How Is Orthostatic Hypotension Diagnosed
Your healthcare provider will check your blood pressure while youre seated, lying down and standing. You may also get one or more of these tests:
- Blood tests to check for conditions like diabetes and anemia.
- Echocardiogram to check the hearts pumping action.
- Electrocardiogram to test for heart rhythm changes.
- Exercise stress test to measure heart rate during physical exertion.
- Portable EKG devices to measure heart rhythm.
- Tilt table test to safely measure blood pressure, heart rate and heart rhythm while you lie on a table that moves from horizontal to vertical.
When Do You Check Orthostatic Blood Pressure Ada Clarifies
Arefa Cassoobhoy, MD, MPH
Hello. I’m Dr Arefa Cassoobhoy, a practicing internist, Medscape advisor, and senior medical director for WebMD. Welcome to Morning Report, our 1-minute news story for primary care.
A Recommendation to Monitor Orthostatic Blood Pressure
We all know that blood pressure should be measured at every clinic visit, and now the American Diabetes Association adds a few clarifying points for patients with diabetes and hypertension.
Orthostatic blood pressure should be measured at initial visits for hypertension and then periodically. This includes checking a second blood pressure within 3 minutes of standing from a sitting or supine position. This can help monitor for autonomic neuropathy or volume depletion, which can get worse with high blood pressure medications. It’s important because orthostatic hypotension is common in people with hypertension and diabetes, and is linked to an increased risk for heart failure and death.
The ADA also recommends home blood pressure measurements to monitor for white coat hypertension or masked hypertension. Research suggests that this may even help with medication adherence.
The evidence is overwhelming. Reaching blood pressure goals with our patients reduces cardiovascular events and microvascular complications.
Follow Dr Cassoobhoy on Twitter at
Any views expressed above are the author’s own and do not necessarily reflect the views of WebMD or Medscape.
Tables
Orthostatic Blood Pressure & Adrenal Function
The orthostatic blood pressure test measures the supine blood pressure and then the standing blood pressure. The test is an indicator of how efficiently blood is pumped to the upper extremities. If cardiac output is weak, this will often result in orthostatic hypofunction: a decrease in systolic blood pressure upon standing. Conversely, if cardiac output is excessive, this will tend to result in orthostatic hypertension: an excessive increase in systolic blood pressure.
The implications for the orthostatic blood pressure tests are many. First of all, the orthostatic tests are reflective of several possible imbalances in the body.
- Autonomic nervous system stress. Orthostatic hyperfunction indicates excess sypathetic nervous system function and possible vasoconstriction. Orthostatic hypofunction indicates excess parasympathetic nervous system function and possible excess vasodilation.
- Electrolyte imbalance. In hypofunction, deficiencies of certain minerals like sodium can result in diminished cardiac output. In hyperfunction, a deficiency of potassium and magnesium may result in vasoconstriction.
- Adrenal Excess often found in a similar pattern with orthostatic hyperfunction.
- Adrenal Insufficiency often found with orthostatic hypofunction.
Recommended Reading: How To Calibrate Home Blood Pressure Monitor
Newbies Are The Worst Off
Interestingly, the more recently a person came down with ME/CFS, the worse off they were. The relative newbies those who have been ill for less than 4 years had the worst drops in pulse pressure, followed by those who had had ME/CFS for over ten years.
Why would people newer to ME/CFS have worse problems than those who had it longer? Perhaps because some sort of compensatory approach over time been developed. The autonomic nervous system can be trained and it can apparently adapt to some extent. My symptoms were certainly worse in the beginning.
Diastolic Blood Pressure Analysis
Patient characteristics in subjects with and without DBP OH are also shown in . There were also significantly more subjects that met criteria for DBP OH during the supine-to-standing test than during the sit-to-stand test using a 10 mmHg drop in each test . In those with DBP OH, the mean decline in DBP during the supine-to-standing test was 28.4 ± 0.8 mmHg, which was significantly larger than the decline during sit-to-stand testing . In those without DBP OH, the DBP increased during supine-to-standing testing on average by 6.0 ± 0.4 mmHg this was significantly different from sit-to-stand testing , which increased by 2.3 ± 0.4 mmHg on average.
You May Like: Stopping High Blood Pressure
Management: From A To F
The goal of management of orthostatic hypotension is to raise the patientâs standing blood pressure without also raising his or her supine blood pressure, and specifically to reduce orthostatic symptoms, increase the time the patient can stand, and improve his or her ability to perform daily activities. No specific treatment is currently available that achieves all these goals, and drugs alone are never completely adequate.
Therapies primarily consist of a combination of vasoconstrictor drugs, volume expansion, compression garments, and postural adjustment. Education about orthostatic stressors and warning symptoms empowers the patient to adopt easy lifestyle changes to minimize and handle orthostatic stress.
Because the mainstays of treatment are volume expansion and vasoconstriction, it is difficult to improve the symptoms of orthostatic hypotension without inducing some degree of supine hypertension. Strategies to minimize nocturnal hypertension and to treat orthostatic hypotension in special circumstances are summarized in .
What Is The Best Medicine For Orthostatic Hypotension
The most often prescribed medication is fludrocortisone: it causes an increase in blood volume. Midodrine can also be used 30 minutes before getting up, for example, and then 2 or 3 times a day.
Pyridostigmine may also be prescribed for mild hypotension. Also, medications that slow the emptying of the stomach can help treat postprandial hypotension in people with diabetes.
In all cases, close monitoring should be done by the doctor to avoid sudden increases in blood pressure. As a last resort, the installation of an electron systolic trainer can help treatment by increasing the basic heart rate.
You May Like: High Blood Pressure Mayo
Adrenal Fatigue Is Classified Through Sum Cortisol Output
On a salivary hormone test, adrenal fatigue is identified by the sum cortisol level. Cortisol is tested during 4 different intervals throughout the day: morning, noon, afternoon and evening. In a normal cortisol rhythm, cortisol is highest in the morning and progressively decreases throughout the day and evening. Abnormalities with cortisols rhythm tends to indicate various imbalances, including autoimmune processes, chronic infections and inflammatory processes.
It is the sum total of each of the 4 cortisol rhythms that determines adrenal hyper or hypo function. You can read more about these two contrasting physiological imbalances HERE.
When cortisol output is diminished, approximately 23 nM or less, it is a sign of low adrenal output and adrenal HYPOfunction. Conversely, when the sum cortisol level is greater than 40 nM, it is indicative of adrenal HYPERfunction.
A Decrease Of 20 Mm Hg Systolic Or 10 Mm Hg Diastolic
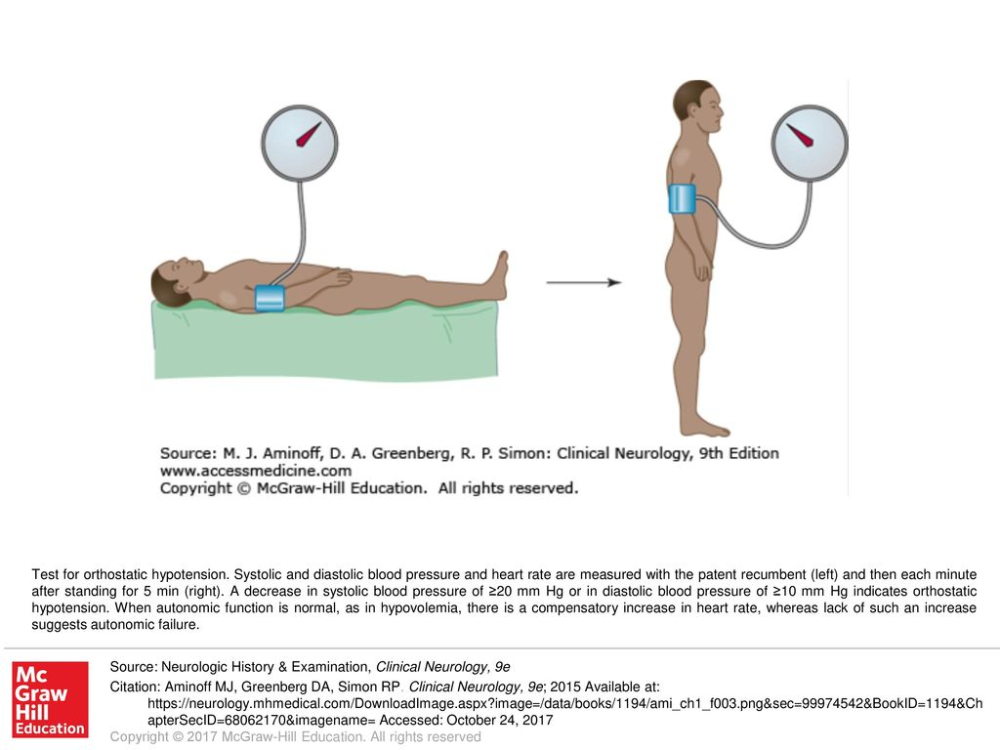
The consensus definition of orthostatic hypotension is a reduction of systolic blood pressure of at least 20 mm Hg or a reduction of diastolic blood pressure of at least 10 mm Hg within 3 minutes of erect standing. A transient drop that occurs with abrupt standing and resolves rapidly suggests a benign condition, such as dehydration, rather than autonomic failure.
In the laboratory, patients are placed on a tilt table in the head-up position at an angle of at least 60 degrees to detect orthostatic changes in blood pressure. In the office, 1 minute of standing probably detects nearly all cases of orthostatic hypotension however, standing beyond 2 minutes helps establish the severity . Orthostatic hypotension developing after 3 minutes of standing is uncommon and may represent a reflex presyncope or a mild or early form of sympathetic adrenergic dysfunction.,
Recommended Reading: High Blood Volume Symptoms
Treatment Of Orthostatic Hypotension
- Fluids to treat dehydration
- Management of diabetes, such as regular insulin injections
- Changes in medication or altered doses if drugs are the cause
- Medication, surgery or both to treat heart conditions
- Medication to increase blood volume or pressure, including corticosteroids
- Medications to treat orthostatic hypotension including pyridostigmine, a drug used in the treatment of myasthenia gravis
- A range of treatments, since orthostatic hypotension may have two or more causes
- In some cases, a lower body pressure suit is required.
Nasa Lean Test: An Easy Way To Diagnose Orthostatic Intolerance In Me/cfs Fibromyalgia And Pots
by Cort Johnson | Aug 25, 2020 | Bateman, Homepage, Orthostatic intolerance, Treatment |
We recommend that all ME/CFS and Fibromyalgia patients have a NASA 10-minute Lean Test to assess for orthostatic intolerance. Batetman Horne Center
The saga of the effort to introduce and validate the NASA Lean Test for ME/CFS just seems so right in so many ways. First the Bateman Horne Center identified a test from NASA no less that can easily be used to identify orthostatic intolerance .
Then they enrolled a large number of patients, got researchers involved, validated the test, and in doing so, learned something new about ME/CFS in the process. Its taken years to get through all this but in the end, it provides something thats really needed an easy test to identify orthostatic intolerance and get doctors engaged in treating ME/CFS as a biological phenomena they can help with.
The NASA Lean Test, validated by the Bateman Horne Center, is easy and requires just two simple instruments already found in doctors offices.
Orthostatic intolerance refers to the inability to stand without symptoms. Although most of us are completely unaware of it, successful standing up requires an array of processes to work properly.
The blood pressure at your arm momentarily drops as your blood starts to flow downwards, but then should bound back up as baroreceptors in the blood vessels tell your heart to beat faster. All this occurs automatically and below the level of consciousness.
Also Check: Apple Watch 2 Blood Pressure
How To Assess Orthostatic Hypotension
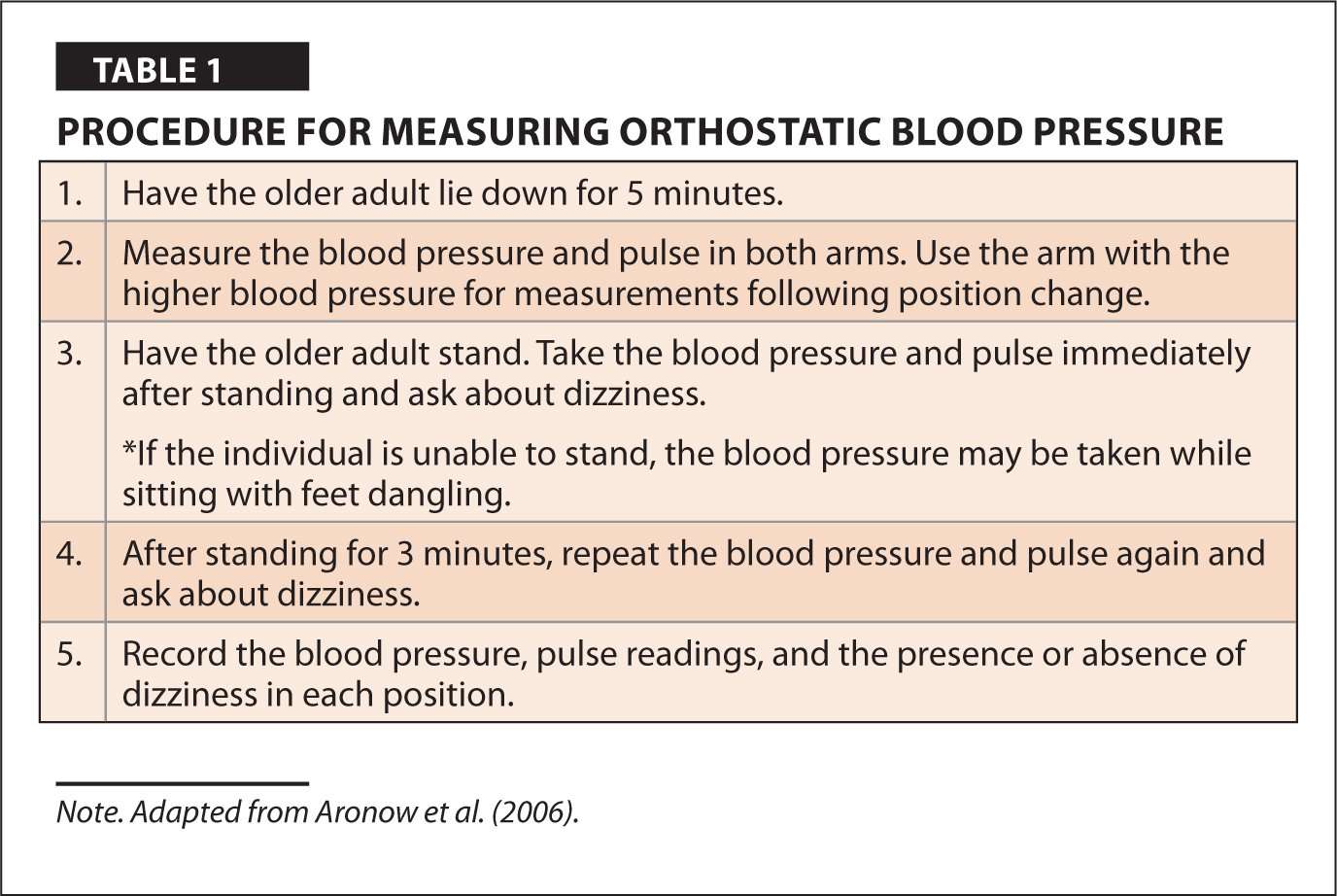
Orthostatic hypotension is assessed by measuring orthostatic or postural blood pressure and pulse changes. This procedure is done by assessing when the client moves from supine to sitting to standing. There are variations in how this procedure is done in terms of timing. Here is a common way to proceed:
Causes Of Orthostatic Hypotension
- Fever
- Some medications, such as some diuretics or antihypertensive medications
- Dehydration due to vomiting, diarrhoea or both, as in gastroenteritis
- Certain conditions, such as anaemia, diabetes, varicose veins or adrenal insufficiency
- Nervous system disease, such as Parkinsons disease or neuropathy
- Heart problems, including irregular heart beat , congestive heart failure, aortic stenosis or heart attack
- Spinal cord conditions such as syringomyelia
- Shy Drager syndrome, a degenerative disorder of the brain and spinal cord that affects functioning of the autonomic nervous system
- Significant blood loss.
Don’t Miss: Low Blood Pressure Shaking
Evaluation And Management Of Orthostatic Hypotension
JEFFREY B. LANIER, MD MATTHEW B. MOTE, DO and EMILY C. CLAY, MD, Martin Army Community Hospital Family Medicine Residency, Fort Benning, Georgia
Am Fam Physician. 2011 Sep 1 84:527-536.
Patient information: See related handout on orthostatic hypotension, written by the authors of this article.
Orthostatic hypotension is defined as a decrease in systolic blood pressure of 20 mm Hg or a decrease in diastolic blood pressure of 10 mm Hg within three minutes of standing compared with blood pressure from the sitting or supine position. Alternatively, the diagnosis can be made by head-up tilt-table testing at an angle of at least 60 degrees.1 Orthostatic hypotension is often found in older patients and in those who are frail.2 It is present in up to 20 percent of patients older than 65 years.3 In one study, the prevalence of orthostatic hypotension was 18 percent in patients older than 65 years, but only 2 percent of these patients were symptomatic.3
In the absence of volume depletion, younger patients with orthostatic hypotension usually have chronic autonomic failure. A related problem, postprandial hypotension, is common in older patients and those with autonomic dysfunction. In postprandial hypotension, there is a decrease in systolic blood pressure of at least 20 mm Hg within 75 minutes of a meal.4
When Should I Call The Doctor For Orthostatic Hypotension
Feeling faint or lightheaded is not normal. While a rare episode that can be explained by circumstances, such as working or exercising in the heat, may be ignored, more frequent occurrences should be investigated.
If a person passes out and is unconscious, even for a short period of time, is never normal and medical care should be accessed.
Recommended Reading: Can High Bp Cause Chest Pain
Old Age Is An Important Risk Factor
- Digestion when you eat and then digest food, an increased blood supply is sent to your intestines. Orthostatic hypotension is more likely to occur about 15 to 45 minutes after eating a meal .
- Standing if you stand up for a long time, it causes a slow but steady drop in blood pressure.
- Frailty and chronic sickness these are more common in old age.
Whats New: Earlier Oh Assessments Are More Informative Than Late Ones
This study found OH identified within 1 minute of standing to be more clinically meaningful than OH identified after 1 minute. Also, the findings reinforce the relationship between OH and adverse events, including injury and overall mortality. Evaluation for OH performed only at 3 minutes may miss symptomatic OH.
You May Like: Claritin And High Blood Pressure
Systolic Blood Pressure Analysis
illustrates subject characteristics comparing those who met the supine-to-standing SBP OH to those who did not. Overall, a large proportion of subjects had underlying autonomic or neurological conditions. There were very few subjects with non-neurogenic forms of OH in this cohort. There were significantly more subjects that met criteria for SBP OH during the supine-to-standing test than during the sit-to-stand test when using the conventional 20 mmHg drop in each test . In those with SBP OH, the mean decline in SBP during the supine-to-standing test was 58.7 ± 1.5 mmHg, which was significantly larger than the decline during sit-to-stand testing . In those without SBP OH, SBP increased during supine-to-standing testing on average by 3.6 ± 0.6 mmHg this was significantly different from sit-to-stand testing , which produced a small decline of 0.6 ± 0.6 mmHg on average.
How To Evaluate The Findings
Normal variation is a 10 mm Hg decrease in blood pressure from lying to standing and an increase in pulse of 1015 bpm.
A decrease in blood pressure from lying to standing of systolic 20 mm Hg or diastolic 10 mm Hg is identified as orthostatic hypotension.
An increase in pulse from lying to standing of 20 bpm is identified as orthostatic pulse.
Recommended Reading: Can You Take Your Blood Pressure Too Much
Determining The Risk Factors Of Orthostatic Hypotension
Duration Matters Less Is Not More
Time matters this study validated the results of another tilt table study which indicated that the 1-3 minute orthostatic assessment typically carried out in doctors offices isnt enough. Even a 2-5 minute tilt table test will miss a considerable set of POTS patients.
The Lee-Bateman study found that at least 5 minutes of the NASA lean test are necessary to pick up signs of orthostatic intolerance in most of the participants and a full ten minutes are needed to pick up more.
Don’t Miss: To Lower Blood Pressure
How Can I Prevent Orthostatic Hypotension
If youre prone to orthostatic hypotension, these steps can reduce symptoms:
- Keep your temperature moderate: Dont take very hot baths or showers.
- Stay hydrated: Drink plenty of water, limit alcohol and avoid heavy, high-carbohydrate meals.
- Dont sleep flat: Elevate your head at night by using more pillows or tilting the mattress.
- Prepare before standing: Give yourself more time to move into a standing position after sitting or lying down. Have something sturdy nearby to hold onto when you stand up.
- Move your muscles: March your feet if you must stand for prolonged periods. Do isometric exercises to raise blood pressure before standing.
- Support blood pressure: Wear compression stockings or an abdominal binder to improve blood circulation and pressure.
What Are The Risk Factors For Orthostatic Hypotension
Orthostatic hypotension most often occurs in the elderly. “Hardening of the arteries” or atherosclerosis that develops as we age makes it more difficult for blood vessels to adapt quickly when necessary. As well, many of the diseases that are associated with orthostatic hypotension are progressive, with symptoms worsening with age.
Pregnancy is associated with orthostatic hypotension. As the pregnancy progresses, the volume of the circulatory system expands and blood pressure tends to fall. This may lead to lightheadedness when standing quickly. Blood pressure levels return to normal after delivery.
Excessive sweating due to physical exertion and exposure to heat are risk factors and potential causes of dehydration and symptoms of orthostatic hypotension. Patients who have other risk factors to develop orthostatic hypotension have an increased risk if they become even mildly dehydrated.
Chronic alcohol use and drug abuse are also risk factors for developing symptoms of orthostatic hypotension.
Read Also: Can Iwatch Monitor Blood Pressure