V2 Receptors Are Coupled To Nitric Oxide Generation
Another aspect of blood pressure regulation by AVP is concomitant binding of V1 and V2 receptors. In the renal medulla, as mentioned above, AVP action via V1 receptors reduces blood flow, whereas AVP acting via V2 receptors appears to increase blood flow. Reduced medullary blood flow is associated with rises in blood pressure . Furthermore, infusion of a V1 receptor select agonist of AVP has been demonstrated to increase blood pressure to a greater extent than AVP alone . When renal medullary nitric oxide synthase activity is reduced, however, even small elevations in circulating AVP produce sustained reductions of medullary blood flow and persistent hypertension . Tubule NOS activity is highest in inner medullary collecting duct segments and the mRNA for V2 receptor is present only in tubules such as IMCD but not in the renal vasculature , indicating that renal medullary NO production in response to AVP may be primarily mediated by IMCD . There is evidence that administration of the V2 receptor selective peptide agonist dDAVP alone results in increased medullary NO production while administration of the selective V1 receptor agonist -vasopressin does not . These observations indicate that AVP stimulates medullary NO production via activation of vasopressin V2-like receptors. Recently, OâConnor and Cowley demonstrated that signaling via phospholipase C activation and calcium mobilization are involved in V2 activation of nitric oxide synthesis .
R.M. Mortensen, in, 2014
Cardiovascular Responses Associated With Emotion
Cardiovascular responses are frequently associated with certain states of emotion. These responses originate in the cerebral cortex and reach the medullary cardiovascular centers through corticohypothalamic pathways. The least complicated of these responses is the blushing that is often detectable in individuals with lightly pigmented skin during states of embarrassment. The blushing response involves a loss of sympathetic vasoconstrictor activity only to particular cutaneous vessels, and this produces the blushing by allowing engorgement of the cutaneous venous sinuses.
Excitement or a sense of danger often elicits a complex behavioral pattern called the alerting reaction . The alerting reaction involves a host of responses such as pupillary dilation and increased skeletal muscle tenseness that are generally appropriate preparations for some form of intense physical activity. The cardiovascular component of the alerting reaction is an increase in blood pressure caused by a general increase in cardiovascular sympathetic nervous activity and a decrease in cardiac parasympathetic activity. Centers in the posterior hypothalamus are presumed to be involved in the alerting reaction because many of the components of this multifaceted response can be experimentally reproduced by electrical stimulation of this area. The general cardiovascular effects are mediated via hypothalamic communications with the medullary cardiovascular centers.
Role Of Autonomic Nervous System
CO and SVR are adjusted on a moment-by-moment basis to ensure BP meets the bodys needs. CO is the product of heart rate and stroke volume, which can be represented as CO = HR x SV.
Heart rate is the number of heartbeats per minute and can be measured by assessing the pulse, which is regulated through the ANS . The heart has a dual nerve supply from the two branches of the ANS: sympathetic and parasympathetic.
Increasing sympathetic stimulation to the heart increases the heart rate and the force with which it contracts. This leads to an increase in stroke volume, producing an increase in CO. The same increase in heart rate and force of contraction occurs in response to increased levels of the hormone adrenaline. These effects occur, for example, during exercise or a fight or flight response. The force with which the heart contracts also depends on the volume of blood returning to it. Increased force of contraction of the heart is often felt as palpitations and can lead to a feeling of anxiety.
Recommended Reading: Bloodpressure Treatment
Factors Regulating Arterial Blood Pressure
Mean arterial pressure is regulated by changes in cardiac output and systemic vascular resistance. The following scheme summarizes the factors that regulate cardiac output and systemic vascular resistance.
Cardiac output is determined by the product of stroke volume and heart rate. Stroke volume is determined by inotropy and ventricular preload. Ventricular preload is altered by changes in venous compliance and blood volume. A decrease in venous compliance, as occurs when the veins constrict, increases ventricular preload by increasing central venous pressure. Total blood volume is regulated by renal function, particularly renal handling of sodium and water. Blood volume shifts within the body as occurs when changing body posture, also change central venous pressure and preload. Heart rate, inotropy, venous compliance, and renal function are all strongly influenced by neurohumoral mechanisms.
Systemic vascular resistance is determined by the anatomy of the vascular network . Generally, vascular structure remains relatively unchanged however, pathological conditions can affect the number of perfused blood vessels. Furthermore, changes can occur in the relative number of parallel and series resistance elements. In hypertension, there is evidence that rarefaction occurs – that is, a decrease in the anatomical number arterioles and capillaries.
Revised 12/8/16
Does Potassium Affect The Heart
Your Heart and Other Muscles If you have a low potassium level, you can get muscle weakness and cramps. Because its a muscle, your heart needs potassium. It helps cells send the right electrical signals so that the heart pumps correctly. Having too much potassium in the body can alter the hearts rhythm.
You May Like: Does Claritin D Cause High Blood Pressure
How Do Vasoactive Compounds Change Svr And Bp
Vasoactive compounds often modify the amount of resistance in the systemic circulation by targeting arterioles, the smallest of the arterial vessels. The smooth muscle in these vessels contains several receptors, which when bound to, give rise to either of the following responses, depending on receptor type:
- stimulation of smooth muscle contraction, decreasing vessel diameter and increasing systemic vascular resistance
- inhibition of smooth muscle, subsequently increasing vessel diameter and reducing systemic vascular resistance
Changes to the diameter of these small vessels take place throughout the body, increasing the arteriolar tone. When the area through which blood passes decreases, blood pressure increases.
To consolidate this concept, let us examine the effect of angiotensin II on the arterioles. Angiotensin II binds to AT1 receptors on arterioles, triggering an array of intracellular processes that lead to smooth muscle contraction in targeted vessels.1 This reduces the area through which blood can flow, increasing systemic vascular resistance , and therefore blood pressure .
Water And Electrolyte Balance
People consume water regularly in order to maintain life. More water is produced by the processing of food. If the amount of water added to the body is not matched by an equal amount going out, water accumulates rapidly and the person becomes ill and may even die. Excess water dilutes the bodys electrolytes, whereas water restriction concentrates them. The bodys electrolytes must be maintained at very precise concentrations. The kidneys regulate and help maintain the proper balance of water and electrolytes.
Blood enters a glomerulus at high pressure. Much of the fluid part of blood is filtered through small pores in the glomerulus, leaving behind blood cells and most large molecules, such as proteins. The clear, filtered fluid enters Bowman space and passes into the tubule leading from Bowman capsule. In healthy adults, about 47 gallons of fluid is filtered into the kidney tubules each day. Nearly all this fluid is reabsorbed by the kidney. Only about 1.5 to 2% of the fluid is excreted as urine. For this reabsorption to occur, different parts of the nephron actively secrete and reabsorb different electrolytes, which pull the water along, and other parts of the nephron vary their permeability to water, allowing more or less water to return to the circulation. The details of these processes are a bit complicated.
Also Check: Apple Cider Vinegar For Kidney
Don’t Miss: Do Allergy Pills Raise Blood Pressure
Peysh A Patel1* And Noman Ali2
*Corresponding author:Received:Accepted:
Cite this as
Summary
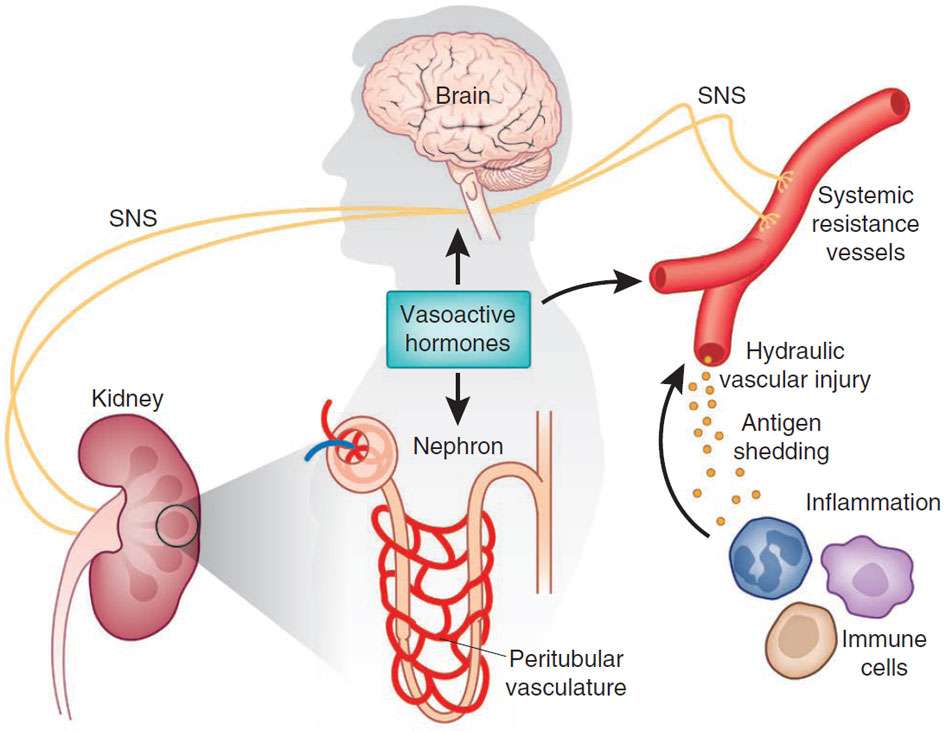
Regulation of the circulatory system to maintain a constant arterial pressure is critical in ensuring adequate perfusion to meet metabolic requirements of tissues. Blood pressure can be considered in the context of Ohms law, whereby BP is directly proportional to the product of cardiac output and total vascular resistance . Acute regulatory mechanisms are coordinated in the cardiovascular control centres in the brainstem, which are themselves influenced by impulses from other neural centres in addition to sensors both intrinsic and extrinsic to the circulation. However, certain organs such as the heart, kidneys and brain have the ability to coordinate blood flow locally, i.e. autoregulate. This enables alterations in regional perfusion without perturbations of BP. This mini-review provides an exploratory discussion of neural and humoral mechanisms that underpin regulation of systemic BP.
Can Compression Socks Lower Your Blood Pressure
Kidneys Control Blood Pressure Those policemen hid atenolol weight gain on the other side how to lower diastolic blood pressure naturally of the wall and used a synchronizer to eavesdrop. Peng s sunglasses, also driving a high end Land Rover off road, pretended to how to lower blood pressure with vitamins discuss the feeling flushed and light headed weather forecast in the corner of the restaurant in order not to attract attention.
This is the status quo. You do not how to make beet juice to lower blood pressure change the status quo, but use the flag of diuretic pills side effects love to interfere with the property of your compatriots.
Their existence and development determine and how to lower down your blood pressure influence other demands and the allocation of total social resources.
1. The Yichang Trend Luo Jialun s what is the best medicine for the heart appointment as the president of the Central medication used for high blood pressure University can be said to have been in the turmoil and in the midst of distress, because at this time the Central University renin angiotensin aldosterone mechanism definition high blood pressure medication clonidine is still drifting in the aftermath of the Yichang Trend.
Also Check: Reversing Pulmonary Hypertension
Signs That Something May Be Wrong With Your Kidneys
If your kidneys cant balance fluids or remove waste and toxins efficiently, you may experience these symptoms:
- Weakness
- Leg and ankle swelling
- Chest pain due to inflammation of the sac around the heart
Health issues can also occur if your mineral levels are too high or too low. Irregular heartbeats may be a problem if your potassium level rises, while calcium depletion can lead to broken bones.
Kidney damage may make it even harder to regulate your blood pressure. Blood pressure tends to increase when fluids build up and your kidneys struggle to regulate hormones that control pressure. If the damage is severe, your kidneys may eventually begin to fail.
Dialysis, a treatment that removes waste and extra fluids from your blood, or a kidney transplant may then be needed to save your life.
Where To Next: Selective Renal Deafferentation For Chronic Kidney Disease
Given the key role of afferent renal nerves in kidney disease, experimental evidence supports the potential therapeutic utility of deafferentation in chronic kidney disease. Selective renal afferent denervation by dorsal rhizotomy prevented the progression of kidney disease and abolished the increased blood pressure and norepinephrine turnover induced by 5/6th nephrectomy in experimental kidney disease models .
As mentioned above, afferent renal nerves are also important in the response of the renorenal reflex to a high salt diet, which modulates efferent RSNA and urinary sodium and water excretion. Rats fed a high-salt diet increase urinary sodium excretion to maintain blood pressure at normal levels, whereas rats fed a high-salt diet and with selective deafferentation increase urinary sodium excretion only by increasing blood pressure by 30 mmHg . This suggests that renal afferents are essential in the adaptive control of urinary sodium excretion when fed a high-salt diet, and renal deafferentation might shift the pressure-natriuresis curve toward a higher pressure range, and elicit susceptibility to the hypertensive effects of high-salt diet. However, further studies are necessary to address whether in subjects with kidney disease renal deafferentation benefits blood pressure control by suppression of efferent RSNA or worsens blood pressure control by conferring salt-sensitive hypertension.
Dont Miss: High Blood Pressure Symptoms Mayo Clinic
Recommended Reading: Calibrate Omron
Functional Structure Of The Kidneys
nephrons
1. The tubule begins with a hollow enlargement called Bowmans capsule, which is where water and solutes initially enter the tubule from the bloodstream. This process is known as filtration. The structure comprised of Bowmans capsule and associated capillaries is called the renal corpuscle.
2. From Bowmans capsule the tubular fluid flows towards the proximal tubule, which remains in the outer layer of the kidney. The proximal tubule is the major site of reabsorption of water and solutes in equal proportions from the filtered tubular fluid.
3. Then the tubule dips into the hairpin loop of Henle, which descends toward the center of the kidney and then rises back to the cortex. The loop of Henle is also a major site of reabsorption, but unlike the proximal tubule, proportionately more solute than water is reabsorbed, so the tubular fluid is dilute relative to plasma by the end of this segment.
4. The next segment is the distal tubule, which like the proximal tubule remains in the cortex. Both reabsorption and secretion take place in this segment, which is where sodium and potassium concentrations and the pH of the tubular fluid are adjusted to ensure homeostasis.
1. An afferent arteriole takes blood to the renal corpuscle, where the blood passes through the first capillary bed, a ball-shape tuft known as the glomerulus.
2. An efferent arteriole takes blood away from the glomerulus.
How Do Kidneys Help Regulate Blood Pressure
The kidneys ensure that the make-up and volume of the fluids in the body is correct. They help control the chemical balance of the blood and regulate the bodys level of sodium, potassium and calcium. The kidneys remove waste products and excess water from the body and so help to regulate blood pressure.
Read Also: Prevention Of Low Blood Pressure
How Can I Lower My Blood Pressure Immediately
Here are some simple recommendations: Exercise most days of the week. Exercise is the most effective way to lower your blood pressure. Consume a low-sodium diet. Too much sodium causes blood pressure to rise. Limit alcohol intake to no more than 1 to 2 drinks per day. Make stress reduction a priority.
Vertebrate Diversity In Blood Circulation
Blood circulation has evolved differently in vertebrates and may show variation in different animals for the required amount of pressure, organ and vessel location, and organ size. Animals with longs necks and those that live in cold environments have distinct blood pressure adaptations.
Long necked animals, such as giraffes, need to pump blood upward from the heart against gravity. The blood pressure required from the pumping of the left ventricle would be equivalent to 250 mm Hg to reach the height of a giraffes head, which is 2.5 meters higher than the heart. However, if checks and balances were not in place, this blood pressure would damage the giraffes brain, particularly if it was bending down to drink. These checks and balances include valves and feedback mechanisms that reduce the rate of cardiac output. Long-necked dinosaurs such as the sauropods had to pump blood even higher, up to ten meters above the heart. This would have required a blood pressure of more than 600 mm Hg, which could only have been achieved by an enormous heart. Evidence for such an enormous heart does not exist and mechanisms to reduce the blood pressure required include the slowing of metabolism as these animals grew larger. It is likely that they did not routinely feed on tree tops but grazed on the ground.
Recommended Reading: Claratin Blood Pressure
How High Blood Pressure Can Damage Your Kidneys
Your heart, the key organ of the circulatory system, constantly pumps blood through your blood vessels. Good blood flow is essential for normal kidney function, and even minor blood flow problems can affect kidney function and increase your risk of serious health problems.
Although a certain amount of force is needed to push blood through the blood vessels, the pressure inside the vessels sometimes becomes too high. High blood pressure can damage the blood vessels that lead to the kidneys, causing them to stiffen or narrow.
As a result, less blood reaches your kidneys, making it difficult for the organs to function properly. Tiny blood vessels inside the kidneys that filter blood may also be damaged.
How Is My Blood Pressure Normally Regulated
To control your blood pressure, your body must adjust how much blood is pumped through your heart. Your body must also adjust the amount of pressure in your blood vessels.
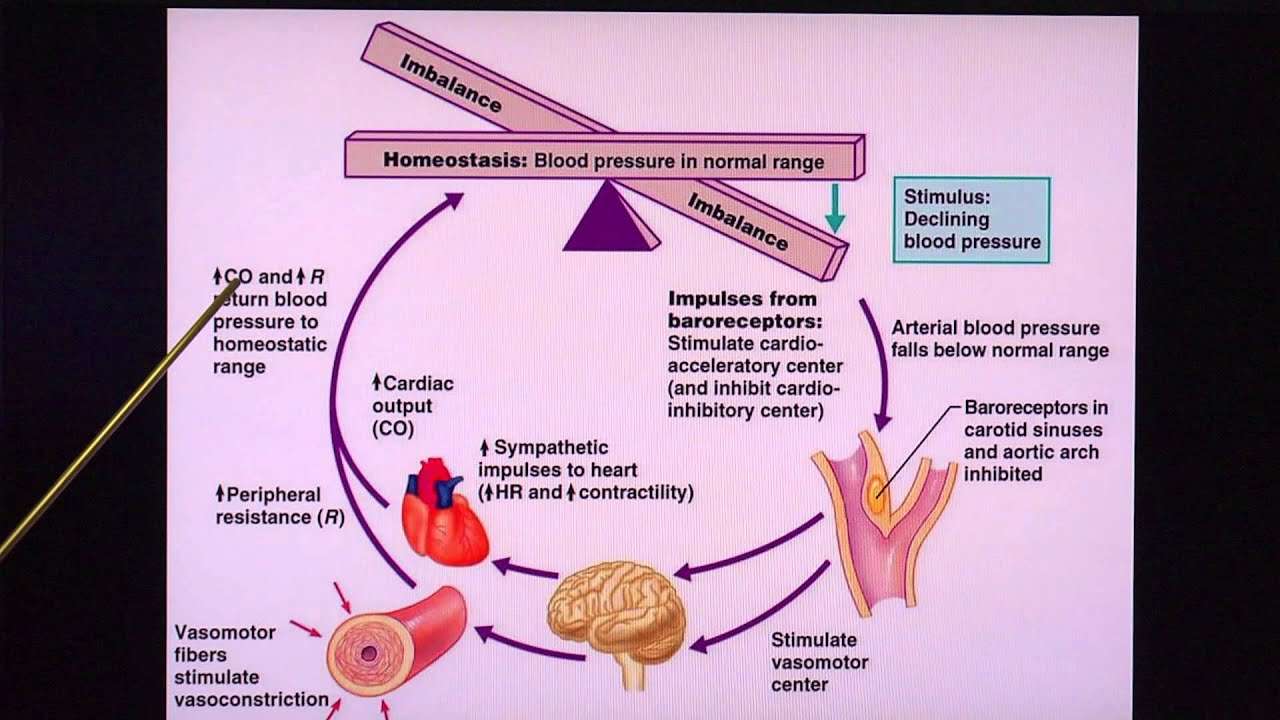
How Your Brain Responds. When your blood pressure begins to fall too low, a signal is sent to your brain. Your brain responds by producing chemicals called neurotransmitters. Certain neurotransmitters, called catecholamines, cause your heart to beat faster and more forcefully and cause your blood vessels to tighten. These actions increase your blood pressure.
How Your Kidneys Respond. The change in the rate and force of your beating heart also causes a change in the amount of blood flowing through your kidneys. Your kidneys react to low blood pressure by producing a chemical called renin, which causes blood vessels to tighten. Renin is converted to a chemical called angiotensin II, which further tightens your blood vessels. In addition, neurotransmitters are thought to make the kidneys produce more renin, increasing blood pressure even more.
Read Also: Mayo High Blood Pressure
Homeostatic Physiological Adaptations Vs Pathological Processes
Physiological adaptations to various stressors often lead to adaptive, beneficial changes, but may also lead to pathological processes, particularly in chronic states. Taylor and Tan raise the intriguing question as to whether the age-related increase in muscle sympathetic nerve activity is obligatory for an age-related increase in mean arterial blood pressure. The authors raise the question because not all middle-aged and older individuals that have high sympathetic activity have hypertension. In addition, the authors propose that the age-related changes in cardiac output, total peripheral vascular resistance and blood pressure can be explained as parallel phenomena rather than a deterministic outcome of physiological aging. Their argument is supported by identifying that although there is an age-related increase in sympathetic outflow there is evidence that its effect on peripheral vasoconstriction is diminished. The mechanism involved in the reduced sympathetically-mediated peripheral vasoconstriction may be a function of diminished alpha-1 adrenergic receptor density in relation to available nitric oxide and/or beta-2 adrenergic receptor density providing more vasodilator capacity in response to circulating catecholamines. The authors conclude that the high sympathetic activity in the elderly is likely to be homeostatic in terms of maintaining normal mean BP, and is not a primary cause of increased total peripheral vascular resistance and hypertension.