Why Pah Is Hard To Diagnose
PAH is difficult to spot and diagnose, even when your doctor is looking for it during a physical exam. The symptoms of PAH mimic those of other similar conditions. Even as PAH progresses, your doctor may have trouble distinguishing it from other heart and lung conditions.
Your doctor will assess your medical history and use one or more tests to determine whats causing your symptoms.
Intravascular Ultrasound And Optical Coherence Tomography In Pah
Intravascular ultrasound and optical coherence tomography can demonstrate intimal fibrosis, a surrogate marker of pulmonary arterial remodelling that correlates negatively with pulmonary arterial compliance and is associated with unfavourable clinical outcomes during mid-term follow-up . OCT has shown development of pulmonary arterial remodelling in patients with borderline PH and the occurrence of reverse remodelling following effective treatment .
What Raises A Persons Risk Of Developing Pulmonary Hypertension
Risk factors for developing pulmonary hypertension include:
- Family history of blood clots.
- Family history of pulmonary hypertension.
- Living at high altitudes.
- Smoking and using tobacco products.
- Use of diet medications such as fen-phen .
- Use of some prescription medications that treat cancer and depression.
- Use of recreational drugs.
- Liver disease.
- Lung disease.
Talk with your provider about your risk factors and what you can do to lower your risk.
Don’t Miss: Does Melatonin Lower Blood Pressure
Pulmonary Versus Systemic Blood Pressure
Unlike systemic blood pressure, which represents the force of your blood moving through the blood vessels in your body, pulmonary blood pressure reflects the pressure the heart exerts to pump blood from the heart through the arteries of the lungs. In other words, it focuses on the pressure of the blood flow in your lungs.
How Does Pulmonary Hypertension Affect My Body
Pulmonary hypertension can cause serious problems in your body, including:
PH is dangerous for people who are pregnant. It can cause complications for both the birthing parent and fetus.
Without treatment, pulmonary hypertension can overtax your heart and eventually be fatal. High blood pressure in your pulmonary arteries forces your heart to work harder to send oxygen-poor blood to your lungs. Your right ventricle is responsible for pumping this blood to your lungs. So, over time, PH causes your right ventricle to get bigger due to the extra work. This condition can lead to right-sided heart failure.
Right-sided heart failure has a ripple effect throughout your body. It can disrupt the normal workings of many organs and systems.
Because pulmonary hypertension can affect your entire body, its essential that youre diagnosed and treated as early as possible. Your provider will prescribe treatment based on whats causing your PH. No matter the cause, untreated PH is life-threatening.
Recommended Reading: How High Is High Blood Pressure
Assessing Your Medical History
To help diagnose PAH, your doctor should assess your personal risk factors for the condition. For example, they should look for any conditions that might contribute to PAH or make the disease worse. You have an increased risk of PAH if you have:
- heart disease
- a family history of PAH
Your doctor may perform genetic screening to see if you have genes linked to PAH.
Your doctor may use the following methods to diagnose PAH:
Scleroderma And Scleroderma Spectrum
The 5th WSPH report, the 2015 European Society of Cardiology /European Respiratory Society PH guidelines and the NIH-supported 2013 CTD-PAH guidelines recommend annual screening in patients with systemic sclerosis . All guidelines recommend the DETECT algorithm in patients with SSc spectrum disorders ) associated with DLCO< 60% of predicted and disease duration > 3years. The current diagnosis Task Force undertook a systematic review of the published literature for screening tools available for CTD-PAH . The review supports incorporating TTE, DETECT or forced vital capacity /DLCO ratio > 1.6 and blood markers in SSc spectrum disorders. Based on this data and on the published guidelines, this Task Force recommends the incorporation of DETECT, TTE or FVC/DLCO ratio with elevated NT-proBNP to screen for SSc spectrum disorders. Although the prevalence of PAH is lower in those with DLCO80% of predicted, review of two large cohorts in the USA suggested that PAH is present in these patients.
Recommendations
- For patients with SSc and SSc spectrum with uncorrected DLCO< 80% of predicted, annual screening should be considered. The appropriate screening tools include DETECT, the 2015 ESC/ERS recommendations for TTE or FVC/DLCO ratio > 1.6 and > 2-fold upper limit of normal of NT-proBNP. If any of these screening tests are positive, these patients should be referred for RHC. For those with uncorrected DLCO80% of predicted, screening may be considered with TTE.
You May Like: What Kind Of Tea Is Good For High Blood Pressure
What Are The Stages Of Pulmonary Hypertension
There are four main stages of pulmonary hypertension. The World Health Organization calls these functional classes. Theyre based on the symptoms you feel and refer to how well you can carry out your daily activities. As PH gets worse, the symptoms become more noticeable and more disruptive to your daily life.
- Class 1: You dont have any symptoms.
- Class 2: You dont have symptoms when youre resting. But you feel some discomfort or shortness of breath during some routine activities. These include household chores and climbing stairs.
- Class 3: You may still feel fine when youre resting. But its now much harder to do normal tasks because you feel tired or short of breath.
- Class 4: You have symptoms even when youre resting. The symptoms get worse when you try to do any normal task.
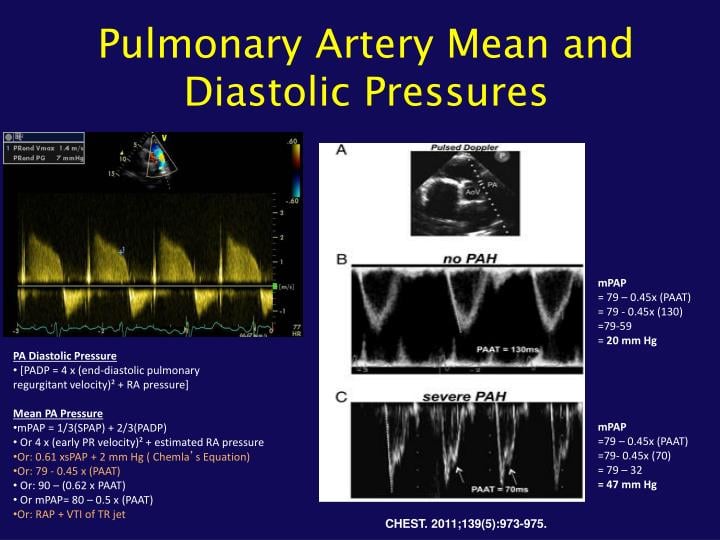
Mean Pulmonary Pressure Diastolic Pulmonary Pressure And Pulmonary Vascular Resistance
Echocardiography permits calculation of mean and even diastolic pulmonary artery pressure. Although these calculations are rarely performed, they may help the investigator to confirm the diagnosis or cause him/her to suspect the diagnosis in ambiguous situations . Pulmonary artery diastolic pressure can be estimated by looking at the pulmonary regurgitation signal . The velocity at end-diastole is converted into a pressure gradient . The estimate of right atrial pressure is added to this value.
sPAP= PRvel2 x 4 + RAP
Another means of estimating mean pulmonary artery pressure is by using the maximal PR velocity and applying the following formula.
MPAP = 4x peak PR velocity
Pulmonary regurgitation, CW Doppler spectrum. Diastolic pulmonary pressure can be measured from end-diastolic velocity.
It is also possible to measure mean pulmonary pressure from the pulmonary “forward” flow signal using Mahan’s regression equation:
MPAP =79 – 0.45
Several studies have shown that pulmonary vascular resistance can be calculated with echocardiography. This is done by measuring maximal tricuspid velocity and the velocity-time integral across the pulmonary valve and using the following formula:
Catheter = /CO
Others have suggested using the velocity-time interval across the left ventricular outflow tract instead:
TR vel / TVI LVOT
Also Check: What Causes A Low Pulse With High Blood Pressure
Preparing For Your Heart Catheterization
Before the heart catheterization a doctor will explain the risks and benefits of this procedure. You will remain without food or drink 12 hours before the procedure. You may take you regular a.m. medications on the day of the procedure however you should hold any blood thinners or diabetic medications.
When To See Your Doctor
How Pulmonary Arterial Hypertension Is Diagnosed
Because symptoms are similar to other common lung diseases, it can often be hard to diagnose PAH. Diagnosis is a process of eliminating other diseases. With the help of lung and heart specialists you will need to take a number of tests, such as:
- Blood tests: Include HIV, thyroid tests, autoimmune disease panels , liver tests and blood chemistry tests.
- Electrocardiogram: Shows the electrical activity of the heart and may help detect abnormalities. Doctors may also be able to detect signs of strain on the right side of the heart.
- Lung function tests : Check for diseases like asthma or emphysema.
- 6-Minute Walk Test: Objectively measures how far you can walk and to see if your oxygen levels drop when you exert yourself.
- Echocardiogram: Ultrasound of the heart to check the size and condition of the chambers of the heart. It can also be used to estimate the blood pressure in the pulmonary arteries.
- Right Heart Catheterization: This test is invasive, so it is not usually performed unless other tests cannot produce a firm diagnosis. It involves inserting a catheter into a large vein in either the neck, arm, or groin, and threading it through the right side of the heart and into the pulmonary artery. This allows measurement of the blood pressure in the lungs.
Read Also: Does Smoking Weed Lower Blood Pressure
Pulmonary Hypertension In Echocardiography
So what does echocardiography, or cardiac ultrasound, have to do with pulmonary hypertension? Well, to be honest, echo plays a critical role in screening for pulmonary hypertension.
In the same article from the Journal Of The American Society of Echocardiography, it mentions that, Given the nonspecific symptoms and subtle physical signs, particularly in the early stages, a high clinical index of suspicion is necessary to detect the disease before irreversible pathophysiologic changes occur. In this regard, transthoracic echocardiography, by providing direct and/or indirect signs of elevated pulmonary artery pressure , is an excellent noninvasive screening test for patients with symptoms or risk factors for PAH, such as connective tissue disease, anorexigen use, pulmonary embolism, heart failure, and heart murmurs. It may also provide key information on both the etiology and the prognosis of PH.
In short, what their saying is that echo is a great way to not only screen for PHTN, but that echo also provides information on the cause and the prognosis.
So as a cardiac sonographer, if you havent noticed yet, we tend to get a lot of patients who have already been diagnosed with pulmonary hypertension, or who are suspected of having pulmonary hypertension.
But what is it specifically we should be looking for with echocardiography in these pulmonary hypertension cases?
Well thats exactly what were going to go over in this article
So lets dive right in.
Pulmonary Hypertension Guidelines For Echo: And How To Measure Rvsp
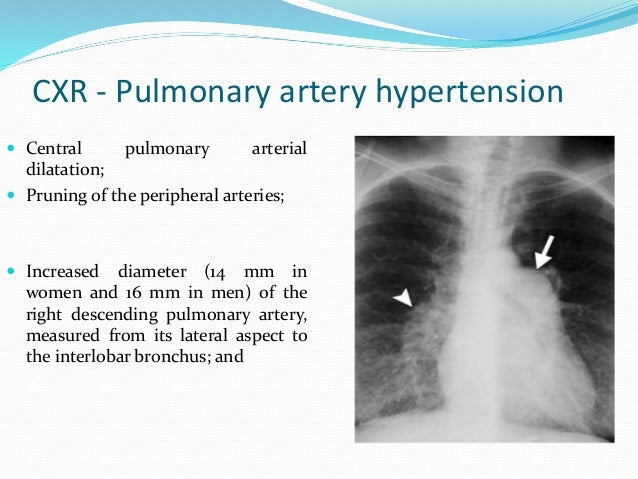
You probably dont need to be told that echocardiography plays a major role in the noninvasive assessment of pulmonary hypertension. Echo is used to not only screen for the disease, but to determine right and left heart structure and function as well as monitor the progress of patients undergoing treatment for pulmonary hypertension.
You May Like: When To Take Blood Pressure Medication
What Are The First Symptoms Of Pulmonary Hypertension
The first symptom of pulmonary hypertension is shortness of breath during your daily activities. These may include climbing stairs or grocery shopping. You may also feel short of breath when you exercise.
At the start of pulmonary hypertension, you may not have any symptoms. When you do start to notice symptoms, they may be mild. But PH symptoms get worse over time, making it harder for you to do your usual activities.
Who Does Pulmonary Hypertension Affect
Pulmonary hypertension can affect adults at any age. It commonly affects people who have heart or lung conditions. Its also more common among people with other medical conditions. PH affects:
- Nearly 100% of people with severe mitral valve disease.
- About 65% of people with aortic valve disease.
- Up to 30% of people with scleroderma.
- About 20% to 40% of people with sickle cell disease.
- About 1 in 200 people with HIV.
PH usually affects adults. But rarely, it can affect newborns. This is called persistent pulmonary hypertension of the newborn . Infants with this condition may need treatment in the intensive care unit.
Don’t Miss: What Is The New Normal Blood Pressure
Diagnostic Approach In Patients With Clinical Suspicion For Ph/pulmonary Arterial Hypertension
PH due to parenchymal, cardiac, thromboembolic and other diseases is associated with worse outcomes and limited treatment options, resulting in referral of these patients to PH centres. Guidelines for the diagnosis and management for these subgroups are addressed separately by the relevant 6th World Symposium on Pulmonary Hypertension Task Force articles in this issue of the European Respiratory Journal .
Cardiac Index Evaluation Of Intracardiac Shunt Venous Oxygen Saturation Uric Acid
The determination of cardiac index is essential for the diagnostic work-up and follow-up programme in patients with PH. The thermodilution technique is used in the vast majority of PH centres. In patients with severe PH, a recent study indicates that thermodilution was equally accurate to the Fick method over a broad range of cardiac output values . Although conflicting results have been published, the agreement between the two methods was not affected by the severity of tricuspid regurgitation . In most cases of PH, the accuracy of the thermodilution technique is acceptable. However, in case of intracardiac shunt, as in the patients with patent foramen ovale, the thermodilution technique is inappropriate. Only the Fick method, with measurement of pulmonary venous O2 content is able to measure pulmonary blood flow.
Oximetry is required to exclude intracardiac shunting. Further investigations may also be required although they do not intrinsically belong to the standard evaluation of PH. The high pulmonary blood flow-related hyperkinetic component of PH is often associated with vasoconstriction and arterial remodelling . The prevalence of patent foramen ovale in PH is similar to the normal population, and this finding provides no detectable influence on resting haemodynamics or exercise tolerance in patients with PH .
Don’t Miss: How Does Blood Pressure Medicine Work
Sleep Study And/or Overnight Oximetry Study
One of the causes of pulmonary hypertension is poor quality breathing during sleep. If someone’s oxygen levels are low during sleep, this condition puts a lot of strain on the lungs and heart and may lead to pulmonary hypertension. Since a patient would be asleep when these abnormalities of breathing are occurring, she/he may not feel that their breathing is limited during sleep and may not be aware of this.
- A sleep study is a study done in a sleep center . The patients come to the sleep center in the evening, get hooked up to different monitors including an oxygen monitor and are asked to sleep . When they wake up in the morning, they go back home. If a patient indeed has trouble with her/his breathing when asleep, they may need to be on oxygen or use certain masks, such as a CPAP , at night to help with their breathing and to improve their pulmonary hypertension.
- An overnight oximetry study is a test in which a recording “pulse oximeter monitor” continuously measures a patient’s oxygen level and heart rate overnight. This test could be done in someone’s home. This is more convenient than the sleep study but does not give us all the information needed.
What Medications Treat Pulmonary Hypertension
Pulmonary vasodilators are medications that treat PAH and CTEPH. They cant be used for other types of PH, including those caused by underlying heart or lung issues.
Pulmonary vasodilators help your pulmonary arteries relax. This lowers blood pressure and eases the load on the right side of your heart.
People with PH may take a variety of other medications based on their underlying conditions.
Recommended Reading: What Causes High Blood Pressure And Low Heart Rate
What Is Pulmonary Hypertension
The heart has 2 sides. The right side of the heart gets blood from the body and it sends this blood to the lungs to be ‘cleaned’. The lungs give oxygen to this blood and get rid of toxic gases such as carbon di-oxide . This ‘clean’ blood now makes its way to the left side of the heart which then gets pumped to the rest of the body. Then the blood makes its way back to the right side of the heart, and so on and so forth. This is a continuous cycle that happens minute after minute throughout our life.
Most people have heard the term “hypertension” which is increased pressure. But this typically refers to increased pressure that the left side of the heart is exposed to, and is measured usually with a cuff that is wrapped around a person’s arm. This is very different from, and is usually not associated with, “Pulmonary Hypertension”.
Pulmonary hypertension reflects increased pressures in the blood vessels in the lungs, which makes it difficult for the right side of the heart to send blood to the lungs to be ‘cleaned’. This is not easily directly measured and requires both non-invasive clues as well as invasive means to accurately measure.
Ph Associated With Chronic Thromboembolic/embolic Disease
A thrombus or thromboembolism is a blood clot that blocks the passage of blood through a vessel. If blood clots travel to the lung, the obstruction may lead to pulmonary hypertension. Sometimes blood clots in the lungs do not cause symptoms. Pulmonary Hypertension caused by blood clots is rare and may require surgical removal of the clots by a procedure called thromboendarterectomy.
There are many diseases that can cause pulmonary hypertension . The following is a brief explanation of each of these conditions.
Don’t Miss: What Is The Best Wrist Blood Pressure Monitor
Right Ventricular Systolic Pressure And Echo
The way we do this is by using echo to measure the right ventricular systolic pressure, or RVSP.
Right Ventricular Systolic Pressure in echo is obtained by simply measuring the pressure gradient of the tricuspid regurgitant jet.
How To Measure RVSP in Echo
To measure the RVSP in echo, all you need to do is line up your cursor parallel with the tricuspid regurgitant jet and turn on continuous wave Doppler. This will give you the peak velocity of the TR jet.
Now to find out the pressure gradient, all you need to do is plug it into the formula 4V2. Heres what it will look like.
Pressure Gradient Formula: 4 x V2
Example #1:
Say that the peak TR velocity was 2.5 m/s. We would start by multiplying that by itself .
V2 = 2.5 x 2.5
4 x 13.69 = 54.76 mmHg
Medical History And Physical Exam
Your doctor may ask you about any symptoms you have been experiencing and any risk factors such as other medical conditions you have.
Your doctor will also perform a physical exam to look for signs that may help diagnose your condition. As part of this exam, your doctor may do the following:
- Check whether the oxygen levels in your blood are low. This may be done by pulse oximetry, in which a probe is placed on your finger to check your oxygen levels.
- Feel your liver to see if it is larger than normal.
- Listen to your heart to see if there are changes in how it sounds, and also to find out if your heartbeat is faster than normal or irregular or if you have a new heart murmur.
- Listen to your lungs for sounds that could be caused by heart failure or interstitial lung disease.
- Look at the veins in your neck to see if they are larger than normal.
- Look for swelling in your abdomen and legs that may be caused by fluid buildup.
- Measure your blood pressure.
Don’t Miss: What Is The Normal Blood Pressure For Adults