How Do You Risk Stratify And Provide A Risk Assessment
Regular risk assessment of patients with pulmonary hypertension is strongly recommended. A comprehensive risk assessment is required since there is no single determinant that provides enough prognostic information. The most important question to be addressed at every clinic visit, is the patient compatible with a good long-term prognosis ? To answer this question, a structured approach is needed, and all pulmonary hypertension specialists should have a checklist to help provide a comprehensive risk assessment:
Achieving low clinical risk also functions as the primary treatment goal, thus treatment should be tailored to achieve and maintain a low-risk status.
What Is Primary Pulmonary Hypertension
Primary pulmonary hypertension is high blood pressure in the lungs. Its a rare lung disorder in which the blood vessels in the lungs narrow and the pressure in the pulmonary artery rises far above normal levels. The pulmonary arteries carry blood from your body to the lungs where carbon dioxide is traded for oxygen.
Pulmonary hypertension is a serious, chronic disease that can lead to heart failure if its not treated.
Assessing Your Medical History
To help diagnose PAH, your doctor should assess your personal risk factors for the condition. For example, they should look for any conditions that might contribute to PAH or make the disease worse. You have an increased risk of PAH if you have:
- heart disease
- a family history of PAH
Your doctor may perform genetic screening to see if you have genes linked to PAH.
Your doctor may use the following methods to diagnose PAH:
Also Check: Spicy Food High Blood Pressure
Causes Of Miscellaneous Pulmonary Hypertension
- Blood Diseases: Certain blood diseases, such as bone marrow disease, are associated with pulmonary hypertension. Doctors postulate that, because these blood diseases cause the body to produce excess red blood cells, they can contribute to pulmonary hypertension.
- Systemic Disorders: Some systemic disorders cause a condition called vasculitis, a kind of inflammation that affects blood vessels throughout the body. Over time this can narrow blood vessels and restrict blood flow to vital organs and tissues, including the lungs, which can result in pulmonary hypertension.
- Tumors: Certain conditions cause tumors to develop in the lungs or chest. These tumors can press against the pulmonary arteries, restricting blood flow and causing pulmonary hypertension.
- Metabolic Disorders: Some metabolic disorders, including thyroid disorders, Gaucher disease, and glycogen storage disease, can result in pulmonary hypertension.
Ph Associated With Left Ventricular Diastolic Dysfunction
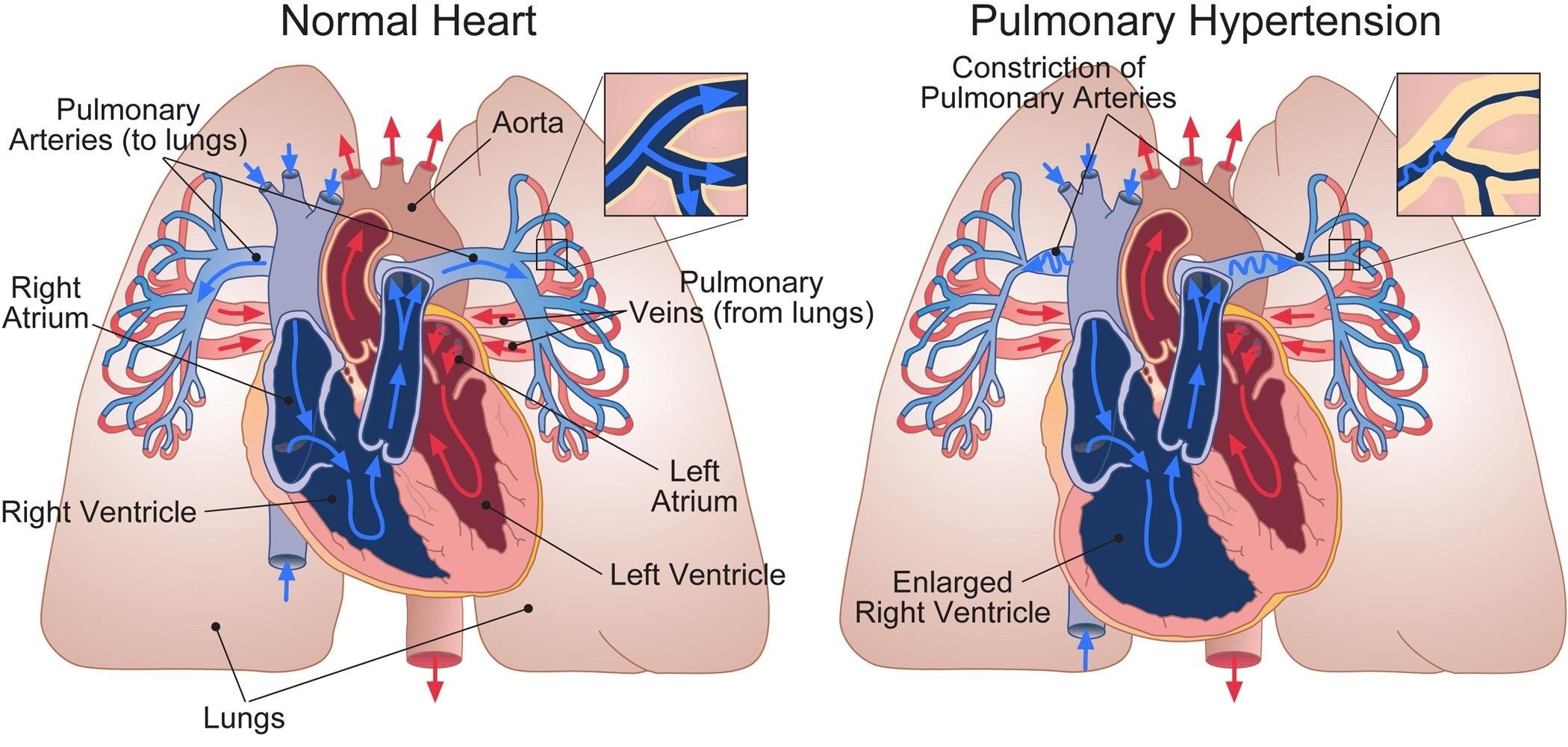
The heart cycle is divided into two phases, systole and diastole. Systole is when the heart is pumping blood out to the lungs and body. After the ventricles eject the blood they must relax and refill with blood to prepare again for pumping. This relaxation phase is known as diastole. The ventricles can become stiff over time not allowing the ventricles to fill completely with blood during diastole. The stiffness of the ventricles and inability to relax causes the pressure to rise on the left side of the heart, and eventually the pressure in the lungs rises. This condition is known as diastolic dysfunction. Diastolic dysfunction may occur with normal aging but is also associated with chronic high blood pressure, coronary artery disease and many forms of cardiomyopathies .
Diastolic dysfunction can only be diagnosed by heart catheterization. The data that the doctor obtains during the heart catheterization will help identify this type of heart disease. Although diastolic dysfunction is a form of pulmonary hypertension the treatment is different and the goal is to relax the left ventricle using specific drugs such as nitrates. It is also important to control the bodys blood pressure, treat coronary artery disease and control lung congestion with diuretics.
Recommended Reading: Do Onions Lower Blood Pressure
Living With Pulmonary Hypertension: Everything You Need To Know
Feb 28, 2018 6:51:41 AM / byDuke Reeves
Pulmonary hypertension is a serious, chronic disease that affects the heart and the blood vessels in the lungs. Although it is somewhat rare, the disease can result from a large number of health conditions, genetics, or even occur spontaneously.
Unfortunately, most cases of pulmonary hypertension are chronic and incurable. But especially with early diagnosis and proper medical treatment, people with the disease are able to manage the symptoms of pulmonary hypertension and maintain a good quality of life.
In the early stages of the disease, people who have pulmonary hypertension tend to experience fatigue and shortness of breath during physical activity. But symptoms worsen and multiply as the disease progresses.
Life expectancy and treatment options depend mostly on how early the disease was caught and what cause, if any, doctors can find for the disease. In this guide, we will help you better understand pulmonary hypertension, what causes it, and what kind of treatments options are out there to help patients manage the disease.
Pah Affects Women More Than Men
The idiopathic and heritable forms of PAH are at least twice as common in women compared to men, according to the Pulmonary Hypertension Association. In fact, PAH is most often diagnosed in women between the ages of 30 and 60.
It’s not currently known why females are more susceptible, but some theories under investigation have to do with the role of estrogen, changes that occur during pregnancy and links to autoimmune issues, which also tend to be more prevalent in women.
Read Also: Is High Blood Pressure Heart Disease
Taking Care Of Yourself
One of the best things you can do for yourself is to stay active, even if you have shortness of breath. Regular exercise, like taking a walk, will help you breathe better and live better. Talk to your doctor first to find out what kind of exercise is best for you, and how much you should do. Some people may need to use oxygen when they exercise.
Get plenty of rest, too. Pulmonary hypertension makes you tired, so get a good night’s sleep and take naps when you need to.
Just like anyone else, it’s good for you to eat a healthy diet with lots of fruits, vegetables, and whole grains. That’s important for your overall health.
A Symptom Diary Can Help
Start by keeping track of your symptoms in a diary or journal. It can be hard to notice when things change or gradually get worse. When you write down how you feel every day, you create a record you can review and share with your doctors. This way, you donât have to rely on your memory to recall when you felt dizzy, short of breath, or overly tired.
Note the symptom, the day, and the time you noticed it. A simple pen-and-paper system is fine, or you can keep track on your computer or smartphone. Many apps that help you keep tabs on your symptoms are free or low-cost.
Itâs also a good idea to keep track of your weight. If you quickly put on some pounds , it could mean your PAH is getting worse. Weigh yourself at the same time every day and write the number down.
However you do your diary, bring the information when you see your doctors.
Also, know what symptoms shouldnât wait for your next appointment. For example, if you have chest pain, fainting, or any problems that get worse, be sure to call the doctor.
Read Also: Do Onions Lower Blood Pressure
Confirming High Pressures In The Pulmonary Arteries
Normal pressure in the pulmonary arteries is between 11 and 20 millimeters of mercury when measured by cardiac catheterization. Your doctor may perform the following tests to confirm high pressures in the pulmonary arteries.
- Cardiac catheterization to provide a definite diagnosis of pulmonary hypertension. A diagnosis of pulmonary hypertension is made if the pulmonary artery pressure is 25 mm Hg or greater while at rest.
- Echocardiography to estimate pulmonary artery pressure. An estimated pulmonary artery pressure of 35 to 40 mm Hg or greater on echocardiography suggests pulmonary hypertension. A diagnosis of pulmonary hypertension may be made when enough changes are seen on an echocardiogram. If the echocardiogram suggests pulmonary hypertension, then right heart catheterization may be the next step.
What Are The Clinical Classifications Or Groups
Additional laboratory, diagnostic, and imaging tests are completed to further characterize the possible etiology of pulmonary hypertension. The additional tests include, but are not limited to:
- Blood tests and immunology
- High-resolution CT scan without contrast
- Pulmonary function test with arterial blood gases
- Sleep study
- Genetic testing, in select patients
At this point, all the information obtained from the RHC and additional testing listed above allows for categorizing into a specific WHO group. The clinical classification of pulmonary hypertension is intended to categorize multiple clinical conditions into five groups according to their similar clinical presentation, pathological findings, hemodynamic characteristics, and treatment strategy. The classifications or groups are defined by the World Health Organization and are referred to as WHO group 1-5:
WHO Group 1
- idiopathic, heritable, drug- or toxin-induced, and associated with connective tissue disease, HIV infection, portal hypertension, congenital heart disease, or schistosomiasis
- pulmonary veno-occlusive disease/pulmonary capillary hemangiomatosis
- diagnosing PAH requires exclusion of comorbid cardiac, lung, thromboembolic, and other diseases that predispose to increasing pulmonary artery pressures
WHO Group 2
- left ventricular systolic dysfunction, left ventricular diastolic dysfunction, valvular heart disease, or specific congenital abnormalities
WHO Group 3
WHO Group 4
WHO Group 5
Read Also: Onion And Blood Pressure
Caring For Someone With Pulmonary Hypertension
Pulmonary hypertension usually progresses slowly, and eventually results in shortness of breath and a decreased ability to perform the activities of daily living at home. For most of the course of the illness you will not need any extra assistance at home. However, at the end stage of pulmonary hypertension, you may need services such as home oxygen, council cleaning, and meals on wheels. These can be arranged through your GP or local volunteer services.
When Should I Call My Doctor About Pulmonary Hypertension
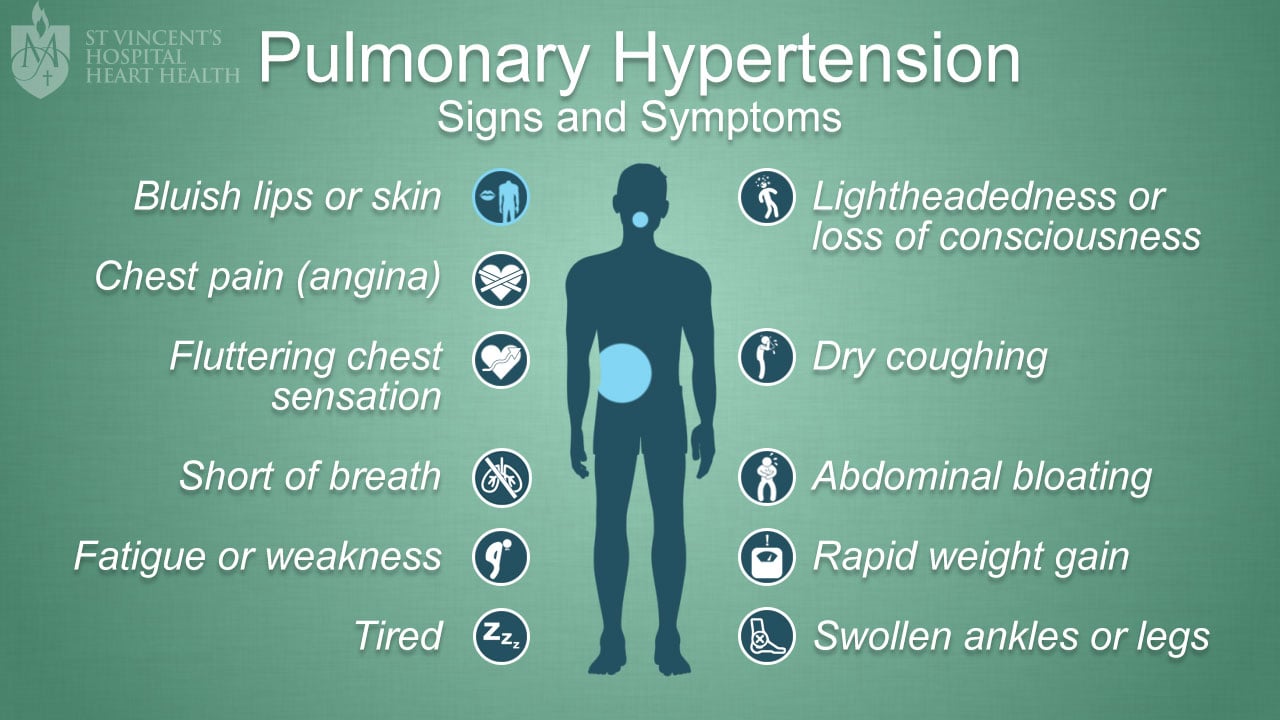
- Weight gain â 2 pounds in one day or 5 pounds in one week
- Swelling in your ankles, legs, or abdomen that has become worse
- Shortness of breath that has become worse, especially if you wake up short of breath
- Extreme fatigue or decreased tolerance for activity
- A respiratory infection or a cough that has become worse
- Fast heart rate
- Episodes of chest pain or discomfort with exertion that are not relieved with rest
- Difficulty breathing with regular activities or at rest
- Restlessness, confusion
Recommended Reading: Onions And Blood Pressure
When To See A Gp
See a GP if you have any symptoms of pulmonary hypertension. They may ask you about your symptoms and medical history, and they may carry out a physical examination.
Correctly diagnosing pulmonary hypertension can sometimes take time because its symptoms are similar to those of many other heart and lung conditions.
Tests you may have include a type of heart scan called an echocardiogram, and right heart catheterisation, where a thin, flexible tube is inserted into your pulmonary artery.
The changes in the pulmonary arteries that lead to pulmonary hypertension can be caused by:
- problems with the smaller branches of the pulmonary arteries
- conditions that affect the left side of the heart
- lung diseases or a shortage of oxygen in the body
- blood clots that cause narrowing or a blockage in the pulmonary arteries
Read more about the causes of pulmonary hypertension.
Follow Up Care For Ph
While it can take weeks to months to notice a significant improvement with medical therapy, it is important to follow up closely with your PH specialist to make sure that there is improvement.
Patients will follow up within three months of their diagnosis.
If they are doing well, they will follow up every six to 12 months for continued monitoring of their disease.
Follow up can involve repeat testing including:
- The six-minute walk test
Recommended Reading: Omron Bp785 Calibration
How Pulmonary Arterial Hypertension Is Treated
Although there is no cure for PAH, there are medications and procedures that can slow the progression of the disease and improve your quality of life. Treatment options vary from person to person, so you will want to work closely with your doctor to determine the best plan for you. Newly diagnosed patients with PAH should be referred to an accredited pulmonary hypertension care center for evaluation and right heart catheterization.
PAH-specific medications come in multiple forms: oral, inhaled and intravenous /subcutaneous. Intravenous treatments open up the blood vessels to help ease chest pain and shortness of breath. Subcutaneous treatments use a portable infusion pump to open up the blood vessels and ease PH symptoms. Inhaled treatments, such as prostacyclins, are primarily used to relieve shortness of breath.
There are a wide range of oral treatment options. Endothelin Receptor Antagonists prevent blood vessels from narrowing and are commonly used to help patients participate in physical activities. Phosphodiesterase Inhibitors allow the lungs to relax and the blood vessels to dilate. Prostacyclin Analogue, Selective IP Receptor Agonist, and Soluble Guanylate Cyclase Stimulators allow the blood vessels in the lungs relax.
Why Do The Pulmonary Arteries Narrow
Scientists believe that the process starts with injury to the layer of cells that line the small blood vessels of the lungs. This injury, which occurs for unknown reasons, may cause changes in the way these cells interact with the smooth muscle cells in the vessel wall. As a result, the smooth muscle contracts and grows more than is normal and narrows the vessel.
You May Like: Does Vodka Raise Blood Pressure
How Do You Define And Diagnose Pulmonary Hypertension
Pulmonary hypertension is defined by either a mean pulmonary artery pressure at rest of 20 mm Hg or more as measured by a right heart catheterization or a right ventricular systolic pressure of 30 mm Hg or more as measured by an echocardiogram. An RHC is the diagnostic gold standard and an essential component in the evaluation of pulmonary hypertension. While an echocardiogram can be a useful screening tool for the presence of pulmonary hypertension, it only provides an estimate of RVSP. An RHC is absolutely required to confirm the diagnosis, assess the severity of hemodynamic impairment, provide risk assessment, and guide pulmonary hypertension-specific therapy.
The threshold to perform a left heart catheterization in addition to an RHC should be low in patients with risk factors for heart disease and when the measurement of left ventricular end-diastolic pressure is important to avoid potential misclassification of pulmonary hypertension.
Ph Associated With Chronic Thromboembolic/embolic Disease
A thrombus or thromboembolism is a blood clot that blocks the passage of blood through a vessel. If blood clots travel to the lung, the obstruction may lead to pulmonary hypertension. Sometimes blood clots in the lungs do not cause symptoms. Pulmonary Hypertension caused by blood clots is rare and may require surgical removal of the clots by a procedure called thromboendarterectomy.
There are many diseases that can cause pulmonary hypertension . The following is a brief explanation of each of these conditions.
Read Also: Does Spicy Food Cause High Blood Pressure
Pulmonary Hypertension And Interstitial Lung Disease
Pulmonary hypertension, or PH, occurs when blood pressure within the lungs becomes abnormally elevated. It can be caused by a thickening of the pulmonary artery walls, heart failure, lung disease , and clots within the lungs’ blood vessels. It’s common for ILD patients to also develop pulmonary hypertension.
PH should not be confused with ordinary hypertension sometimes called systemic hypertension or high blood pressure. PH can occur in patients with or without ordinary hypertension.
PH in ILD is also a different disease than primary pulmonary hypertension also called idiopathic pulmonary arterial hypertension a rare condition in which PH develops in the absence of lung disease or any other known cause.
Pulmonary Hypertension Guidelines For Echo: And How To Measure Rvsp
You probably dont need to be told that echocardiography plays a major role in the noninvasive assessment of pulmonary hypertension. Echo is used to not only screen for the disease, but to determine right and left heart structure and function as well as monitor the progress of patients undergoing treatment for pulmonary hypertension.
Don’t Miss: Does Entresto Lower Blood Pressure
Pulmonary Hypertension And Sleep Apnea
The rare and severe lung disease called pulmonary hypertension affects the pulmonary arteries, causing high blood pressure. The pulmonary arteries transport the blood from the right heart ventricle to the lungs, but when affected by the disease, they become narrowed and thickened. The hearts of patients with pulmonary hypertension need to work harder to properly pump the blood, which make them enlarged, weakened, and more susceptible to complications that could include right heart failure.
The diagnosis, management, and prognosis of pulmonary hypertension are closely related to the causes of the disease but they are not completely understood. It can develop as consequence of alterations in the cells that line the pulmonary arteries with or without a known reason or as result of another condition.
Sleep apnea, a potentially severe sleep disease that makes patients stop breathing repeatedly for short periods of time while sleeping, is among the most common diseases that cause pulmonary hypertension.
Advancing Research For Improved Health
In support of our mission, we are committed to advancing pulmonary hypertension research in part through the following ways.
- We perform research. Our Division of Intramural Research, which includes investigators from the Sickle Cell Branch, is actively engaged in the study of pulmonary hypertension.
- We fund research. The research we fund today will help improve our future health. Our Division of Lung Diseases and its Lung Biology and Disease Branch oversee much of the research on pulmonary hypertension that we fund. Search the NIH RePORTER to learn about research the NHLBI funds on pulmonary hypertension.
- We stimulate high-impact research. Our Trans-Omics for Precision Medicine Program now includes participants who have pulmonary hypertension. This work may help us understand how genes contribute to differences in disease severity and to how patients respond to treatment, particularly in patients who have sickle cell disease. The NHLBI Strategic Vision highlights ways we may support research over the next decade, including research on pulmonary hypertension.
Learn about exciting research areas the NHLBI is exploring about pulmonary hypertension.
Also Check: What A Good Blood Pressure