Development And Diagnosis Of Pulmonary Hypertension And Sleep Apnea
Sleep apnea is known to contribute to the development of cardiovascular disease and pulmonary hypertension. It happens because the disease increases the risk of hypertension, pulmonary vascular disease, ischemic heart disease, stroke, congestive heart failure and arrhythmias. A study, Obstructive sleep apnea and pulmonary hypertension, concluded that the increase in pulmonary artery pressure is related to repetitive nocturnal arterial oxygen desaturation and hypercapnia, in addition to large intrathoracic negative pressure swings.
Because the disease causes the effects repeatedly, it results in pulmonary vascular remodeling, sustained pulmonary hypertension and right ventricular hypertrophy, as demonstrated in rodent tests. Both conditions share a series of risk factors that include age, gender, obesity, diabetes and hypertension. However, the American College of Chest Physicians does not consider screening for pulmonary hypertension needed for patients with sleep apnea unless there are suspicions, which can delay diagnosis and treatment, as well as accelerate the development of more severe consequences.
Prevalence Of Pah In Sleep Apnea
Respiration.Cor Vasa.Thorax.Chest.Chest.Eur Respir J.Am J Respir Crit Care Med.Klin Wochenschr.Am J Respir Crit Care Med.Arch Intern Med.Am Rev Respir Dis.Psychiatr Clin Neurosci.Respiration.Cor Vasa.Thorax.Chest.Chest.Eur Respir J.Am J Respir Crit Care Med.Am J Respir Crit Care Med.Arch Intern Med.Am Rev Respir Dis.Klin Wochenschr.Psychiatr Clin Neurosci.
Respiration.Thorax.Chest.Am J Respir Crit Care Med.Respiration.Cor Vasa.Chest.Chest.Eur Respir J.Arch Intern Med.Am Rev Respir Dis.Psychiatr Clin Neurosci.Chest.Chest.Cor Vasa.Chest.Chest.Eur Respir J.Am J Respir Crit Care Med.Am Rev Respir Dis.Thorax.Arch Intern Med.Thorax.
Arch Intern Med.Am J Respir Crit Care Med.Am J Respir Crit Care Med.Arch Intern Med.
Curr Opin Pulm Med.Am J Respir Crit Care Med.J Appl Physiol.
- Lavie P
- Lavie L
Am J Respir Crit Care Med.
- Chan L-Y
- et al.
Am J Respir Crit Care Med.
What Is Sleep Apnea
Apnea is a temporary cessation of breathing, especially during sleep. Based on the definition, referring to the condition as sleep apnea may seem redundant. But because apneas can occur at other times, it is an important distinction to make.
With sleep apnea, breathing stops and starts at least 5 times an hour, but can pause as many as several hundred times a night. These pauses can last anywhere from 5 seconds to several minutes at a time. When this happens, blood oxygen levels drop and trigger you to wake up. Frequent sleep disruptions causes a variety of side effects. These side effects may include:
- Irritability
- Driving accidents
- Depression
There are a few types of sleep apnea but the most common type is Obstructive Sleep Apnea . With OSA these apnea events occur when the airway becomes partially or completely blocked during sleep. The blockage may be due to several different factors.
Common causes of Obstructive Sleep Apnea are:
- Relaxation of the neck and throat muscles, causing the soft palate to collapse
- Tongue balling up in the back of the throat
- Fatty deposits in the tongue or neck restrict the airway
- Narrow airway
With OSA the brain continues sending messages to the body to breathe. The muscles of the chest and diaphragm work even harder to breathe but are not able to completely clear the blockage. This results in the loud snoring, choking, or gasping during sleep that is common for people with the condition.
Don’t Miss: Do Onions Lower Blood Pressure
What Is The Relationship Between Sleep Apnea And Blood Pressure
Of the two types of sleep apnea, only OSA is linked to high blood pressure. CSA isnt a known cause of hypertension, but it develops in 30 to 50% of people with heart failure.
The prevalence of OSA is estimated to be between 4 and 7% of the general population, but it affects 30 to 40% of people with hypertension. Of people diagnosed with OSA, it is estimated that around half also have high blood pressure.
In healthy individuals, blood pressure naturally lowers by between 10 and 20% at night, a phenomenon that is sometimes referred to as blood pressure dipping. People with severe OSA experience blood pressure dips of less than 10%, which indicates a nondipping blood pressure pattern.
People who have nondipping blood pressure at night face an increased risk for cardiovascular issues. Additionally, many patients with OSA experience a sudden and pronounced elevation of their blood pressure when they wake up in the morning. This morning surge is another factor that may increase risk for cardiovascular disease. Moderate to severe OSA increases all-cause and cardiovascular mortality.
OSA doesnt only affect blood pressure at night. Studies show that daytime blood pressure levels also increase with sleep apnea severity.
Should I Talk To My Doctor About Sleep Apnea
If you have high blood pressure and are concerned about whether you might also have sleep apnea, speak with a doctor. Diagnosis is the first step to accessing effective treatments for OSA that may improve your sleep and blood pressure. Consider whether any of the following symptoms apply to you:
- Daytime sleepiness
- Difficulty with attention and memory
- Headaches in the morning
- Dry mouth when waking up
- Irritability, anxiety, or depression
Sleep apnea is often not recognized by the affected individual. In many cases, a bed partner notices nighttime symptoms of OSA, which prompts a visit to the doctor. If you share a bedroom or home with someone else, ask if they have noticed you exhibiting any of these signs while you are sleeping:
- Loud snoring
- Choking or gasping during sleep
- Pauses in breathing during sleep
Experiencing one or more of these symptoms does not necessarily mean you have sleep apnea, but it is a good reason to bring up sleep with your doctor.
- Was this article helpful?
You May Like: Vodka Blood Pressure
How Does Sleep Apnea Cause High Blood Pressure
Related Reading
Each time a person with OSA experiences airway collapse and briefly stops breathing during sleep, their sympathetic nervous system becomes activated and blood pressure rapidly spikes when they resume breathing. Sometimes, this sequence of pausing and resuming breathing can cause a person to wake from sleep. When a person wakes up after an OSA event, activation of the sympathetic nervous system and blood pressure levels escalate to an even greater degree.
Additionally, when sleep is disrupted by OSA symptoms, the body releases sympathetic nervous system hormones called catecholamines into the blood. Catecholamines are stress hormones that are majorly released by the adrenal glands. Examples of catecholamines include dopamine and epinephrine . High levels of catecholamines in the blood cause high blood pressure.
Sleep Apnea And Cardiovascular Conditions
For many people, Sleep Apnea and Cardiovascular Conditions go hand-in-hand and often occur at the same time, but its unclear if Sleep Apnea directly causes heart conditions. It can refer to a number of conditions, including:
- Heart Attack
- High Blood Pressure
Heart failure has also been linked to a less common form of Sleep Apnea.
Known as Central Sleep Apnea, its a condition in which the signal to breathe isnt sent to the lungs by the brain. Central Sleep Apnea impacts people with congestive heart failure and Cheyne-Stokes Breathing4.
This is a form of shallow breathing that gradually decreases during sleep, and eventually can cause it to stop completely. The stoppage of breathing is known as Central Sleep Apnea4. Central Sleep Apnea is treated differently from the most common form of Sleep Apnea: Obstructive Sleep Apnea.
Obstructive Sleep Apnea is the most common form of Sleep Apnea and its also the easiest to treat. Obstructive Sleep Apnea is a condition in which a persons airway becomes blocked by the soft tissues of the mouth and throat during sleep, preventing air from reaching the lungs. Obstructive Sleep Apnea affects over 22 million Americans, and many of them dont know that they have it5.
- High BMI
- Tobacco Use
- Alcohol Consumption
Reducing risk factors for one condition usually has a side effect of improving the symptoms of the other and vice-versa. Thats why its important to take steps to reduce these risk factors as a part of your Sleep Apnea treatment.
Read Also: Does Spicy Food Cause High Blood Pressure
What Treatments Are Available
CPAP has been shown to be effective in patients with heart failure. Controlled trials have shown that treatment of OSA with CPAP is associated with significant improvements in cardiac function, sympathetic activity and quality of life. In the Canadian Positive Airway Pressure study, CPAP improved nocturnal oxygenation, increased left ventricular function, lowered norepinephrine levels and improved functional capacity among patients with sleep apnea and heart failure. Several recent studies have shown reductions in pulmonary artery pressure in patients with OSA after nocturnal CPAP treatment.
Answer provided by David Pham, MD, FCCP, Pulmonary Hypertension Specialist, Pulmonary & Critical Care, Lung Care Center, Fountain Valley, Calif.
How Sleep Apnea Affects Blood Pressure
High blood pressure, also called hypertension, is a common health issue in which the amount of force that pumps blood through blood vessels is higher than normal. People with hypertension often dont have symptoms but learn they have high blood pressure during routine checks at a doctors office. If left untreated, high blood pressure puts a daily strain on the cardiovascular system which may lead to stroke, heart disease, and other conditions. Fortunately, managing hypertension with medication and lifestyle changes can reduce your risk for harmful health effects.
Sleep apnea is a sleep disorder that causes numerous lapses in breathing during sleep. There are two types of sleep apnea: obstructive sleep apnea and central sleep apnea . OSA is marked by episodes of airway collapse, which blocks airflow into the lungs and often causes snoring and gasping during sleep. In CSA, breathing lapses occur because of a lack of communication between the brain and the muscles involved in breathing.
Its important to understand the relationship between hypertension and sleep apnea because these two conditions affect one another, and treatment for sleep apnea can lower blood pressure in people who have both.
Recommended Reading: Does Spicy Food Cause High Blood Pressure
Does Sleep Apnea Cause High Blood Pressure
Sleep Apnea plays a very important role in causing high blood pressure, but it is not the only cause1. High blood pressure has been linked to many things, including:
- Diet
- Caffeine Intake
- Sleep Conditions
Improving any one of these risk factors can lower your blood pressure. Studies have also found that in instances where a persons blood pressure is being treated but is not fully regulated, Sleep Apnea treatment can help.
Typically, Sleep Apnea treatment involves using Continuous Positive Airway Pressure therapy through either a CPAP machine, APAP machine, or BiPAP machine to blow pressurized air into the airway, causing the relaxed muscles of the airway and throat to open up.
This, in turn, allows air to reach the lungs. Provided you use your therapy equipment regularly, it can help raise blood oxygen during sleep. As blood oxygen saturation goes up, blood pressure goes down.
Sleep Apnea can also indirectly influence blood pressure. If youre not sleeping, you may go through your day tired. In these situations, you may consume more caffeine to help stay awake. Increased caffeine consumption can lead to higher blood pressure readings. If Sleep Apnea is adequately treated, you may need less caffeine to stay awake.
Osa And Heart Failure
Given the strong etiological relationship between OSA, on one hand, and CAD , hypertension and arrhythmia on the other, it is not surprising that OSA is also an independent risk factor for heart failure . The prevalence of OSA in heart failure patients is far higher than in the general middle-aged population .
Patients with OSA have high prevalence of hypertension creating difficulty in making strong conclusions about a direct relation between OSA and left ventricular abnormality independent of hypertension . However, several studies have suggested a causative relation between OSA and left ventricular remodeling, probably via intermittent hypoxia-induced oxidative stress . A large portion of patients with OSA have either systolic dysfunction or subclinical echocardiographic left ventricular abnormalities . In an important study of children with OSA who are free of cardiovascular disease , Amin et al. found evidence of asymptomatic early left ventricular remodeling in these children.
Chronic cardiovascular consequences of OSA LV = left ventricle, RV = right ventricle, SVR = systemic vascular resistance, = increased
Read Also: Do Onions Lower Blood Pressure
Why Do The Pulmonary Arteries Narrow
Scientists believe that the process starts with injury to the layer of cells that line the small blood vessels of the lungs. This injury, which occurs for unknown reasons, may cause changes in the way these cells interact with the smooth muscle cells in the vessel wall. As a result, the smooth muscle contracts and grows more than is normal and narrows the vessel.
Narrative Review Of Sleep And Pulmonary Hypertension
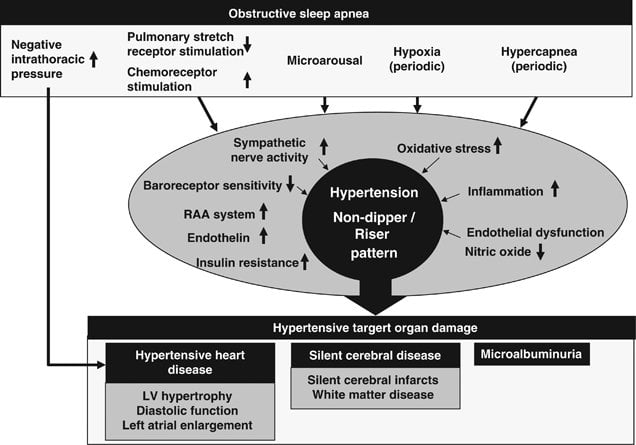
Bacon Jenny Louise1, Fleming Carys1, Marino Philip2
1Surrey and Sussex Healthcare NHS Trust, Redhill Guys and St Thomas NHS Foundation Trust , , UK
Contributions: Conception and design: None Administrative support: F Carys Provision of study materials or patients: None Collection and assembly of data: BJ Louise Data analysis and interpretation: BJ Louise, M Philip Manuscript writing: All authors Final approval of manuscript: All authors.
Correspondence to:
Keywords: Pulmonary hypertension pulmonary heart disease sleep apnoea syndromes sleep apnoea obstructive hypoventilation
Submitted May 30, 2020. Accepted for publication Aug 17, 2020.
doi: 10.21037/jtd-cus-2020-004
Also Check: Is High Blood Pressure Heart Disease
Sdb In Patients With Precapillary Ph
So far, the direct or indirect effects of SDB on precapillary PH had been discussed. There is evidence that the relation may also act in the opposite direction, so that precapillary PH may trigger SDB . As many features of patients with left ventricular failure and SDB, such as low cardiac output, increased sympathetic tone, and arrhythmia, are also common in patients with precapillary PH and right ventricular failure, some authors have also looked at SDB in patients with precapillary PH of different origins. These studies are summarized in Table 2.
Table 2
Sleep-disordered breathing among patients with precapillary pulmonary hypertension
Fig. 4
Apnea/hypopnea index in 38 patients with precapillary pulmonary hypertension. The bars are ordered in descending order of the total apnea/hypopnea index with the black part representing the obstructive and the gray part the central events. A value of 10 was observed in 45% of patients, the median value was 8/h .
Can Sleep Apnea Cause Lung Problems
Research published in BMC Pulmonary Medicine found that patients with OSA had increased lung elasticity recoil pressure. The elastic quality of lung tissues is what allows them to expand and contract when you breathe. With increased lung elasticity recoil pressure the lungs snap back too forcefully. This creates a vacuum effect that contributes to airway collapse in OSA. The resulting reduction in lung volume increases the risk or worsens the symptoms of some very serious lung problems.
Lung problems that are common in patients with sleep apnea include:
- Chronic Obstructive Pulmonary Disease
- Pulmonary Hypertension
- Asthma
You May Like: Do Onions Lower Blood Pressure
Qualifying For Disability For Sleep Apnea
SSA The Social Security Administration doesnt provide a listing for disability concerning sleep apnea. SSA disability listing does cover other breathing disorders, mental defects, and heart diseases in disability listing.
Having diseases that are listed in the SSA disability list can make you eligible to receive benefits against your disability. If you can qualify by meeting the required criteria of the disability listing due to sleep apnea, you can receive benefits.
To meet the criteria, you need to prove that your ailment is causing hindrance in major life activities. You can meet the listing for certain complications like severe mood disturbance, cognitive defects, behavioral issues, chronic heart failure symptoms, or chronic pulmonary hypertension.
Social Security Listing 3.09 states that pulmonary hypertension qualifies automatically for the disability benefits if the pressure on the pulmonary veins is greater than 40 mm Hg.
Listing 4.0 shows lengthy criteria if you want to list sleep apnea based on heart diseases. For mental disorder benefits list 12.02 discusses even strict criteria for disability benefits. To qualify, under the listing a person must suffer an intellectual mental disorder, depression, memory issues, or anxiety. Other than these, you must prove that you either have:
Osa Is A Cause Of Hypertension
Hypertension, the most prevalent cardiovascular disease, is also the best established cardiovascular consequence of obstructive sleep apnea . Hypertension affects approximately 30% of adults in the United States with an impact on public health that cannot be overstated. The World Health Organization estimates that even suboptimal blood pressure levels are responsible for 62% of cerebrovascular disease and 49% of ischemic heart disease . On the other hand, OSA affects between 9% and 25% of middle-aged adults . OSA is estimated to be present in 3040% of patients with hypertension, while 40% of patients with OSA are thought to have hypertension . Since both disorders are very prevalent in middle-aged individuals, and coexist in a large portion of the population it had been difficult to elucidate the causeeffect relationship between the two disorders. However, in recent years, mounting evidence from large epidemiological studies, along with human and animal experiments, was able to confirm the presence of this causal relationship between OSA and hypertension. The mechanism of hypertension in patients with OSA remains only partially understood so far. In this article, we will focus on the clinical and epidemiological evidence for the causative relationship between OSA and hypertension. The basic mechanisms of the association between OSA and hypertension were reviewed in the first part of this series.
You May Like: Do Onions Lower Blood Pressure
Osa And Precapillary Ph
Patients with OSA may show acute or chronic hemodynamic changes associated with intermittent hypoxemia. Various pathophysiologic mechanisms have been discussed. Comorbid conditions additionally play an important role.
Sympathetic Overstimulation. In patients with OSA, breathing efforts against an occluded airway cause large fluctuations in systemic blood pressure associated with hypoxemia, arousals and surges of sympathetic tone . Moreover, major rises in both systemic and PAP during long apneas in phasic REM sleep have been described . The large arterial pressure swings associated with sympathetic overstimulation in OSA patients induce vascular shear stress and promote endothelial dysfunction . Repetitive hypoxia and reoxygenation may upregulate hypoxia-inducible factors, vascular endothelial growth factor and erythropoietin, and trigger inflammatory processes . These mechanisms may lead to elevations in PAP that persist even during daytime and over prolonged time as suggested for the pathophysiology of systemic hypertension in OSA.
Fig. 2
Example of polysomnographic recording during phasic and tonic rapid eye movement sleep. There are major rises in both systemic and pulmonary artery pressure during apneas in phasic REM sleep . Abdo., abdomen HR, heart rate PAP, pulmonary artery pressure Psa, systemic arterial pressure.