How Does Aldosterone Act In The Body
Aldosterone acts in the body by binding to and activating a receptor in the cytoplasm of renal tubular cells. The activated receptor then stimulates the production of ion channels in the renal tubular cells. It thus increases sodium reabsorption into the blood and increases potassium excretion into the urine.
aldosterone, a steroid hormone secreted by the adrenal glands. Aldosterone serves as the principal regulator of the salt and water balance of the body and thus is categorized as a mineralocorticoid. It also has a small effect on the metabolism of fats, carbohydrates, and proteins.
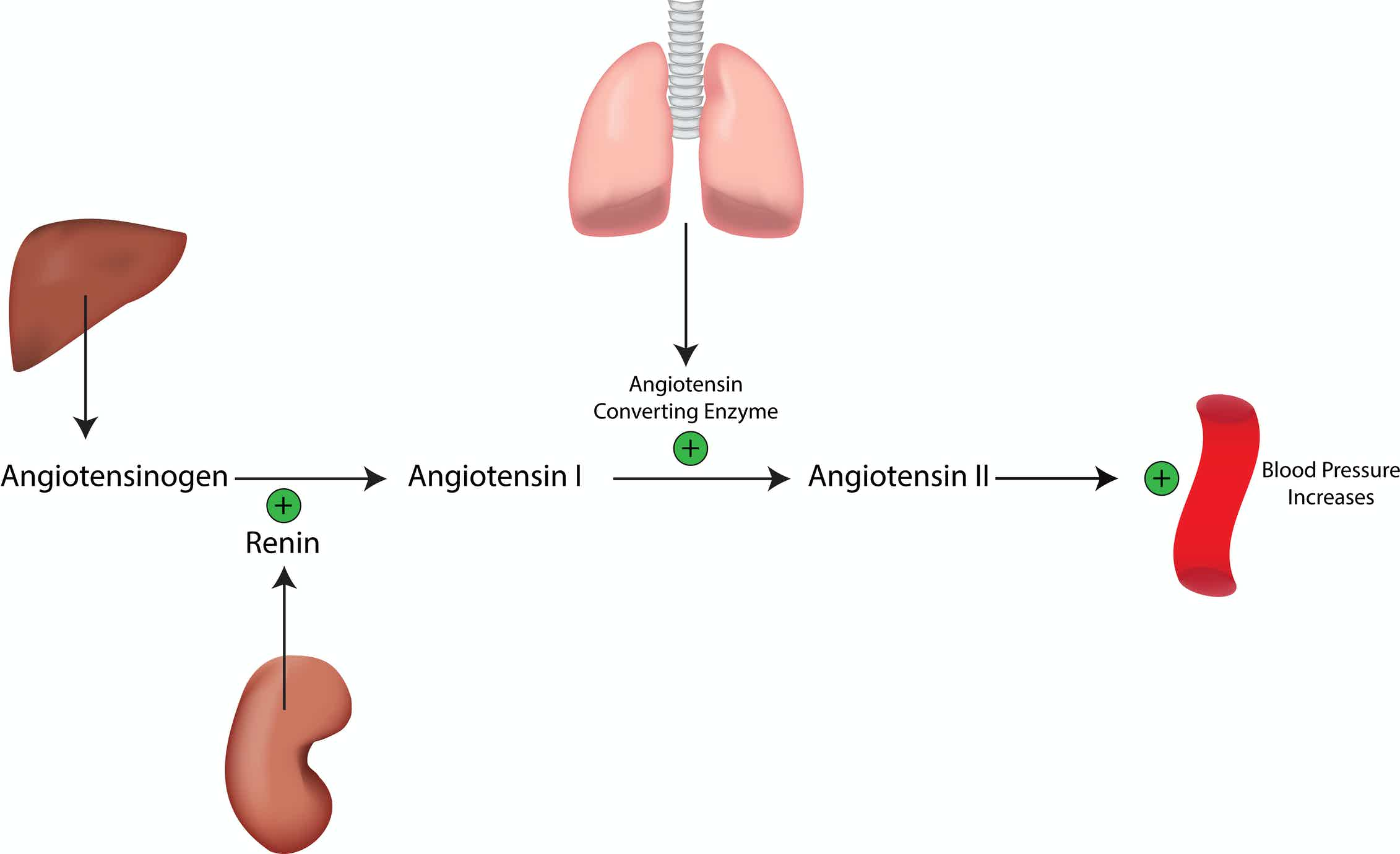
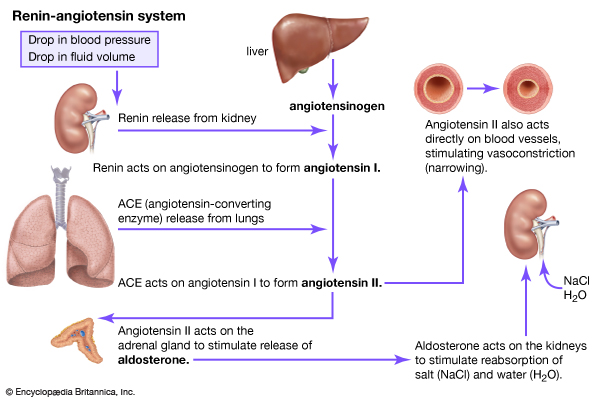
Aldosterone is synthesized in the body from corticosterone, a steroid derived from cholesterol. Production of aldosterone in the zona glomerulosa of the adrenal cortex is regulated by the renin-angiotensin system. Renin is secreted from the kidneys in response to variations in blood pressure and volume and plasmasodium and potassium levels. Renin acts on a protein circulating in the plasma called angiotensinogen, cleaving this substance into angiotensin I. Angiotensin I is subsequently converted to angiotensin II, which stimulates the release of aldosterone from the adrenal glands.
Pure aldosterone was isolated from beef adrenal glands in 1953 by research groups in England and Switzerland. By 1956 its structure was established, and it was synthesized from other steroids. The availability of other mineralocorticoids as therapeutic agents greatly restricts the use of aldosterone in therapy.
Rna Isolation Reverse Transcription
Total RNA was extracted using RNeasy mini kit and reverse transcribed by M-MLV . Derived complementary DNAs were amplified using PCR master mix . Primer sequences for hAS were as follow: 5-GTG GCG TGT TCT TGT TGA ATG-3 and 5-GGT GGA TTT GAA CAT GAC CTC-3. -actin was amplified as a reference gene with primers 5-ACCGCTCGTTGCCATTAGTGATGA-3 and 5-AAGGCCAACCGTGAAAAGATGACC-3.
The Classical Ras Pathway And High Blood Pressure
The classical RAS pathway is known to be an important factor in heart disease. One heart disease that is common in the United States is chronic high blood pressure, also known as hypertension. According to the Centers for Disease Control and Prevention , hypertension affects approximately half of adults in the United States.
Some people with hypertension have no identifiable cause. This is referred to as primary, or essential, hypertension. Other people have hypertension due to secondary causes. Secondary hypertension can be caused by hormonal imbalances in the classical RAS pathway. For example, a tumor in the adrenal gland can release excessive amounts of aldosterone and lead to fluid retention and high blood pressure.
Many scientific papers, conference presentations, and textbooks have been written about the importance of the classical RAS pathway in blood pressure regulation. This is an area of research still being pursued by scientists more than 50 years after the discovery of the system.
The details of the renin-angiotensin-aldosterone system continue to be investigated and could help us further understand:
- Why people develop primary hypertension
- Why some people don’t respond well to typical high blood pressure treatment
- Why some people with high blood pressure develop more complications than others
Recommended Reading: Does Vodka Raise Blood Pressure
What Is An Aldosterone/renin Ratio
An aldosterone/renin ratio is a screening test to detect primary aldosteronism in high-risk, hypertensive individuals. To determine the ratio, blood levels of aldosterone and renin are measured and a calculation is done by dividing the aldosterone result by the renin result. The ARR is considered the most reliable screening for primary aldosteronism, though it is not straightforward to interpret. Anything that could interfere with the test, such as medications, posture, sodium intake, and plasma potassium, needs to be taken into account before the test to avoid false positives or false negatives. Other tests, like suppression tests, are used to confirm the diagnosis after screening.
Direct Cardiac Effects Of Mineralocorticoids
For aldosterone to have direct, specific effects in the heart, it is necessary that the mineralocorticoid receptor be expressed. Moreover, glucocorticoids are potential ligands for the mineralocorticoid receptor and are normally prevented from occupying it by 11-hydroxysteroid dehydrogenase-2 , an enzyme in mineralocorticoid target tissues that converts cortisol and corticosterone to inactive cortisone and 11-dehydrocorticosterone, respectively . In addition, aldosterone may have rapid nongenomic effects on cardiac function through pathways that have yet to be completely defined . However, most of the pathological processes discussed in this review have a time course measured in weeks, consistent with effects mediated by classic mineralocorticoid receptors.
In fact, both the mineralocorticoid receptor and 11-HSD2 are expressed in the human heart , consistent with the idea that aldosterone could affect the heart directly and not just through its pressor effects. However, the heart is comprised of several types of cells, including cardiomyocytes, fibroblasts, endothelial cells, neurons, and vascular smooth muscle cells. Moreover, these cell types are not functionally equivalent throughout the heart due to the dramatically different pressure loads experienced by the various chambers of the heart. The potential cardiac effects that aldosterone might have obviously depend on the cell types and regions in which the mineralocorticoid receptor and 11-HSD2 are expressed.
You May Like: Do Onions Lower Blood Pressure
How Is It Used
Aldosterone and renin tests are used to evaluate whether the adrenal glands are producing appropriate amounts of aldosterone and to distinguish between the potential causes of excess or deficiency. Aldosterone may be measured in the blood or in a 24-hour urine sample, which measures the amount of aldosterone removed in the urine in a day. Renin is always measured in blood.
These tests are most useful in testing for primary aldosteronism, also known as Conn syndrome, which causes high blood pressure. If the test is positive, aldosterone production may be further evaluated with stimulation and suppression testing.
Both aldosterone and renin levels are highest in the morning and vary throughout the day. They are affected by the bodys position, by stress, and by a variety of prescribed medications.
What Does The Raas System Do
When there is decreased blood flow to the kidneys, and low blood pressure, the RAAS system is triggered.
- Angiotensin II causes vasoconstriction of the afferent arterioles in the nephrons, which increases sodium and water reabsorption by the kidneys.
- Angiotensin II causes aldosterone to be released from the adrenal cortex. Remember that aldosterone causes the reabsorption of sodium and water by the kidneys.
- Angiotensin II causes vasoconstriction of blood vessels throughout the body. When the blood vessels are constricted, that helps to increase blood pressure.
Understanding these hormones and how this system works is crucial to understanding the pathophysiology of the related diseases and disorders of the Endocrine System. The Medical-Surgical Nursing – Endocrine video tutorial series is intended to help RN and PN nursing students study for nursing school exams, including the ATI, HESI and NCLEX.
Read Also: Do Onions Lower Blood Pressure
How Does Cortisol Cause Hypertension
cortisolcausing hypertensionCortisolhypertensionCortisol
. Beside this, how does cortisol increase blood pressure?
1. In humans, the hypertensive effects of adrenocorticotropic hormone infusion are reproduced by intravenous or oral cortisol. Oral cortisol increases blood pressure in a dose-dependent fashion. Cortisol-induced hypertension is accompanied by a significant sodium retention and volume expansion.
Also Know, can too much cortisol cause high blood pressure? Excess cortisol could result from a tumor or as a side effect of some medications. Too much cortisol can lead to Cushing’s syndrome. Symptoms include: high blood pressure.
One may also ask, how does Cushing’s cause hypertension?
Untreated Cushing’s syndrome can lead to heart disease and increased mortality. Cortisol can also exhibit mineralocorticoid activity in high concentrations, worsening the hypertension and leading to hypokalemia and hypernatremia .
What are the symptoms of high cortisol levels?
High cortisol level symptoms
What Are The Symptoms
The main symptom of hyperaldosteronism is high blood pressure, which can range from moderate to severe. In some cases, high blood pressure related to hyperaldosteronism doesnt respond to medication. In others, it may only respond to a certain combination of medications.
High blood pressure doesnt typically have symptoms. But when it does, they can include:
- headaches
There are two types of hyperaldosteronism, known as primary and secondary hyperaldosteronism. While they have similar symptoms, their causes are different.
Don’t Miss: Do Onions Lower Blood Pressure
Control Of Aldosterone Release From The Adrenal Cortex
The role of the reninangiotensin system
Angiotensin is involved in regulating aldosterone and is the core regulation. Angiotensin II acts synergistically with potassium, and the potassium feedback is virtually inoperative when no angiotensin II is present. A small portion of the regulation resulting from angiotensin II must take place indirectly from decreased blood flow through the liver due to constriction of capillaries. When the blood flow decreases so does the destruction of aldosterone by liver enzymes.
Although sustained production of aldosterone requires persistent calcium entry through low-voltage-activated Ca2+ channels, isolated zona glomerulosa cells are considered nonexcitable, with recorded membrane voltages that are too hyperpolarized to permit Ca2+ channels entry. However, mouse zona glomerulosa cells within adrenal slices spontaneously generate membrane potential oscillations of low periodicity this innate electrical excitability of zona glomerulosa cells provides a platform for the production of a recurrent Ca2+ channels signal that can be controlled by angiotensin II and extracellular potassium, the 2 major regulators of aldosterone production.Voltage-gated Ca2+ channels have been detected in the zona glomerulosa of the human adrenal, which suggests that Ca2+ channel blockers may directly influence the adrenocortical biosynthesis of aldosterone in vivo.
The plasma concentration of potassium
Adrenocorticotropic hormone
The role of sympathetic nerves
This Hormone Which Helps The Body Manage Water And Sodium Is A Focus Of Growing Interest Among Researchers
High blood pressure which has no symptoms or warning signs can harm your blood vessels, heart, brain, eyes, and kidneys. An estimated 46% of adults in the United States have this stealth condition. A combination of unhealthy habits, such as smoking, a poor diet, and lack of exercise, can contribute to a rise in blood pressure. While kidney disease may cause high blood pressure, for most people the underlying cause is unknown.
However, for about one of every 15 people with high blood pressure, an imbalance of the hormone aldosterone may be to blame. This problem may be even more common among people with poorly controlled high blood pressure . “Among those people, up to one in five may have too much aldosterone,” says Dr. Gail Adler, chief of cardiovascular endocrinology at Harvard-affiliated Brigham and Women’s Hospital.
To continue reading this article, you must log in.
- Research health conditions
- Prepare for a doctor’s visit or test
- Find the best treatments and procedures for you
- Explore options for better nutrition and exercise
You May Like: Does Spicy Food Cause High Blood Pressure
The Raa System And Covid
The Coronavirus disease 2019 , or SARS-CoV-2, led to a global outbreak that affected nearly 200 million people worldwide as of July 2021. The disease is associated with severe complications in people who have pre-existing cardiovascular diseases, such as hypertension and diabetes.
The renin-angiotensin system plays an important role in the COVID-19 infectious disease process.
The SARS-CoV-2 uses angiotensin-converting enzyme 2 as a “receptor” and cellular entry point to infect a wide range of cells in the body. More specifically, ACE 2, which is embedded in the surfaces of cells, is recognized by spike proteins on the COVID-19 virus. This recognition leads to a lock-and-key relationship that opens the door for the virus to enter.
Binding Of Angiotensin Ii
Angiotensin II exerts its action by binding to various receptors throughout the body. It binds to one of two G-protein coupled receptors, the AT1 and AT2 receptors. Most actions occur via the AT1 receptor.
The table below outlines its effect at different points. These will be discussed in more detail below.
| Site |
| Increases thirst sensation and stimulates anti-diuretic hormone release |
You May Like: How To Calibrate Blood Pressure Monitor Omron
Effects Of Aldosterone On Cardiac Fibrosis
The most widely used animal model for studying cardiac effects of aldosterone is the uninephrectomized rat given 0.9% saline to drink. Aldosterone may be continuously administered by osmotic minipump, in which case severe cardiac hypertrophy and fibrosis develop within weeks. Although severe hypertension typically develops in this model, cardiac hypertrophy and fibrosis are blocked by spironolactone at doses that do not ameliorate the hypertension .
These effects of aldosterone may involve direct stimulation of proliferation of cardiac myocytes and fibroblasts as well as a reparative response to inflammation and cell death .
Some of the discrepancies between these studies may reflect technical differences that result in important phenotypic differences in the cultured cells. Moreover, it is difficult to extrapolate the results of in vitro studies to an intact tissue consisting of several different cell types. Thus, it is uncertain whether aldosterone affects cardiac fibrosis in vivo by a direct effect on fibroblasts or an indirect mechanism.
Cyp11b2 Expression And Cardiac Production Of Aldosterone In Pathological States
The main interest in the role of aldosterone in the cardiovascular system concerns its effects in pathological states such as myocardial infarction or congestive heart failure. The expression of CYP11B2 was studied in rats subjected to myocardial infarction by coronary artery occlusion. In the noninfarcted myocardium of the left ventricle, myocardial infarction increased CYP11B2 mRNA, aldosterone levels, and angiotensin II levels. All of these changes were blocked by treatment with losartan, suggesting that these increases are mediated primarily by cardiac angiotensin II via the AT1 subtype receptor. The collagen deposition induced by myocardial infarction in noninfarcted left ventricular myocardium was prevented by both spironolactone and losartan . In a similar study enalapril failed to inhibit cardiac aldosterone production, although losartan was effective. This may be related to the phenomenon of aldosterone escape, which refers to the tendency of circulating aldosterone levels to return to normal or supranormal levels during long-term ACE inhibitor therapy of chronic heart failure . Similarly, CYP11B2 expression increased in rat hearts that developed experimental autoimmune myocarditis. Cytokine, chemokine, and extracellular matrix genes also increased . It is likely that the increase in CYP11B2 expression was a consequence of myocardial dysfunction induced by the myocarditis.
Recommended Reading: Do Onions Lower Blood Pressure
What Are The Physiologic Effects Of Aldosterone And How Does Dysfunction Contribute To Adrenal Crisis
Aldosterone is produced by multiple hydroxylations of deoxycorticosterone and is normally 60% protein bound. The renin-angiotensin system stimulates aldosterone release. Increased potassium stimulates aldosterone production, and decreased potassium inhibits production. Chronic adrenocorticotropic hormone deficiency may inhibit production.
The primary actions of aldosterone cause the kidneys, gut, and salivary/sweat glands to affect electrolyte balance. The primary targets are the kidneys where it stimulates reabsorption of sodium and secretion of potassium and hydrogen ions. The kidneys’ effect on sodium and potassium depend on the intake of these cations . The effects on hydrogen probably can occur independently.
Persistent aldosterone excess results in atrial natriuretic factor release and renal hemodynamic changes for compensation. Congestive heart failure and cirrhosis with ascites are exceptions that cause progressive sodium retention. Excess aldosterone results in sodium retention, hypokalemia, and alkalosis. Aldosterone deficiency results in sodium loss, hyperkalemia, and acidosis. Hyperkalemia stimulates aldosterone release to improve potassium excretion. Aldosterone is the first-line defense against hyperkalemia.
References
Ishii M. Endocrine Emergencies With Neurologic Manifestations. Continuum . 2017 Jun. 23 :778-801. . .
Elshimy G, Alghoula F, Jeong JM. Adrenal Crisis. StatPearls. 2020 Jan. . .
- Regulation of the adrenal cortex.
Why Is Adh Produced
ADH is secreted in response to three things.
Recommended Reading: Does Hot Sauce Cause High Blood Pressure
Primary Hyperaldosteronism Is A Disease Caused By An Adrenal Tumor That Produces Excess Of The Hormone Aldosterone The Excess Aldosterone From The Adrenal Tumor Causes High Blood Pressure And Is Named Conn’s Syndrome After The Doctor Who Discovered It Although The Symptoms May Be Mild Too Much Aldosterone In The Long Term Is Very Toxic And Can Cause Stroke And Heart Attacks
It breaks our heart to encounter patients on a weekly basis with Conn’s syndrome and primary hyperaldosteronism who have not been diagnosed and treated for years and decades. If you have Conn’s syndrome and primary hyperaldosteronism due to a benign aldosterone-producing adrenal tumor causing low potassium, high blood pressure and increased risk of stroke, heart attack, kidney failure and heart arrythmias, you need to take action. Unfortunatly, many patients are placed on medications just treating the symptoms of the disease. It does not remove the underlying tumor! Again, medications do not remove the tumor, surgery does.
What Is Being Tested
Aldosterone is a hormone that plays an important role in maintaining normal sodium and potassium concentrations in blood and in controlling blood volume and blood pressure. Renin is an enzyme that controls aldosterone production. These tests measure the levels of aldosterone and renin in the blood and/or the level of aldosterone in urine.
Aldosterone is produced by the adrenal glands located at the top of each kidney, in their
Aldosterone is a hormone that plays an important role in maintaining normal sodium and potassium concentrations in blood and in controlling blood volume and blood pressure. Renin is an enzyme that controls aldosterone production. These tests measure the levels of aldosterone and renin in the blood and/or the level of aldosterone in urine.
Aldosterone is produced by the adrenal glands located at the top of each kidney, in their outer portion . Aldosterone stimulates the retention of sodium and the elimination of potassium by the kidneys. Renin is produced by the kidneys and controls the activation of the hormone angiotensin, which stimulates the adrenal glands to produce aldosterone.
A variety of conditions can lead to aldosterone overproduction or underproduction . Since renin and aldosterone are so closely related, both substances are often tested together to identify the cause of an abnormal aldosterone.
Don’t Miss: Does Cholesterol Raise Blood Pressure