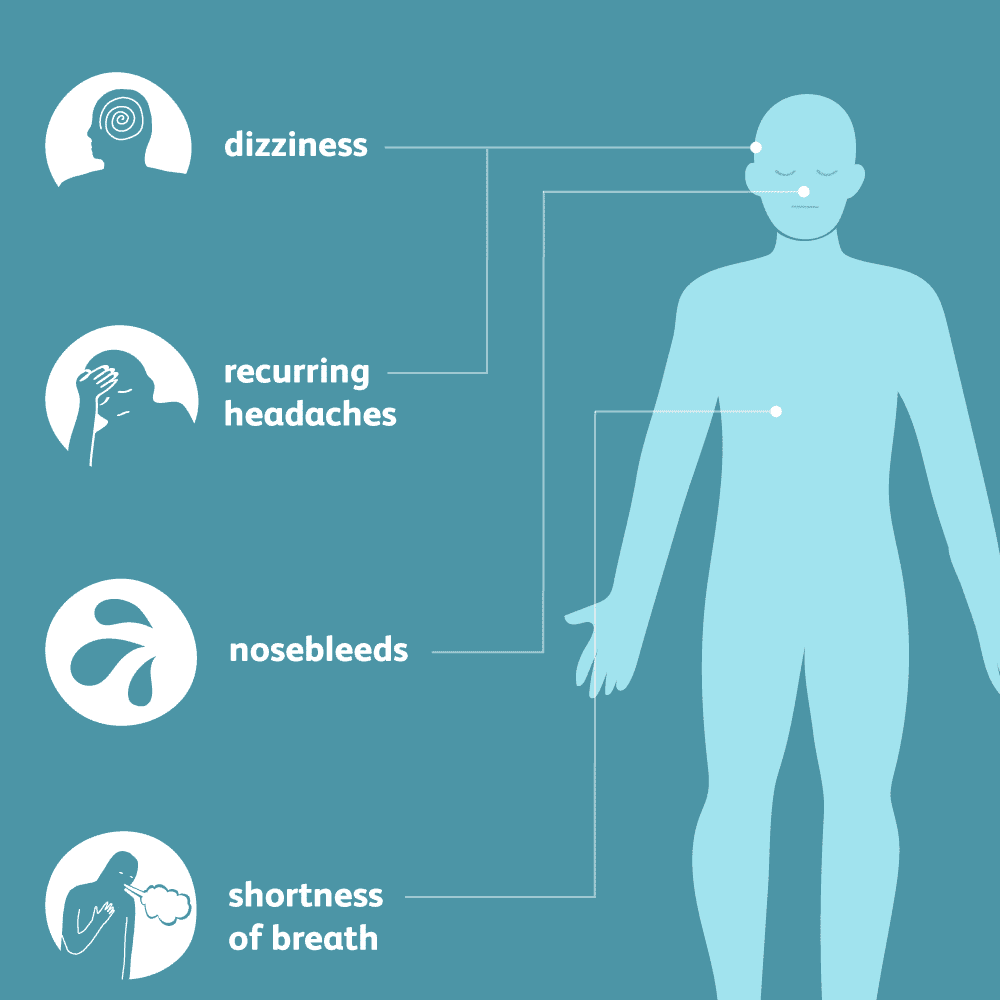
Symptoms Of Pulmonary Hypertension
- a racing heartbeat
- swelling in the legs, ankles, feet or tummy
The symptoms often get worse during exercise, which can limit your ability to take part in physical activities.
If you have a type of pulmonary hypertension known as pulmonary arterial hypertension , you may not have any symptoms until the condition is quite advanced.
Pah Affects Women More Than Men
The idiopathic and heritable forms of PAH are at least twice as common in women compared to men, according to the Pulmonary Hypertension Association. In fact, PAH is most often diagnosed in women between the ages of 30 and 60.
It’s not currently known why females are more susceptible, but some theories under investigation have to do with the role of estrogen, changes that occur during pregnancy and links to autoimmune issues, which also tend to be more prevalent in women.
Also Check: Can You Take Your Own Blood Pressure
Why: Communicating And Prognosticating In Ph With Uncertainty
Communication with patients who have PAH requires preparation and a knowledge base of the underlying disease process, disease trajectory, and prognosis. These communications may arise from the primary PAH treatment team or may come from different parts of the multidisciplinary team depending on comfort level and expertise. Collaboration with PC may be initiated with an intensive up-front assessment at the time of diagnosis, with long-term follow-up on an as-needed basis when symptoms or side effects occur, or may be initiated only when symptoms/side effects begin to outweigh the derived benefit from PH-directed therapies. How do we measure successful or beneficial PC interventions? Quality metrics in palliative medicine may be best measured by QOL rather than length of survival as a surrogate marker. The ultimate goal of PC is a patient-centered focus with a plan that aligns with the patient’s value system and provides a supportive structure to uphold those values and improve QOL. Despite historical obstacles, implementation of PC may improve QOL and provide a respite from symptoms and medication side effects while neither hastening nor postponing death.